Keywords:
Neuroradiology spine, Musculoskeletal spine, Conventional radiography, Absorptiometry / Bone densitometry, Diagnostic procedure, Observer performance, Comparative studies, Metabolic disorders, Demineralisation-Bone, Osteoporosis
Authors:
A. Bazzocchi1, F. Fuzzi1, P. Spinnato1, D. Diano1, G. Guglielmi2, C. Sassi1, G. Battista1, E. Salizzoni1; 1Bologna/IT, 2Foggia/IT
DOI:
10.1594/ecr2012/C-1943
Results
Seventy vertebrae (70/884,
7.9%) were excluded from the lesion-based analysis of results,
as not evaluable with one or both of the two techniques: 14/70 (20.0%) with radiography,
59/70 (84.3%) with DXA (upper thoracic spine).
Out of the 814 verterbrae considered in the analysis,
40 “true” fractures were detected (40/814,
4.9% vertebrae; 25/40,
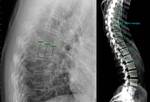
62.5% mild fractures) in 26 affected patients (38.2% of the 68 studied patients) (Fig. 2,
Fig. 3).
On a lesion-based analysis DXA sensitivity and specificity were 70.0% and 98.3% showing a good accuracy (AUC=0.842±0.044).
Performance of DXA on a patient-based evaluation achieved similar results: sensitivity 73.1%,
specificity 90.5%.
The experience of radiologists did not significantly influence DXA accuracy,
sensitivity and specificity on both lesion- and patient-based analysis (p=0.748 and p=0.994,
respectively).
Inter-observer agreements among the 3 observers was higher for XR (k=0.824 for XR,
0.720 for DXA,
p=0.011) (Fig. 4).
Intra-observer agreements were excellent (k=0.954 and 0.915,
for XR and DXA respectively,
p=0.322) (Fig. 5).
As previously said,
accuracy of DXA was not influenced by radiologist experience; moreover, reproducibility and repeatability of the two techniques were independent from sex,
age,
body mass index of patients,
arthrosis,
and vertebral level of lesions.
However DXA sensitivity was affected by mild VFs.