We identified 7 patients who had undergone sacral resection of a tumour involving the proximal sacrum,
with lumbo-pelvic reconstruction.
All patients were seen and treated after 2004.
The patient details and tumour types are shown in figure 2.
Mean tumour size on preoperative imaging was 10.7cm maximum diameter (range 6-16cm).
5 patients underwent total sacrectomy and 2 partial sacrectomy involving proximal sacrum and sacroiliac joint.
6 patients demonstrated adequate resection margins on histopathological examination,
although resection was deemed marginal for patient 4.
Postoperative follow up ranged from 10 to 46 months (figure 2).
A total of 76 imaging studies were reviewed (range 8-16 per patient).
These comprised 17 CTs (range 1-4 per patient),
17 MRIs (range 1-5 per patient) and 42 radiographs (range 2-10 per patient).
The earliest radiograph was performed 1 week after surgery,
the latest at 40 months.
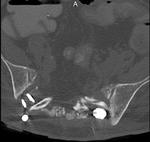
2 patients demonstrated small pelvic fluid collections up to 4 weeks postoperatively,
which were drained under ultrasound guidance.
This grew coagulase negative staphylococci in both cases.
A further 2 patients developed clinical signs compatible with infected metalwork in the late postoperative period,
with subsequent removal at 14 months and 23 months respectively.
No specific diagnostic features were demonstrated on imaging.
Coliforms and methicillin sensitive Staphylococcus aureus were cultured from one patient and extended-spectrum β-lactamase-producing (ESBL) Escherichia coli from the other.
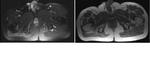
Changes in muscle appearances on MRI
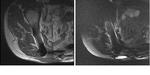
MRI changes in muscle signal and morphology were seen in 6 patients following operation.
5 patients demonstrated T2 signal hyperintensity between 10 and 20 months postoperatively and 4 patients displayed atrophy with fatty infiltration between 10 to 32 months postoperatively.
Muscle changes were seen predominantly within the gluteal musculature but also piriformis,
quadratus femoris and obdurator internus.
The distribution corresponded to nerve resection documented at surgery.
An example of this on MRI is provided in figure 3.
The remaining patient underwent right gluteal compartment resection as part of the initial resection of the right iliac and sacral osteosarcoma; no other muscle changes were evident on imaging.
Structural complications
Metalwork complications
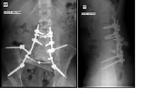
Rod fractures were observed in 4 patients,
the earliest instance at 9 months after instrumentation and the latest at 16 months.
Bilateral iliolumbar rod fractures were noted in 2 patients; the other two cases involved the left iliolumbar rod.
The fractures occurred at the lumbosacral curve in all but one case.
Two of these patients also demonstrated a concurrent fracture of the transverse connecting rod.
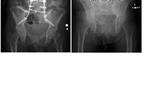
Figure 4 shows a radiograph with rod fracture.
Screw loosening with surrounding osteolysis around the iliac bolts was observed in 4 patients between 12 and 28 months after surgery.
This was associated with rod fracture in three patients and infected metalwork in one.
Graft complications
Bony graft incorporation,
as evidenced by callus formation and osseous bridging,
was assessed on plain radiographs and CT. In some cases,
the graft interface was obscured by metalwork on the standard AP and lateral radiographic projections and therefore only assessed adequately on CT.
All patients had at least one fibula graft in situ,
ranging from one to four strut grafts.
The earliest evidence of bone union was seen at 6 weeks.
Sites not showing evidence of incorporation by 5 months did not progress to bone union within the follow up period.
Images of union and non union are shown in figure 5.
There was an average rate of 55% non union at graft/bone interfaces in each patient (range 25- 83%).
Graft fractures occurred in 2 patients: transverse graft fracture occurred at 17 months following rod fracture in one case,
and a vertical graft fracture at 23 months in another patient.
Associated graft displacement was observed in both of these patients (figure 6).
The combined effect of graft and metal implant complications resulted in change in the morphology of the lumbo-pelvic junction,
with subsequent lumbar kyphosis and axial collapse in 5 patients (figure 7).
Disease recurrence
2 patients developed local tumour recurrence,
proven on biopsy and subsequent histology.
One patient with chordoma demonstrated local disease recurrence at 29 months postoperatively.
The patient with osteosarcoma developed local tumour recurrence at 6 months after surgery,
with subsequent development of pulmonary metastasis and liver metastasis despite chemotherapy.
The patient was deceased at 17 months into the follow up period.
The patient with spindle cell sarcoma developed pulmonary metastasis at 27 months without local recurrence and was deceased at 36 months post operatively.
Other complications
Bursa formation was identified over protruding instrumentation in 2 patients following movement secondary to graft or implant complication (figure 8).
Displacement of a fibula graft resulted in small bowel laceration in one patient.
This was obscured on CT by metal artefact.
The patient underwent laparotomy and repair at 32 months postoperatively.
The instrumentation was also removed at this time,
with evidence of infection on microbiological testing.