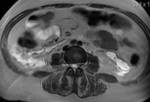
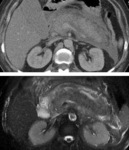
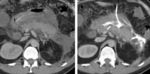
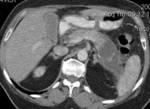
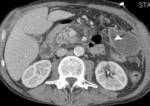
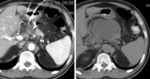
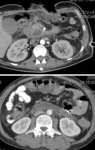
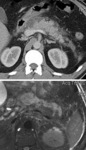
Inflammation changes in retroperitoneal fat were obtained on CT and MRI images of all 200 patients.
In 122 cases forming the fluid collection were detected.
In 78 cases the retroperitoneal fat inflammation came to nothing more than infiltration.
To distinguish changes between fluid and infiltration we carried out the MRI (in 16 cases).
(fig 4)
As the prevalence of peripancreatic changes all the patients were divided into groups.
In group #1 were combined 80 patients with limited peripancreatic changes.
In 72 patients in this group used only the conservative treatment.
In 8 cases was conducted US guided drainage.
In 1 case the outcome of the changes was a pseudocyst.
Which subsequently (after 1 year) decreased in size in half.
In other cases,
changes disappeared,
no effects were observed.
In group #2 were combined 46 patients with extended changes.
Patients in this group was under dynamic CT.
Dynamic imaging included 5 - 7 CT studies with an interval of 7 - 10 days,
according to a standard protocol,
adopted in our clinic.
There has been a tendency to increase in the collections size during the first week of the disease.
In 40 patients of group №2 in the collections were discovered fat inclusion.
The availability of plots of fat density is often combined with the inefficient collecton drainage,
which was the ground for the MRI,
which clarifies the presence of solid mass of debris.
(fig 5).
In the case of contraindications to MRI 8 patients CT fistulography was performed,
which demonstrated similar information.
(fig 6).
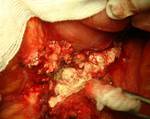
During the intraoperative revision of the extended changes always identified numerous areas of fat necrosis. (fig 7).
36 patients were performed percutaneous ultrasound guided drainage collection,
which was at the same time,
and diagnostic and therapeutic procedures.
The infection was confirmed by bacteriological tests in 28 cases.
Only in 6 patients in not drained collections were found gas bubbles.
In 22 cases,
percutaneous drainage was a final method of surgical treatment.
In 14 cases,
the drainage was performed in the stage of surgical treatment.
In 12 patients collection were further incapsulated and on this place were formed pseudocysts,
which had been removed in 4 cases,
in 8 cases regressed.
In 8 cases in the cysts soft tissue density inclusions were detected.
(fig 8).
In 9 cases there was the development of abscesses.
In all abscesses the drainage was performed successfully.
(fig 9).
In this study identified the following places of the collection localizations:
Typical ways of exudate spreading:
- Along the front sheet renal fascia on the right (in 22 cases)
- Along the front sheet renal fascia on the left (in 58 cases)
- Central type of the spreading.
Most frequently to the mesokolon transversum.
Central only.
(in 16 cases) With other types combined (in 63 cases).
More rare ways of exudate spreading:
- Perirenal spatium (inwards from renal fascia) on the right (in 14 cases)
- Perirenal spatium on the left (in 3 cases)
- Retronefrium spatium on the right (in 12 cases)
- Retronefrium spatium on the left (in 5 cases)
- In 18 cases we detected a single large collector in the bursa omentalis,
which was successfully drainaged in all cases.
(fig 10)
We also had been observing the most difficult to allow for drainage places.
Behind the head of the pancreas (in 12 patients).
Central localization,
on the abdominal vessels (in 11 patients).
(fig 11)
20 patients in whom there's extensive exudate prevalence up to the small pelvis were combined in a group #3.
All patients experienced a development of organ failure of at least one of the systems.
All patients in group #3 underwent staged surgical management.
Lethal outcome was in 6 cases.
Most often (in 146 cases) in the first three groups were detected foci of pancreatic necrosis which were located under a pancreas capsule.
(fig 12a) MPR CT and MRI always identify the relationship with the capsule.
(fig 12b)
In group №4,
consisting of 28 patients were included patients with large-areas,
total or subtotal pancreatic necrosis.
These patients have not expressed spread of the exudate.
15 patients had isolated the limited collectors.
In the 16 cases were formed liquid collections n the projection of the pancreas.
In 14 cases,
the collections were drained.
In the rest of the cases were made of various sizes resections.
In 7 patients with extensive edema and increased pancreas was observed bilious hypertension.
As well as were found 4 patients,
who had an increase in gland and reducing its density.
In this they have been observed infiltration in all retroperitoneal and peritoneal spatium and multiple organ failure.
Noted that the right-hand type the spread of the exudation was combined with the concrements in the biliary system.
As a result of the research we have developed the following algorithm of CT and MRI diagnostics of acute pancreatitis:
- MDCT with bolus contrast in the day of receipt of the hospital.
- MDCT with bolus contrast every 3 days within the first 10 days of the disease.
- Scheduled MDCT before and after each stage of surgical intervention
MRI should be performed;
- To differentiate of infiltration and liquid content
- If not efficiency drainage to identify the size and localization sequestered tissue
We also have developed a standard protocol for describing CT and MRI studies in acute pancreatitis in which should describe the belonging of the one of described groups.
The efficiency of application of the new diagnostic approach was assessed in the course of the year.
Severity condition and the time of hospital admission patients whom applied the new approach were significantly lower.
Also in this group decreased the need for surgical interventions.