RESULTS:
Among the 984 MR images that were retrospectively reviewed,
81 MR images from 81 consecutive patients with tears at the rotator cuff footprint were included in our study (8.2%).
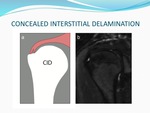
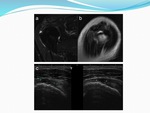
Thirty-two out of eighty-one (39.5%) footprint lesions were concealed interstitial delamination tears (Fig.
2). Most of the CID tears were located at the supraspinatus tendon (14 patients out of 32 patients with CID tears).
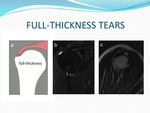
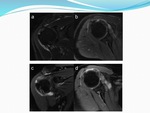
Full-thickness tears (Fig.
3) accounted for 25 out of 81 (30%) lesions.
Full-thickness tears were predominantly located at the supraspinatus tendon (20 patients out of 25 patients with full-thickness tears),
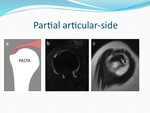
and 14 and 10 out of 81 (17.2% and 12.3%) lesions were PASTA (Fig.
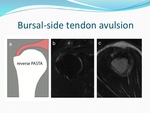
4) and reverse PASTA (Fig.
5), respectively,
most of them located at the supraspinatus tendon.
Ultrasound imaging was performed in 25 patients at a later time.
The period between the MR and ultrasound imaging was 1 day and 2 years and 3 months.
There is no changes in the ultrasounds findings in 12 patients. Ultrasound showed no changes in 12 patients (Fig.
6) and showed an increase of the injury in eight patients (Fig.
7).
No correlation between MRI and ultrasound imaging was found in five patients (MRI found CID whereas the ultrasound was normal in three patients and showed focal tendinopathy in two patients).
A Constant Score was obtained for 32 patients.
Of these 32 patients,
16 gave a value of 5 or less for pain (50%) and 25 gave a value of 10 or less for pain (78%).
These findings suggest that tears at the rotator cuff footprint are often associated with the presence of symptoms.
Of these 32 patients,
only 8 gave a value of 15 (no pain).
DISCUSSION:
Rotator cuff (RC) disease is the most common cause of shoulder pain and dysfunction in adults.
Tears occurring at the RC can be classified into partial-thickness or complete tears,
where partial-thickness tears can be located on either the bursal or the articular side.
Lesions involving the mid-substance of the tendon are called interstitial or intrasubstance tears.
It has been reported that most of the tears occur in a region about 1 cm medial to the tendon insertion,
the so-called “critical zone”.
In 1934,
Codman described a type of tear where tendon fibres were torn at the bony attachment at the greater tuberosity,
which he called “rim-rent” tears [1].
“Rim-rent” tears were defined as partial-thickness tears occurring on the articular side of the rotator cuff at the tendon insertion on the greater tuberosity.
A more anatomical description of this type of tear is a partial articular-sided supraspinatus tendon avulsion (PASTA) lesion,
which is virtually synonymous with rim-rent tears.
Only a few radiological publications concentrated on the imaging of tears at the rotator cuff footprint [2,
3].
A more detailed anatomical description of this type of tear was recently reported by Schaeffeler et al.
and called “tears at the rotator cuff footprint”,
which represents the region of humeral insertion of the supraspinatus and infraspinatus tendons [4].
The incidence of tears at the rotator cuff footprint in our population was 81 out of 984,
or 8.2%,
similar to that reported by Vinson et al.,
who found a total of 49 rim-rent tears in 200 consecutive shoulder MRIs.
The results of our study support the theory that tears at the rotator cuff footprint are not an uncommon type of tear.
Most of the footprint lesions in our study were CID lesions (39.5%),
but full-thickness tears accounted for 30% of all lesions at the footprint.
Our results are similar to those of Vinson et al.,
and also suggest that bursal-sided partial-thickness tears are less common than previously believed,
constituting only 12.3% of all rotator cuff tear at the footprint in our study.
It was mentioned that preoperative MR imaging is helpful in drawing attention to the presence of a concealed tear that might otherwise be missed on arthroscopic inspection.
Little is known of the natural history and spontaneous healing of partial tears.
Codman’s assertion that spontaneous healing occurs has not been substantiated by histological examinations [1].
In a series of 35 en-bloc histological sections from surgical specimens of partial tears,
Fukuda et al.
observed no active repair in any portion examined [6].
Yamanaka and Matsumoto undertook an arthrographic follow-up over 2 years on 40 joint-side tears that had not been operated on,
and found that 10% had decreased in size and 10% had disappeared,
but the remaining 80% became larger or progressed to full-thickness lesions [7].
During our study we observed eight cases that were treated conservatively and showed progression on ultrasound.
Since making this observation,
we also noted that many full-thickness rotator cuff tears at the footprint appear on imaging as if they had originated as partial tears at the footprint and then progressed to involve the full thickness of the tendon.
This observation supports the progression theory and underlines the importance of diagnosing partial-thickness rotator cuff tears.
Arthroscopy has enabled the visualization of partial thickness tears on the joint and bursal sides.
However,
the diagnosis of intratendinous tears still remains elusive.
The indications for the surgical treatment of partial thickness tears have not been clearly delineated.
Surgical treatment is generally considered for patients with symptoms of sufficient intensity and duration and in whom imaging suggests the presence of partial or small full-thickness lesions.
Surgery may involve debridement of the partial tear,
acromioplasty alone,
acromioplasty and debridement,
or repair of the cuff in addition to acromioplasty.
Our study has several limitations.
First,
the design of the study is retrospective.
Second,
we used MRI instead MR arthrography.
Third,
not all of our patients underwent arthroscopy.
Therefore,
the findings of rotator cuff tears were not correlated with the gold standard.
Moreover,
in some cases,
the time between the realization of MRI and ultrasound was not enough to draw any conclusions about the evolution of the tears.