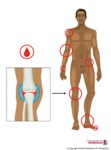
Haemophilia is a congenital coagulopathy,
recessive inheritance X-linked (although up to a third of patients have sporadic haemophilia by a spontaneous mutation),
deficiency in clotting factors VIII,
IX and XI (haemophilia A,
B and C, respectively),
which manifests clinically in males (Fig. 1)
Are calculated up to 400,000 people affected by haemophilia in the world,
with an incidence in Spain than 1 in 15,000 births.
Haemophilia A occurs in about 1 in 10,000 males (85% of haemophilia) and B in 1 in 100,000,
with no racial predilection.
Haemophilia C has certain differences from the A and B: its incidence is 1 per million births,
and tendency to haemorrhage is lower (not usually seen hemarthrosis or muscle bleeds).
The clinical severity correlates with the coagulation factor levels in the blood (concentration factor)(Fig. 2 ):
MILD: 5-10%
MODERATE :1-5%: delayed bleeding or prolonged bleeding
SERIOUS: <1%: clinical presentation in the first year of life with severe bruising.
Its most common clinical haemarthrosis repeat (to 70-80%).
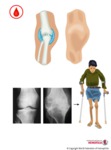
The joints most often affected (Fig. 3 ) are knees (45%),
elbows (30%) and ankles (15%) and ultrasound and MRI have been proven as the best evidence for diagnosis.
In 1868 and Volkman said that bleeding can occur spontaneously or after trauma and in 1892 linked the Atritis König of haemophilia with previous bleeding and recurrent joint.
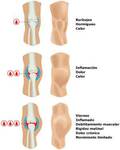
He noted the three clinical stages (Fig. 4 ):
Acute rebleeding.
The clinic is described as the aura with mild stiffness limited to the synovial bleeding and tingling.
When the entire joint is filled with blood are heat,
pain,
swelling and tension.
Later we find limited movement and muscle spasms.
Subacute inflammatory response and with panartritis: recurrent bleeding hurts less and the degree of impact of mobility is lower.
Chronic: fibrosis and contractures.
After diffuse haematoma in the synovium,
there is blood resorption and inflammatory response leading to the formation of new blood vessels that carries more bleeding,
then produce recurrent bleeding and synovium creates enzymes that cause further inflammation.
This affects the synovial destruction and scar formation and fibrosis.
The cartilage breaks down and becomes rough,
destroying the joint with onset of local pain,
deformities and fractures (Fig. 5 ).
MRI is a highly accurate diagnostic method that allows us to assess the involvement both intra and extra-articular and severity depending on the scale that is based supports and values all scale criteria of Denver and the European Score.
We study therefore potentially reversible lesions: effusion / haemarthrosis,
synovial hypertrophy and hemosiderin,
and irreversible: changes in the subchondral bone (bone erosions and subchondral cysts) or joint margins and loss of articular cartilage.
With MRI can pinpoint the exact location of the spill,
its size,
stage blood,
if any clots and the possibility of rebleeding.
MRI can also assess the extra-articular involvement and other musculoskeletal injuries not haemophiliacs.
Synovial hypertrophy is the first sign of joint involvement after bleeding: in the first stage (exudative phase) is smooth and regular,
while proliferative phase becomes rough and irregular.
Early detection and early treatment of synovial involvement are the only proven strategies to prevent the progression of joint disease and the development of irreversible changes.
Detection of hemosiderin differentiating articular haemophilic bleeding of other pathologies.
Intramuscular and subcutaneous haematomas account for 15% of bleeding complications,
and are produced by compression of vessels or peripheral nerves.
When located in forearm flexor muscles,
clinically claw hand appears and if in the twin: equinus.
If encapsulates and progresses rapidly pseudotumor is formed,
whose treatment is conservative.
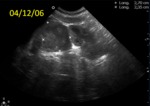
The most serious medical conditions are life threatening,
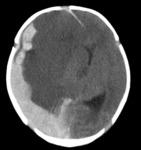
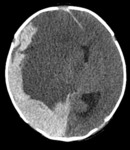
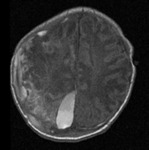
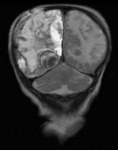
such as intraperitoneal bleeding in oropharyngeal cavity and cerebral haemorrhage (frequency <5%),
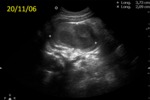
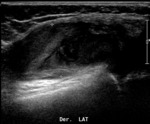
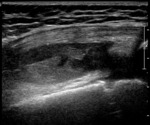
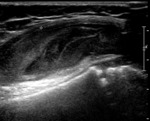
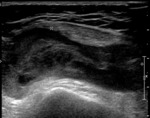
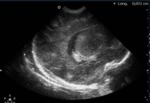
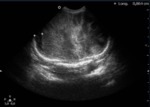
with ultrasound (Fig. 6 Fig. 7 Fig. 8 Fig. 9 Fig. 10 Fig. 11) being the initial imaging method for studying joint,
abdominal and brain,
in patients with open fontanelle.
CT ( Fig. 16 Fig. 17 Fig. 20 Fig. 21) and MRI (Fig. 27 Fig. 28) complement the study with greater accuracy.
The most appropriate diagnosis is made with the clinical history and laboratory tests with a time of normal or increased bleeding,
increased activated partial thromboplastin time,
platelet count normal,
and a quantitative study of factor VIII and IX.
The treatment is based on prevention of bleeding and replacement therapy lacking factor (treatment with FVIII concentrates or prophylactically IX has demonstrated a significant benefit in terms of reduced incidence and severity of haemarthrosis (less sequelae) ).
In the 80s began to use the first coagulation factors from fresh human plasma.
Subsequently,
due to infection,
the first decade were introduced viral inactivation methods lyophilized concentrates,
transforming them into products much safer.
Presently,
the recombinant factor VIII,
the most crowded,
is produced from cells grown in the laboratory (the World Federation of Haemophilia recommended recombinant products,
as it ensures greater safety with the same efficacy as plasma products).
Treatment with FVIII concentrates or prophylactically IX has demonstrated a significant benefit in terms of reduced incidence and severity of hemarthrosis (less sequelae).
Gene therapy using recombinant products (introduction of genes into cells of the patient able to combine with existing genetic material,
providing the information needed to make the protein deficit causes the disease),
provides good prospects for the future.
The interventional treatment is performed by chemical synoviorthesis,
radiosynoviorthesis (radioisotope synovectomy) and surgical synovectomy.
Prevention attempts to avoid the use of AAS,
genetic counseling to detect female carriers and the severity of symptoms,
prevention of bleeding (avoid exposure to unnecessary trauma and physical therapy) and vaccination for potential infections (such as hepatitis transfusions B,
...).