The radiological examinations,
clinical and histopathologic reports from fourteen patients (11 females,
3 males,
mean age 42) with histologically verified abdominal wall tumours were retrospectively reviewed.
The tumours were primarily assessed with sonography and,
in selected cases,
further CT or MRI examinations were performed.
The following sonographic features were analysed: size,
shape,
echotexture,
vascularity,
and effect on the surrounding tissue.
Within the 15 patients included in the study a large diversity of histopathological entities was found,
including desmoid (n=5),
endometriosis (n=3),
Schloffer tumour (n=2),
lipoma (n=1),
focal myositis (n=2),
and metastasis of cervical carcinoma (n=1).
Description of the encountered entities:
Lipoma: the clinical diagnosis of lipoma is based on patients' clinical history (indolent,
slowly growing tumour) and on the palpation of a soft,
well-defined and mobile mass.
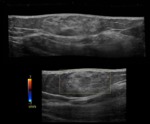
It sonographically appears as an ovoid,
well-circumscribed,
sometimes capsulated tumour which is iso-,
or slightly hypo-/hyperechoic (Figure 2A) compared to the adjacent adipose tissue.
It can develop in the subcutaneous fat tissue as well as intramuscularly.
It usually present typical "striped" pattern,
i.e.,
inner hyperechoic bands parallel to the skin [2].
On color Doppler mode it usually shows few Doppler signals (Figure 2B).
It usually has a characteristic sonographical appearance,
so that generally it does not require additional imaging procedures.
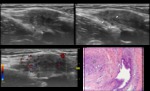
Desmoid: manifests as a slowly growing mass which can develop from the musculoaponevrotic structures of the abdominal wall and from their fascial coverings [3].
It can also develop within the subcutaneous adipose tissue.
It is a tendon-like lesion consisting of fibroblasts and a variable amount of collagen (Figure 3D).
Due to the high collagen content it is firm when pressing onto with the scan head.
Even if of benign character,
it is a locally aggressive fibrous tumour with a high tendency to reoccur if not resected completely.
The echotexture of this tumour depends on the amount of the fibroblastic proliferation,
collagen content and vascularity [3] and hence can be variable,
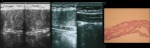
ranging from homogeneously hypoechoic (Figure 3A) to mixed hypo- and hyperechoic (Figure 4) [4].
When using a high frequency scan head (up to 17 MHz) the hyperechoic areas demonstrate a fibrillar pattern,
similar to the pattern seen in tendons (Figure 4) [4].
Intramuscular desmoids show spindle-shaped margins which extend between the muscle fibers at the tumour’s proximal and distal ends on the longitudinal scans performed along the long axis of the muscle fibers (Figure 3B arrowheads) [4].
Desmoids situated superficially within the subcutaneous adipose tissue have an irregular appearance in each orthogonal plane (Figure 4),
which can be due to the fact that superficial desmoid is surrounded by loose connective tissue [4].
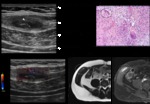
The diagnostic imaging algorithm of desmoid tumours includes also CT and MRI.
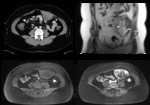
CT shows a soft-tissue mass of variable attenuation relative to muscles and also variable enhancement (Figure 5A) [3,
5].
Heterogeneous attenuation may be seen because of necrosis or degeneration [5].
On MRI desmoids may have heterogeneously signal and inhomogeneous enhancement (Figure 5B,
C and D) because of the variable distribution of spindle cells,
collagen and myxoid matrix [5].
On T2-weighted images the signal intensity is usually intermediate,
between skeletal muscles and subcutaneous fat (Figure 5B) [5].
Inside the tumour hypodense (on CT) and hypointense (on MRI T1-weighted and T2-weighted sequences) bands may be present (Figure 5A and 5B,
arrowheads) corresponding to collagen bundles [5].
Endometriosis: is defined as functioning endometrial tissue (endometrial glands and stroma,
Figure 7D) at ectopic sites.
In many cases abdominal wall endometriosis occurs after laparoscopic or laparotomic surgery involving the uterine cavity,
but it may also include lesions which are not a consequence of any previous surgery [6].
It can be situated both superficial within the subcutaneous tissue and deep involving the muscle layers.
Its locations include the umbilicus,
caesarean section scars and the inguinal canal [6,
7].
While the presence of abdominal wall endometriosis at the level of a previous operation scar can be explain by the concept of iatrogenic transport of endometrial cells to ectopic sites [8],
spontaneous abdominal wall endometriosis in a scarless abdomen should have a different pathogenesis.
Direct extension of endometrial tissue along the round ligament can be a possible pathogenesis of spontaneous inguinal endometriosis (Figure 6) [7,
9].
Indeed,
in one case of our series in a patient with no history of abdominal surgery we could provide evidence of the contact between the endometriosis mass situated in the right inguinal canal and the round ligament (Video).
The clinical symptoms of abdominal wall endometriosis include cyclic or continuous pain associated with a palpable mass,
and sometimes additional symptoms suggestive of ovarian or pelvic endometriosis,
such as dysmenorrhea,
dyspareunia or infertility [6].
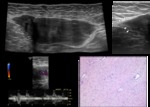
On sonography the lesions appear mostly solid (Figure 7) [6,
8],
but can also be cystic and show internal septa [7].
When solid,
they have a round/ovoid shape,
are usually inhomogeneous,
but can also present as homogeneously [6] hypoechoic masses.
These tumours display ill-defined margins and can contain small cystic changes (Figure 7B,
arrowheads).
On color Doppler they show scarce blood vessels (Figure 7C).
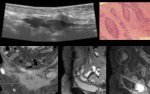
Suture granuloma (Schloffer tumour): it represents a benign tumour-like,
granulomatous inflammatory lesion that occurs after a surgical intervention in which nonabsorbable sutures were used [10,
11].
It usually develops slowly,
may remain asymptomatic for many years and can be accompanied by vague symptoms including moderate pain or discomfort.
Histologically it is characterized by a histiocytic reaction with foreign body giant cells around the suture (Figure 8C) [11].
Sonographically the suture granuloma presents as a well-defined hypoechoic lesion that may include an echo-free or echo-poor liquefied center representing a chronic abscess and hyperechoic double (rail-like) or single lines inside it representing suture material (Figure 8A,
arrowhead) [11].
On color Doppler scant vascularization is observed (Figure 8B).
Due to its high spatial resolution sonography usually enables the correct diagnosis based on the detection of the typical appearance of sutures within the hypoechoic granuloma.
Because of their small size,
sutures are not easily detectable on CT or MRI images (Figure 8D and E),
these modalities being able to only detect an unspecific fluid collection with enhancement due to inflammation.
Focal Myositis: is a rare,
benign inflammatory pseudotumour of skeletal muscles [12].
It presents with localized,
painful swelling within the soft tissue over a period of several weeks [12].
It is not associated with previous trauma or signs of systemic disease and resolves spontaneously within a few weeks (Figure 9B).
Diagnosis is establish by biopsy,
which shows severe myopathy with inflammation demonstrated by lymphocytic infiltration of the perimysial and endomysial spaces,
scattered muscle fiber necrosis and regeneration,
as well as interstitial fibrosis (Figure 9C) [12].
Focal myositis can be recurrent affecting multiple muscle groups [13] and some patients with focal myositis can subsequently develop polymyositis [14].
The sonographic appearance can show an enlarged muscle with homogeneously hyperechoic signal (Figure 9A).
The lesion can also present as a polylobulated,
inhomogeneous and hypoechoic tumour within the muscle [15].
Metastases: these tumours can occur in the abdominal wall within surgical scar following open surgery [16],
or interventional procedures such as percutaneous needle biopsy or percutaneous ablation therapy for focal liver malignancies [17].
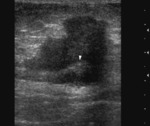
These lesions show round or oval form,
and can be single or multiple.
The nodules have variable size,
ill-defined margins with infiltration of the adjacent tissue as a sign of aggressive malignant character.
They usually display hypoechoic solid echotexture (Figure 10).
They may become very large without any clinical manifestation.
The most common metastasis is from melanoma [1].
When a metastasis occurs in the umbilicus,
it is called a Sister Mary Joseph’s nodule [18].
Primary malignant tumours of the abdominal wall such as sarcomas [19,
20] are rare and were not included in our series.

![Fig. 6: Anatomic scheme of the possible extension of endometrial tissue along the round ligament. The canal of Nuck, which constitutes a small evagination of the parietal peritoneum, surrounds the round ligament through the inguinal canal. In the adult the canal of Nuck is obliterated. Occasionally this canal may remain patent, creating a communication between the peritoneal cavity and the female inguinal canal, providing the most likely pathway for endometrial tissue to seed in the superficial inguinal soft tissue [9].](https://epos.myesr.org/posterimage/esr/ecr2012/112645/media/416638?maxheight=150&maxwidth=150)