The incidence of hepatocellular carcinoma (HCC) is increasing worldwide.
Currently it is the third leading cause of death from cancer and the first leading cause of death in patients with liver cirrhosis.
[1]
90% of HCC in the western world arises in a cirrhotic background and one-third of cirrhotic patients will develop HCC during their lifetime.
[2]
To reduce the disease-related mortality an early diagnosis allowing the application of curative therapies is essential.
Accordingly to the 2012 consensus guidelines from the European Association for the Study of the Liver (EASL) and the European Organization for Research and Treatment of Cancer (EORTC),
patients at high risk for developing HCC should enter a surveillance program using abdominal ultrasound every 6 months.
If a nodule <1cm is found,
ultrasound should be repeated 4 months later and further investigation (with MDCT or MR) is then mandatory if there is evidence of growing or change in imaging pattern.
[2]
Since 2005,
it was established that the diagnosis of HCC could be settled,
by non-invasive criteria in cirrhotic patients based on the identification of the typical imaging hallmark of HCC (hypervascularity 
in the arterial phase with washout in the portal/late phases).
[3] A few years ago these criteria were only applied to lesions > 2cm in one imaging technique,
while lesions between 1-2cm required two coincidental techniques.
[3] Recent updated American Association for the Study of Liver Diseases (AASLD) guidelines have proposed that one imaging technique (MDCT or MRI) showing the HCC hallmark suffices for diagnosing 1-2cm tumors.
[4] EASL-EORTC updated recommendations supports this finding but states that in suboptimal settings (for example,
technological limitations) two coincidental techniques are still recommended.
[2] As so,
MDCT and MRI have been stated as accurate,
noninvasive imaging techniques in the detection of HCC in a cirrhotic liver,
while biopsy remains the gold-standard in uncertain cases.
[2]
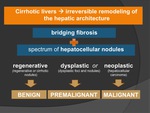
It is well-know that there is a wide spectrum of nodules affecting cirrhotic patients besides HCC.
(Fig.1) The most frequent nodules in cirrhosis are benign regenerative nodules,
although,
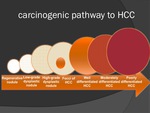
there is a well-described carcinogenic pathway to dysplasia and later HCC.
(Fig.2) [5,6,7] So,
proper definition of nodules as pre-neoplastic or neoplastic is mandatory as it has critical therapeutic implications.
[2]
Awareness of the spectrum of cirrhotic associated lesions allows distinction of the lesions that have a higher degree of suspicion,
preventing unnecessary or inadequate procedures.
[8.9]
Remarkably arterial hypervascularity has a high specificity for HCC,
but the sensitivity is less satisfactory as in very early hepatocarcinogenesis there is a reduction of intranodal arterial blood supply caused by degeneration of normal hepatic arterial vasculature and so there is still a portal perfusion predominance.
In the next carcinogenesis phase there is a rapid replacement of normal vasculature by neoplastic angiogenesis which leads to an increased abnormal arterial blood supply and finally,
in advanced stages,
to complete obliteration of intranodular portal veins.
[10,
7]
So one must keep in mind that about 10%–20% of HCC will appear hypovascular,
typically the small,
well-differentiated tumors (i.e.,
those characterized by hepatic artery degeneration and preserved portal veins).
[2]