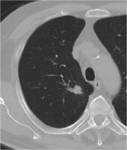
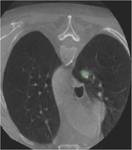
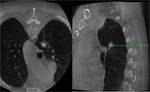
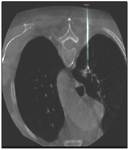
Patients characteristics
This was a retrospective review of the biopsies performed in our institution between February 2010 to July 2011.
This study was approved by internal board review of our Hospital.
From February 2010 to July 2011,
70 percutaneous transthoracic needle biopsies of pulmonary nodules were performed in 70 patients (40 males,
30 females,
mean age 65.6 years,
range 26-82 years).
All patients had a diagnostic conventional chest CT prior to biopsy.
The mean size of the lesion was on average 5,5 cm (range 1 cm -11 cm).
The lesions were divided into two groups according to their transverse diameter: lesions equal or less to 3 cm (34 patients) and lesions larger than 3 cm (36 patients).
The lesion was on average 2.5 cm from the pleura (range 0-5 cm) in the first group of patients (lesion equal or less to 3 cm) and it was on average 1,2 cm from the pleura (range 0 – 4 cm) in the second group.
52 of 70 patients (74,2%) were suffering from chronic obstructive lung disease,
55/70 patients (78,5%) were smokers at the moment of biopsy.
Imaging system and needle path overlay
All examinations were performed in the angiography suite (Philips Allura Xper FD20 system,
Philips Best NL) with CBCT navigation (Xperguide,
Philips Healtcare,
Best,
NL).
The C-arm rotates around the patient acquiring CT-like imaging on which the operator plans a virtual needle path choosing the skin entrance point and a target.
In our study we used a 4 s acquisition time for a rotation of 240°,
which generates 310 images with a 512 x 512 image matrix and a total reconstruction time of 25s.
Depending on the image matrix and field of view,
the highest spatial resolution is 0.4 mm while contrast resolution for the soft tissue is equivalent to 5 HU at a slice thickness of 10 mm.
The reconstructed isotropic soft tissue volume is displayed automatically on the monitor in the examination room; manipulation and viewing of the image volume can be done directly at the tableside as well as in the control room.
Lung biopsies technique
The biopsies were performed by two interventional radiologist (GP.C.
and F.F.
with 15 and 7 years of experience respectively).
Written informed consent was obtained from each patient before the procedure.
During the procedure,
heart rate,
ECG,
oxygen saturation and respiratory rate were continuously monitored,
while blood pressure was obtained every 4 minutes.
The patients were placed prone or supine depending on the lesion location.
Once CBCT scan was acquired,
the access area was prepped with sterile technique and local anesthesia was given (10 cc of mepivacaine 2%,
Angelini,
Roma,
Italy).
The needle was then advanced according to the virtual path determined by the operator with realtime fluoroscopy.
Once the target reached,
a confirmation CBCT was obtained.
In all cases,
fine needle aspiration was obtained with 20 Gauge bioptic needle (Biopsy Bell,
Medical Device,
Modena,
Italy).
Immediately after FNAB an additional CBCT was performed to evaluate any complications,
moreover a follow-up postero-anterior expiratory chest radiograph was also obtained two hours after biopsy.
The complications were classified into minor and major complications according to SIR classification [6].
Calculation of Radiation Dose
Doses in Cone-Beam CT were calculated with PCXMC dose Calculations (version 2.0) according to ICRP 103 and considering a hermaphrodite phantom (Rando phantom,
model RAN-10,
Churcin
Associates,
Smithtown,
NY ) [7].
For fluoroscopy,
projection parameters such as source-to-skin distances,
field dimensions and positions chosen during the actual procedures were used to calculate dose.
An AP projection was
chosen for supine patients,
PA projection for prone patients and LR or RL projections depending on lesion site and patient position (x-ray tube as close as possible to pulmonary lesion).
The needle is advanced based on two views,
one view is parallel to the needle and the other view is perpendicular to the needle.
Adjustments are made in the orthogonal view.
Doses were calculated considering the actual Dose Area Product (DAP) imparted in each projection.
A single arc was divided into 43 steps,
5° each,
and calculation was done taking into account patient position (supine or prone).
Doses were calculated dividing total arc DAP in 43 equal parts and associating one part to each step.
This schematization seems adequate because C-arm speed rotation is nearly constant.
Statistical analysis
Technical success rate,
sensitivity,
specificity,
positive predictive value,
negative predictive value and accuracy were calculated.
Technical success was defined as correct placement of the needle into the lesion.
Accuracy was determined by comparing FNAB with final histopathological diagnose in cases of surgical resection or clinical and radiological outcomes if surgery was not performed.