Between January 2011 and December 2011 we prospectively studied 26 consecutive Patients (mean age 45 years old; range 29;74 years old) referred for MR imaging of the inferior abdomen by gynecologists.
Among these 7/26 presented endometriosis,
12/26 uterus cancer,
4/26 adnexal pathology and 3/26 resulted with no pathology.
MR imaging was performed on a 1.5T scanner (Magnetom Symphony,
Siemens,
Erlangen,
Germany),
using a pelvic phased array coil.
To reduce bowel peristalsis,
the patients were asked to fast 4-6 hours before the examination and 1 mg of butylscopolamine (Buscopan,
Schering,
Germany) was administered intramuscularly in all patients,
10 minutes before the beginning of the examination.
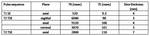
Axial T1-weighted Spin Echo (SE) images were obtained with the following imaging parameters: TR/TE 520/9.3 msec,
1 Average,
FOV read 320 mm,
4 mm section thickness and 1 mm interslice gap.
Sagittal T2-weighted Turbo Spin Echo (TSE) images were obtained with TR/TE 6040/90 msec,
4 Averages,
FOV read 330 mm,
3 mm slice thickness,
1 mm interslice gap.
Subsequently axial T2-weighted TSE images,
with TR/TE 5520/106 msec,
2 Averages.
FOV read 320 mm,
4 mm slice thickness,
1 mm interslice gap,
and coronal T2-weighted TSE images,
with TR/TE 3870/101 msec,
2 Averages,
FOV read 320 mm,
3 mm slice thickness,
1 mm interslice gap,
were obtained respectively perpendicular to and parallel to the endocervical canal.
Furthermore axial T2-weighted TSE images,
with use of body coil,
were obtained from the level of the thin-section axial images to the level of the renal hila,
with 7 mm slice thickness and 1 mm interslice gap,
for evaluation of paraaortic lymphadenopathy ( Table 1 ).
Two radiologists analyzed all the MR images in order to investigate the topographical anatomy of the pelvic fasciae.
The pelvic visceral peritoneum was divided into three groups of fasciae,
partially fused together: the parietal pelvic fascia,
the visceral pelvic fascia and the extraserosal pelvic fascia (5).
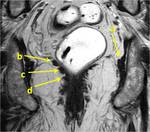
The parietal pelvic fascia covers the anterior surfaces of the sacrum and the coccyx and the structures contiguous to the pelvic walls.
Its muscular component includes the elevator ani,
the internal obturator, the coccigeo and the piriform muscles,
that usually appears hypointense on T2-weighted images ( Fig. 1 ).
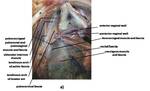
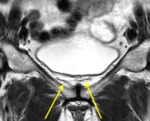
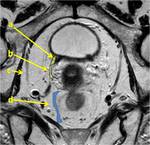
In this connective tissue we can identify two important bilateral surgical landmarks: the tendinous arch of pelvis fascia (1,6),
a whitish line stretching from the pubic bone and symphysis to the ischial spine,
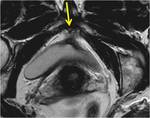
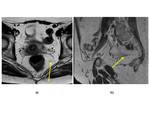
( Fig. 2 ; Fig. 3 ) and the pubo-vescical ligament (5),
tauted between the pubic symphysis and the bladder neck ( Fig. 4 ; Fig. 5 ),
that appear hypointense on T2-weighted images.
The visceral pelvic fascia envelopes all the visceral organs,
binding them to the pelvic walls.
It is normally divided into fasciae of individual organs (vescical,
vaginal and rectal fascia),
pubo-cervical fascia,
recto-vaginal fascia and recto-sacral fascia.
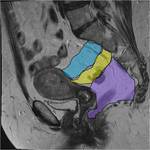
Furthermore two bilateral important ligaments can be appreciated: the utero-sacral and the recto-vaginal ligaments ( Fig. 6 ).
These two ligaments with the rectal stalks and the recto-sacral fascia constitute a single connective fascial block that prevents the prolapse of the pelvic organs during movements ( Fig. 7 ).
The extraserosal pelvic fascia is formed by the parametrio,
the paracervix,
the superior vescical ligament,
the lateral ligament of rectum and the presacral fascia (5).
It is considered like a support to the neuro-vascular structures of the pelvis and permits the physiological movements of each organs ( Fig. 8 ).
All these connective structures are in effect useful anatomical landmarks in the gynecologic pelvic surgery for both benign and malignant conditions.