MR Protocol usually includes unenhanced imaging T1 gradient-recalled echo (GRE) sequences with out-of-phase and in-phase image acquisitions,
T1 with fat-saturation,
T2 with fat-saturation,
and sometimes T2*.
In some centers,
diffusion-weighted sequences are also performed.
After administration of the gadolinium chelate T1-weighted images are acquired in arterial,
portal and late phases.
Some centers also recommend mixed extracellular and hepatocellular agents and Superparamagnetic iron oxide based MRI contrast agents but until now dynamic MRI after bolus injection of gadolinium is still the workhorse of liver imaging.
MDCT protocol,
four phases: nonenhanced,
arterial-phase,
portal-venous-phase and late phase.
1.
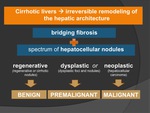
Regenerative Nodules (RNs)
ž Formed in response to necrosis,
altered circulation,
or other stimuli
ž Are the most common cirrhosis-associated nodules
ž Classified according to size : micronodules (<3mm),
macronodules (≥3 mm)
ž Giant nodules (>5 cm) are rare
ž Round and sharply circumscribed
ž Numerous and diffusely distributed
MR:
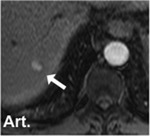
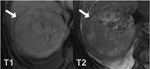
Low signal intensity on T2 and T2* (Fig.3)
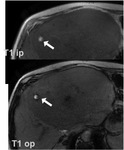
Signal intensity on T1 is variable may be hyperintense (Fig.4)
Lipid-containing nodules display signal loss on out-of-phase GRE images
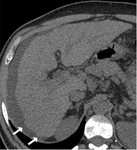
CT:
Difficult to visualize - Isodense
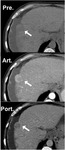
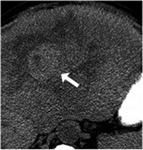
May be depicted in nodular hepatic surface (Fig.5)
Siderotic Regenerative Nodules
Some nodules have high iron content
MR:
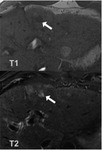
Low signal intensity on T1 and T2* (Fig.6)
CT:
Predominantly high-attenuation nodules on unenhanced CT
Enhancement
Predominantly portally perfused
Enhance to the same degree as the adjacent liver or slightly less enhancement
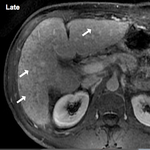
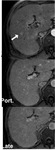
RNs with thick septa are visualized as round nodules surrounded by enhancing fibrous septa on delayed-phase MRI (Fig.7)
2. Dysplastic Nodules (DNs)
ž composed of hepatocytes that display histologic characteristics of abnormal growth caused by a presumed or proved genetic alteration
ž Without histologic criteria for malignancy or invasion
ž dysplastic foci (<1 mm in diameter) or dysplastic nodules (≥1 mm in diameter).
ž classified as low or high grade,
according to the degree of dysplasia
ž the clinical relevance is still unclear
MR:
LOW GRADE : similar to regenerative nodules
HIGH GRADE: Generally T1 hyperintense; Iso/hypointense on T2 (Fig.8)
CT:
LOW/HIGH GRADE: Difficult to visualize - Isodense
Enhancement
LOW GRADE : predominantly portally perfused
similar to the surrounding parenchyma (Fig.9)
HIGH GRADE: With progressive dedifferentiation there is a shift to
predominantly arterial perfusion
Hypervascular in the arterial phase
No washout! (Fig.10)
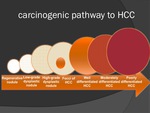
3. Hepatocellular Carcinomas (HCCs)
ž Malignant neoplasms composed of dedifferentiated hepatocytes.
ž Small (<2 cm in diameter) or large (≥2 cm in diameter)
ž Classically three major types:
- nodular: multiple,
fairly discrete nodules throughout the liver
- massive: a single large mass with or without small satellite nodules
- diffuse: when there are multiple,
minute indistinct nodules throughout the liver
ž The signal intensity characteristics of hepatocellular carcinomas in unhenhanced MR depends on their size,
grade and biologic features.
3.1 Nodule-in-nodule
ž Represents focci of HCC within a larger dysplastic or regenerative nodule
CT:
Hard to depict (an isoattenuating nodule)
MR:
Hyperintense focus within a hypointense nodule on T2 (Fig.11)
Enhancement:
The nodule of high signal intensity may show enhancement during the arterial phase and represents the focus of HCC; The lack of enhancement in the surronding area is suggestive of necrosis (Fig.12)
3.2 Small HCCs
ž Tend to be homogeneous,
round or oval,
and well defined.
MR:
Almost always hyperintense on T2
Variable signal intensity on T1 (isointense or even hypointense)
Some hyperintense on the T1 (fat,
glycoproteins or haemorrhage)
CT:
Iso or hypodense nodules (nonspecific)
80%–90% are hypervascular
Enhancement:
Intensely enhanced during the arterial phase (Fig.13)
Washout in portal/delayed imaging phases,
and typically have signal intensity lower than that of the surrounding liver; (Fig.14)
10-20% are hypovascular (very early carcinogenesis)
3.2.
Large HCCs
The increasingly dedifferentiated malignant nodules appear heterogeneous with markedly enhanced on early arterial phase images,
more pronounced washout on venous phase images and equilibrium phase images.
(Fig.15)
3.2.1 Large HCCs – structural variations
A. Large hepatocellular carcinomas with Cytoplasmic fat
MR:
Signal intensity decrease on out-of-phase images in comparison with in-phase images (Chemical shift artifact) (Fig.16)
CT:
decreased attenuation on unenhanced CT but with this technique the demonstration of microscopic fat is difficult (combination with higher-attenuation water and protein increases the mean CT number).
B. Large hepatocellular carcinomas with hemorrhage
MR:
The hemorrhagic foci have marked high signal intensity on T1 and low signal intensity on T2- and T2* (Fig.17)
CT:
The hemorrhagic foci are hyperdense in unenhanced CT (fig.18)
C. Large hepatocellular carcinomas with necrosis
MR:
Intralesional necrosis typically manifests as one or more areas of low signal intensity on T1 and high signal intensity on T2 (fig.19)
CT:
Hypodense areas
Enhancement:
lack of enhancement
D.
Large hepatocellular carcinomas - Mosaic pattern
MR:
Multiple compartments of variable signal intensity at unenhanced T1,
T2 and T2* distributed within the mass in a seemingly random manner (fig.20)
CT:
Heterogeneous mass
Enhancement:
enhance to non-uniform variable degrees (fig.21)
E. Large hepatocellular carcinomas - tumor capsule
fibrous tissue and compressed vessels
MR:
thin circumferential rim with low signal intensity on T1 and T2 (fig.22)
If thicker than 4 mm may have an outer layer with high signal intensity on T2- weighted images
CT:
Hypointense
Enhancement:
enhances progressively and retain contrast on delayed phase images (fig.23)
F. Large hepatocellular carcinomas - satellite lesions
frequently seen in large nodular hepatocellular carcinomas.
MR/CT:
The satellite lesions often appear as multiple subcentimeter nodules outside the tumor margins (fig.24)
G. Large hepatocellular carcinomas - vascular invasion
Differentiation from a bland thrombus is critical.
MR/CT:
The tumor thrombus rapidly enhances during the arterial phase,
and a filling defect is seen on images acquired during later phases (fig.25)
H. Large hepatocellular carcinomas - invasion
Rarely advanced hepatocellular carcinomas may penetrate the liver capsule and invade adjacent structures such as the diaphragm and abdominal wall (fig.
26)