Ultrasound examination is usually the first line method of choice,
used when liver laboratory results are not clear,
because its quickness and easiness.
CT is a widely accepted method for diagnosing liver lesions but it has some disadvantages,
such as radiation exposure or,
in rare cases,
allergic reaction to iodinated contrast.
MRI has become a very effective method for detecting,
locating and characterizing liver lesions,
becoming the non-invasive diagnostic procedure of choice,
and does not expose the patient to any radiation at all.
Cirrhosis
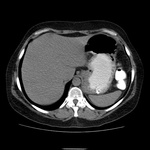
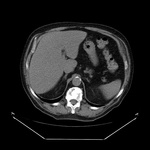
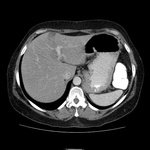
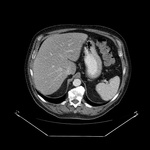
In CT scans,
liver may be normal in early stages,
whereas in later stages it could be seen a heterogeneous attenuation due to spotted fatty infiltration and irregular fibrosis,
showing lobulated edges caused by atrophic areas and regenerative nodules.
When intravenous (iv) contrast media is administrated,
a heterogeneous enhancement is shown.
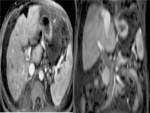
MRI evaluates morphological changes in a cirrhotic liver,
allowing not only detecting and characterizing focal lesions,
but also non-invasively evaluating intra and extrahepatic vessels.
It also helps in differentiating regenerative nodules from small dysplastic siderotic nodules and hepatocellular carcinoma (HCC).
Vascular complications such as portal thrombosis,
cavernoumatous transformation of the portal,
development of varicose veins and porto-systemic shunts,
and tumor invasion are easily demonstrated on MRI examinations,
avoiding using invasive procedures.
Fatty liver
In CT scans,
fatty liver infiltration decreases the attenuation of the affected parenchyma,
with values lower than 40 HU,
or at least 10 HU less than the spleen,
while blood vessels pass without any changes through the fatty infiltration area.
With the contrast media it is difficult to appreciate the fatty change due to the variability of the exploration time and the fact that the maximum liver enhancement is delayed when compared to the splenic one.
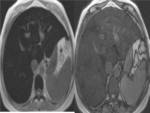
MRI is used in gradient echo sequences (GRE),
in-phase and out-phase (chemical shift),
where a signal drop is observed in out-phase sequences.
It also allows differentiating focal steatosis or a focal fatty infiltration area from a potential hepatic neoplasm,
where unlike these,
focal steatosis most of the times occurs in characteristics areas: adjacent to the falciform ligament or the porta hepatis,
and gallbladder fossa.
Iron accumulation
On CT scans it is shown like liver density increasement,
although it is not specific for hemochromatosis,
also seen in entities like glycogen storage disease,
Wilson's disease or amiodarone administration among others.
However,
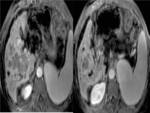
excessive accumulation of iron in the liver is better detected by MRI than CT,
because of its sensitivity.
Besides that,
it could also valorate abdominal solid complications such as cirrhosis or HCC.
Moreover,
using standard sequences (spin-echo),
it may be seen the typical low signal intensity on T2WI in the affected organs.
Vascular disease
In these entities,
CT scans demonstrate an enlarged caudate lobe because of its independent venous drainage,
it is not injured most of the times.
On the other hand,
the hepatic veins or inferior vena cava (IVC) are stenotic and cannot be seen.
The enhancement is heterogeneous with iv contrast media,
showing a centripetal behavior.
Gadolinium can clearly characterize vascular permeability,
especially aorta and its branches,
including hepatic artery veins,
portal vein,
superior mesenteric vein,
splenic vein,
and IVC.
Thus,
MRI is more sensitive than CT in detecting portal vein thrombosis,
being the best imaging method for studying Budd-Chiari syndrome and its follow-up looking for further complications.