MATERIALS AND METHODS
FOCAL CRYOTHERAPY
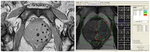
Six patients with localized prostatic carcinoma underwent Focal Cryosurgical Ablation.
The planning of the treatment was based on byoptic and preoperative MR imaging evaluation of size and position of the neoplastic lesions.
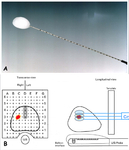
All cryoablation procedures were performed using four cryoprobes (SeedNet,
Galil Medical) (Fig.
1).
Cryoprobes were placed percutaneously,
using endorectal sonography guidance,
with the aid of a needle-spacing template (Fig.
1,
Fig.
2).
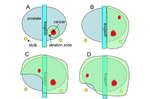
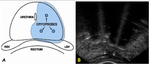
Patients were treated with hemiablation in five cases (the freezing zone enclosed half of the prostate parenchima with a margin of about 5 mm,
taking care of the periurethral zone in order to spare the urethra; the ablation zone was extended to include ipsilateral neurovascular bundle and margin,
for the treatment of possible extracapsular extension of disease).
In one case we treated only the lesion,
located in the central gland (Fig.
3).
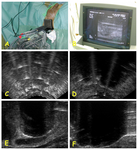
The development of the ice ball was controlled under ultrasound evaluation (Fig.
2,
Fig.
4).
Patients were followed up clinically,
biochemically and by MR imaging 24 hours after surgery,
and subsequently after 3,
12 and 24 months.
All examinations were performed with a 1.5T MR system (Philips Gyroscan Intera Power) using the body phased-array coil.
Imaging protocol included axial Gradient Echo (GRE) T1w,
Turbo Spin Echo (TSE) T2w sequences and contrast-enhanced (ce) TSE fat-suppressed (FS) T1w sequence.
TSE T2w and ce TSE T1w images were also obtained in the sagittal and coronal planes.
Post contrast TSE FS-T1w images were evaluated before and after digital subtraction procedure.
We evaluated the following parameters: A.
Morphology of the gland; B.
Signal intensity of the treated areas; C.
Patterns of vascularization of the treated areas.
FOCAL BRACHITHERAPY
5 patients with localized prostatic carcinoma underwent Focal Brachytherapy.
The planning of the treatment was based on byoptic and preoperative MR imaging evaluation of size and position of the neoplastic lesion.
Seeds were placed percutaneously with perineal approach,
using endorectal sonography guidance,
with the aid of a needle-spacing template (Fig.
5).
Ablation zone is extended to include ipsilateral neurovascular bundle and margin (treatment of possible extracapsular extension of disease) (Fig.
6,
Fig.
7).
Patients were followed up clinically and biochemically (PSA).
MR imaging follow-up was performed at 30 days and 12 months after therapy.
24hours after the treatment a radiographic evaluation of the pelvis was performed in all the patients,
tho evaluate number and position of radioactive seeds (Fig.
8).
30 days after the treatment a morphological MR study was performed for post-implant dosimetric evaluation,
using a 1.5T MR system (Philips Gyroscan Intera Power).
The post-plan dosimetries were based on unenhanced T1w (to locate the radioactive sources) and T2w (to visualise the prostate) imaging,
obtained using a phased-array body coil (Fig.
9).
Post-implant dosimetry was estimated on fused transverse T1w and T2w MR images: a dedicated Treatment Planning System (Variseed 7.0,
Varian) with an image fusion software,
was used to perform dosimetry (Fig.
10,
Fig.
11).
12 months after tretment was performed a MR imaging follow-up with a 1.5T MR system (Philips Gyroscan Intera Power) using the endorectal coil.
All the patients underwent MR conventional multiplanar Turbo Spin-Echo (TSE) T2w sequences,
followed from dynamic axial contrast enhanced (ce) Gradient-Echo (GRE) T1w sequence.
On MR images performed 30 days after the treatment we evaluated the morphology of the gland,
the seeds position and the post implant dosimetry.
On MR images performed 12 months after the treatment we evaluated the morphology and the patterns of vascularization of the gland.
IMAGING FINDINGS
FOCAL CRYOTHERAPY
Twenty-four hrs after treatment the treated areas were about 10 mm larger than the original gland (Fig.
12,
Fig.
13,
Fig.
14,
Fig.
15).
MR examinations showed a mean decrease in size of the treated areas of 30% after 3 months,
70% after
Twenty-four hours after cryoablation,
T2w images showed the prostate parenchima heterogeneously iso-hyperintense,
without significative differences between the treated and the spared zone of the gland.
The margins of the gland came out as poorly defined,
without perilesional rim (Fig.
12,
Fig.
13,
Fig.
14,
Fig.
15).
After 3,
12 and 24 months follow-up treated tissue showed high signal intensity on T2w images,
with a sharp hypointense perilesional rim Fig.
14,
Fig.
15)..
All the patients showed persistence of isointensity of the spared prostatic tissue.
The margins of the gland in correspondence of the treated areas resulted well defined Fig.
14,
Fig.
15).
Post treatment ce-FS T1w and subtracted ce-MR images showed ischemia of the treated zone of the gland,
hypointense as compared with normal prostatic parenchyma,
and relative enhancement of the untreated gland (Fig.
12,
Fig.
13,
Fig.
14,
Fig.
15,
Fig.
16).
CLINICAL FOLLOW-UP
All the patients had a stable PSA level (range 0.2–1.4 ng/mL) 24 months after the treatment.
No patient had clinically documented urinary complications related to the procedure.
MR imaging follow-up revealed no evidence of local or nodal recurrence in all the patients.
FOCAL BRACHITHERAPY
In all the patients,
a radiographic evaluation of number and position of radiation therapy seeds was perfomed at 24 hrs after the treatment (Fig.
8).
30 days after treatment,
prostate resulted more than 5 mm larger than the original gland (Fig.
9) on morphologic T1w and T2w MR images (Fig.
5).
MR examinations showed a mean decrease in size of the gland of 50% at 12 months after the treatment (Fig.
17)
30 days after focal brachytherapy procedure,
T2w images showed the prostate parenchima heterogeneously iso-hyperintense,
without significative differences in terms of signal intensity between the treated and the spared zone of the gland.
The margins of the gland resulted poorly defined,
without perilesional rim (Fig.
9).
Radiation therapy seeds were seen on GRE T1w image as small focal signal intensity voids (Fig.
9,
Fig.
10,
Fig.
17,
Fig.
18).
At 12 months imaging follow-up,
MR evaluation showed reduction in size of the gland,
with diffuse reduction in signal intensity on T2w images and contrast enhancement on dynamic ce GRE T1w images of the treated areas,
due to parenchimal fibrosis and atrophy.
All the patients showed persistence of isointensity of the spared prostatic tissue.
The margins of the treated areas resulted poor defined (Fig.
17).
CLINICAL FOLLOW-UP
PSA level decreased in all the patients at 12 months after the treatment (mean PSA level 2,2 ng/mL).
No patients had clinically documented urinary complications related to the procedure.
MR imaging follow-up revealed no evidence of recurrence in all the patients.