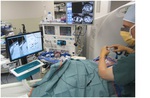
Percutaneous biopsies,
drainages and ablations have become,
one of the most commonly performed image-guided procedures in radiology practice.
General radiologist face a refinement in imaging guidance,
devices and techniques,
but also previously inaccessible and difficult to target lesions requires now a percutaneous diagnostic and management.
Traditional CT guided procedures require the radiologist judgment,
skills and experience to determine needle entry,
trying to avoid the placement of the devices through non-target organs.
In practice,
entry points permitting needle travel in the axial plane are preferred for simplicity.
However,
at times,
the axial plane may suffer from additional risks,
such as crossing multiple anatomic spaces (e.g.
pleural,
retroperitoneal or peritoneal); axial routes may come perilously close to vital structures.
Needle tracks not orthogonal to the z-axis can be tricky to achieve reliably and may require multiple needle re-adjustments that increases the radiation dose for the patients and the time of the procedures.
The outcomes of image-guided therapies,
such as biopsies and RFA,
are highly dependent on the size and location of the lesion,
the accuracy of needle placement and the experience of the physician who rely upon sophisticated manual skills to manipulate complex devices like multi-probe ablation systems towards sometimes nebulous targets.
Proper needle depth placement requires careful attention to needle length and penetration and is operator dependent.
Navigation technology can improve the results by allowing pre-acquired images to be used during the procedures,
sometimes on different contrast phase (arterial or portal vein) that shows better a lesion,
with real-time reference markers,
and visual tracking of the needle to guide the physician’s hand.
Some of the navigation system can also help for a pre-ablation planning,
what before was always the radiologist mental 3D visualization to plan needle insertions,
sizes and types,
and potential numbers of ablations.
NAV systems aid in entry point selection by projecting a virtual path on an image from a planning CT data set.
Potential entry points can be compared for suitability and risk.
Non-axial needle paths are easily planned,
yielding a safe solution from skin to target.
Need to transgress multiple anatomic spaces is reduced.