Clinical symptoms: expressed shortness of breath (3-4 degree on a scale MRCDS) and chest pain (74,3%).
Blood gas analyses:рН – 7,36±0,9; Ро2 – 46,2±12,1; Рсо2 – 50,1±10,3.
The values of the gas composition of the blood in patients with PE authentically did not differ from those of the other causes of an exacerbation of COPD.
In patients with PE were observed lower rates of vital lung capacity (VLC) (42,4 ±3%),
while the FEV1 authentically did not differ.
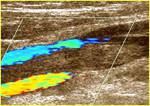
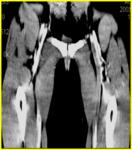
Thrombosis of deep veins of the legs (DVT)(fig.1,
2) has been revealed in for 91.3% of patients.
Localization of DVT: ileo-caval segment - 47.6%, femoro-popliteal segment - 30,1%,
several venous segments -15.2%, the veins of legs - 7,1% .
In 54.7% of the patients DVT proceeded asymptomatic.
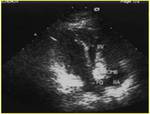
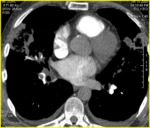
By echocardiography of blood clots in the right atrium (fig.3) was detected in 1 patient with PE and COPD.
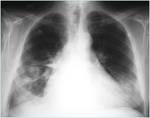
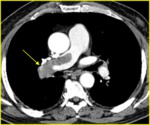
Х-ray of the chest: the findings of PE was suspected in only 36.9% of patients.
The signs of PE (fig.4) included: subpleural infiltrates,
pleural effusion,
elevated hemidiaphragm,
band atelectasis,
cardiomegaly.
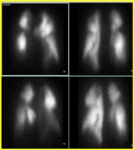
Have we examined patients discrepancy data MSCT with perfusion scintigraphy (99мТс) was 3 cases (6,5%): false positive - 1, false-negative - 2.
Pulmonary perfusion may be impaired as a result of a reactive vasoconstriction due to obstruction of the bronchi.
Specific to PE perfusion defects - hypo- and aperfusion areas (fig.5) can be attributed to the areas of fibrosis,
the presence of effusion in the pleural cavity and emphysema.
Therefore,
the data perfusion scintigraphy of the lungs in COPD more frequently than in other pathological conditions diagnostically unreliable (>30%).
Excess of a level of D-dimer was celebrated in almost all patients with DVT (from 0,5 mcg/ml and 3.5 mcg/ml).
In 2 patients the indicators of D-dimer were below or at the level of 0,5 mcg/ml when there is direct evidence of Pulmonary Embolism when MSCT.
One patient indicators of D-dimer were above 0,5 mcg/ml at negative data MSCT,
even at 3 patients indicators of D-dimer were normal in the absence of signs PE when MSCT.
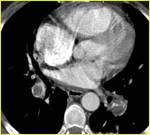
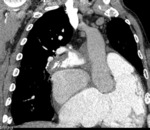
MSCT showed vascular and parenchymal signs of PE.
Vascular signs included intraluminal thromboembolic masses at different levels of the pulmonary artery (fig.6,
7,
8),
often bilateral (56,7%).
Parenchymal signs of PE were lung infarction (41,3%) and mosaic perfusion (15,2%).
Chronic pulmonary embolism was found at 8.6% of the patients.
CT signs of chronic pulmonary embolism (fig.9) recorded in the present study include: organized thrombi,
calcified thrombi,
reanalyzed thrombi,
dilatation of pulmonary artery,
mosaic perfusion.
To assess the status of venous bed successfully used CT-flebography: in the venous vessels clearly render blood clots different localization and length (fig.10).