Patients
Between March 2008 and November 2008,
39 patients scheduled for follow up coronary angiography with IVUS and 64-MDCT after coronary stent implantation were consecutively investigated.
Inclusion criteria for this study is male or non-pregnant female ≥18 years of age and those who had coronary artery disease treated by percutaneous coronary intervention with stent implantation and planned follow-up coronary angiography to evaluate ISR.
We excluded patient with the followings: renal insufficiency (serum creatinine ≥ 2.0 mg/dL),
contraindication to beta-blockers (3rd-degree AV block,
decreased left ventricular function,
asthma,
or severe chronic obstructive pulmonary disease),
previous allergic reaction to contrast,
those who had an acute coronary syndrome at the time of scheduled angiography,
atrial fibrillation,
refusal of patient.
All patients gave written informed consent to the study protocol,
which was approved by the ethical committee.
64-MDCT Technique
The 64-MDCT scanner (Brilliance CT: Philips Healthcare Systems,
Cleveland,
Ohio,
USA) was performed before conventional angiography.
Patients with a heart rate > 65bpm received 100mg of metoprolol orally 1hour before the scan.
The MDCT scanner had the following scan parameters: detector collimation 64 x 0.625mm,
table feed 19mm/sec (0.2 pitch),
gantry rotation time 0.42 sec,
tube voltage 120 kV,
and tube current 400-500 mAs (depending on patient body mass).
Contrast medium (80mL,
370 mg I/mL) was injected IV at 5 mL/s followed by a 40 mL saline flush at 4 mL/s.
The CT value of the area of interest in ascending aorta was monitored from the start of the injection.
As soon as the CT value in the ascending aorta reached 110 H,
scanning was initiated,
and the imaging of the entire volume of the heart was acquired during one breath-hold with simultaneous recording of the ECG tracing.
Axial images (slice thickness,
0.9 mm; increment,
0.45 mm) were reconstructed using a multisector reconstruction algorithm.
Using retrospective ECG gating,
we routinely performed reconstructions at 75% of the R-R interval.
If motion artifacts existed at these reconstruction,
another,
more optimal ECG phase was chosen to provide better image quality.
MDCT data analysis
An observer,
unaware of the results of coronary angiography,
assessed the MDCT data sets on both the original axial CT images and on curved muliplanar reconstruction.
The stent was considered to be patent,
when the distal run-off was present and contrast medium could be detected within the stent.
And ISR was considered to be present,
when the vessel distal to the stent implantation site was not visualized or massive low density area in the stent lumen was detected visually as compared with the reference vessels (the sites proximal and distal to the stent).
The vessels 5mm proximal and distal to the stent were evaluated.
For comparison with IVUS,
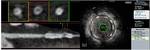
stent areas were measured in cross sectional image planes (Figure 1,
2).
Lumen area stenosis (%) was the difference between the stent CSA and the minimal lumen CSA divided by the stent CSA.
ISR was defined as ≥75% area stenosis in anywhere 5mm proximal and distal to the stent.
IVUS analysis
IVUS was performed with a 2.5F,
40-MHz or 2.9F,
20-MHz single-element mechanical transducer (Boston Scientific,
Volcano corp).
After intracoronary injection of nitrate,
the IVUS catheter was positioned at least 1cm distal to the stent.
IVUS images were recorded after initiation of pullback at 0.5mm/sec.
Experienced observer,
unaware of the results of MDCT reviewed and assessed IVUS image data.
The following IVUS parameters were measure: (1) minimal lumen cross sectional area (CSA,
mm2),
(2) minimal stent CSA (mm2) at minimal lumen CSA,
(3) minimal lumen diameter (mm),
and (4) stent diameter (mm) at minimal lumen CSA were measured.
And the area stenosis (%) was calculated (Figure 1,
2).
The percent area stenosis were comparable to 64-MDCT determined in cross sections with maximal in-stent lumen narrowing.
Binary ISR on IVUS was defined as maximum percentage of area stenosis ≥75% anywhere within the stent or within the 5mm proximal and distal to the stent.
Statistical analysis
Continuous variables are reported as means ± 1SD.
Sensitivity,
specificity,
positive predictive value,
and negative predictive value of MDCT for the detection of ISR using IVUS as the gold standard,
were calcultated.
Correlations were determined by calculating the Pearson correlation coefficient.
A value of p < 0.05 was considered statistically significant.
All continuous variables including stent CSA,
minimal lumen CSA and lumen area stenosis were evaluated using the paired T-test.
Binary data of presence or absence of ISR were evaluated using McNemar test.
Receiver operating characteristic (ROC) curves were calculated for minimal lumen CSA on 64-MDCT using IVUS (significant ISR defined as minimal lumen CSA < 4mm2 on IVUS) as the gold standard.