1.
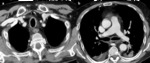
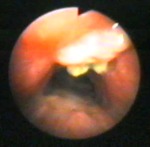
Aspergilloma
Aspergilloma is an Aspergillus infection in immunocompetent host.
The organism causes mild or no reaction and tissue invasion does not occur.
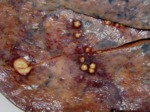
Histopathologically an aspegilloma is a conglomeration of hyphae,
mucin,
fibrin and inflammatory cells in a preexisting pulmonary lesion such as bronchiectasis,
cavity,
bullae or a site of prior surgery.
Fig. 2
The most common underlying causes are tuberculosis,
sarcoidosis and emphysema but it is also possible to find them in patients with bronchiectasis,
pneumoconiosis,
fibrotic lung disease,
neoplasm,
pulmonary infarction,
bronchogenic cyst,
pulmonary sequestration and pneumatoceles secondary to Pneumocystis jirovecii pneumonia.
Although the lesion is usually single,
it can present as multiples ones and it occurs predominantly in the upper lobes.
The most common clinical manifestation of aspergilloma is hemoptysis,
which can reach life-threatening proportions causing death in approximately 5% of patients.
However,
it may also exist for years without causing any symptoms and,
therefore,
its diagnosis can be made as an incidental finding on a routine chest radiograph.
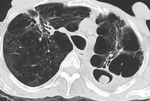
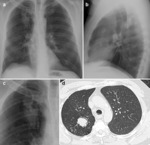
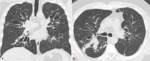
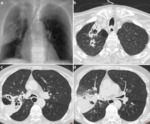
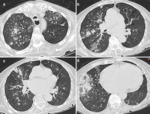
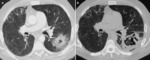
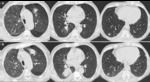
Chest radiographs and CT scans show a lung cavity containing a solid rounded mass which is separated from the wall by a rim of air.
This feature is called the “air crescent” sign. Fig. 3
Another common feature is the thickening of the cavity wall and the adjacent pleura.
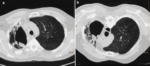
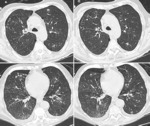
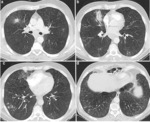
This fungus ball may be mobile.
The changing of the position of the mass within the cavity,
which can be easily demonstrated by rotating the patient in the CT scan,
is a finding that can orientate the diagnosis.
Fig. 4
The differential diagnosis includes hematoma,
neoplasm,
abscess,
hydatid cyst and Wegener granulomatosis.
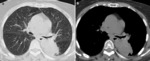
An unusual form of aspergilloma is the one found in patients without preexisting lung cavities which presents as a localized consolidation or as a single nodule or mass with or without an air crescent sign.
In these cases,
differentiation from malignancy or from other chronic infection is radiologically not possible.
Fig. 5
2.
Allergic bronchopulmonary aspergillosis (ABPA)
This entity is characterized by the presence of fleeting dense plugs of mucus,
hyphaes and eosinophils in lung parenchyma due to deposition of immune complexes and inflammatory cells within the segmental and subsegmental bronchi.
ABPA represents a hypersensitivity reaction to Aspergillus occurring almost exclusively in long-standing bronchial asthma patients and occasionally as a complication of cystic fibrosis
Clinically,
patients with ABPA experience wheezing,
cough and fever.
Eosinophilia and elevated serum IgE levels are typically found and they can suggest the diagnosis.
Approximately 20%-60% of patients refer thick mucous plug expectoration in which hyphal fragments can be demonstrated at culture or histologic analysis.
Initial radiologic manifestations are transitory pulmonary opacities secondary to the deposition of immune complexes and inflammatory cells in the alveoli.
With time,
an irreversible damage occurs to the bronchi with dilatation,
wall thickening and mucus plugging.
CT findings include tubular or saccular finger-in-glove areas of increased opacity in a bronchial distribution representing mucus plugging within bronchiectasis,
predominantly involving the upper lobes.
In approximately 30% of patients,
the impacted mucus has high attenuation or demonstrates calcification at CT.
These central tubular bronchiectasis are so highly suggestive of ABPA that are considered the distinguishing mark of the disease.
Fig. 6
The diagnosis is made by a combination of criteria,
of which episodic asthma exacerbations,
transient or fixed pulmonary infiltrates,
central bronchiectasis,
peripheral blood eosinophilia,
elevated serum IgE levels and positive Aspergillus precipitins are the most important.
3. Chronic necrotizing pulmonary aspergillosis (CNPA)
Chronic necrotizing pulmonary aspergillosis (CNPA),
also known as semi-invasive aspergillosis,
is a local and more indolent form of invasive pulmonary aspergillosis that commonly runs progressive over a period of weeks or months and characteristically happens in mildly immunocompromised patients or patients with a chronic disease that predispose them to infection.
Risk factors include diabetes mellitus,
alcoholism,
pneumoconiosis,
collagen vascular disorders,
chronic obstructive pulmonary disease (COPD),
previous radiation therapy,
malnutrition,
myocardial infarction and low-dose steroid use.
Histologically it is characterized by the presence of tissue necrosis and granulomatous inflammation similar to that seen in reactivated tuberculosis.
CNPA presents clinically always with constitutional symptoms.
These can be the only manifestation or can be associated with chronic productive cough or with hemoptysis,
which varies from severe to trivial.
Radiologically,
CNPA appears typically as a chronic consolidation or as multiples nodules with progressive cavitation in one or both upper lobes.
These findings are non-specific,
most commonly mimicking those of mycobacterial infection.
Fig. 7
In some patients,
lesions are more peripheral,
associate pleural thickening and may progress to form a bronchopleural fistula.
4. Invasive pulmonary aspergillosis (IPA)
It is a relatively common life-threatening complication with a mortality rate reported in published series of up to 85%.
It occurs in severe immunocompromised patients,
especially in those with neutropenia due to hematologic malignancies,
chemotherapy or immunosuppressive therapy. Usually,
they develop the disease after a 2-3-week period of profound neutropenia,
with an absolute neutrophil count < 500 cells/mm3.
Depending on the route of spread we can discern two kinds of invasive aspergillosis; angioinvasive and airway invasive,
which can even coexist in the same patient.
However,
this is just a histological and etiopathogenical distinction as,
in the clinical practice,
this is not relevant for therapy.
Both airway-invasive and angioinvasive aspergillosis have similar clinical symptoms and usually patients experience fever,
cough and progressive dyspnea.
Angioinvasive aspergillosis is histologically characterized by invasion of small to medium-sized vessels by fungal hyphae.
This results in thrombus formation and vascular occlusion with the consequent tissue necrosis and systemic dissemination.
These hemorrhagic infarcts are seen in CT scans as small nodules and/or small pleural-based,
wedge-shaped consolidations with a surrounding halo of ground-glass attenuation (halo sign).
The halo sign represents alveolar hemorrhage.
Fig. 8 Fig. 9
The CT halo sign is a highly sensitive predictive sign of early IPA so a CT must be performed immediately at the slightest suspicion of the disease in neutropenic patients.
As the disease progresses the nodules may cavitate,
the necrotic parenchyma detaches from the adjacent lung forming an air crescent similar to that seen in aspergilloma.
This sign is usually found later in the course of the disease,
usually 2–3 weeks after initiation of treatment,
when the patient is recovering from neutropenia and it is considered a good prognostic sign.
Fig. 10
In the right clinical context,
nodules or consolidations surrounded by a ground-glass halo,
progressing to cavitation or air crescent formation are considered typical of angioinvasive aspergillosis.
Fig. 11
Invasive aspergillosis of the airways accounts for 14%-34% of cases of invasive aspergillosis and includes bronchitis and bronchiolitis,
bronchopneumonia and lobar pneumonia without evidence of vascular invasion.
It is characterized at pathological examination by the presence of Aspergillus deep to the airway basement membrane of bronchi or bronchioles,
generally with demonstrable hyphae in the involved airway and accompanied by a neutrophilic reaction.
Surrounding the involved airway there is often a variably sized zone of hemorrhage and/or organizing pneumonia.
In the majority of cases,
radiographic findings of invasive aspergillosis of the airways appear as patchy peribronchial consolidation or as centrilobular nodules and,
in some cases,
as areas of tree-in-bud pattern.
Fig. 12 Fig. 13
These features are non-specific and are indistinguishable from those of bronchopneumonia caused by other microorganisms.
A special subtype of airways invasive aspergillosis is acute tracheobronchitis,
also known as pseudomembranous tracheobronchitis,
which represents 5% of the cases of IPA.
This uncommon manifestation affects almost exclusively lung transplant recipients and AIDS patients.
Infection is mainly limited to the tracheal and bronchial walls with varied degrees of invasion of the mucosa,
submucosa and cartilage but without lung tissue involvement.
Patients experience cough,
dyspnea and hemoptysis but they can also be asymptomatic which can delay the diagnosis and facilitate the progression of the infection to small airways from where lung parenchyma it is easily reached.
CT scans are usually normal; sometimes a non-specific tracheal wall thickening is the only evident finding.
Fig. 14
Bronchoscopy and fungal culture of the sputum proportionate a definitive diagnosis.
Fig. 15