Patients - Between June 2012 and January 2013 a total of 154 patients(89 men and 65 women,
mean age at presentation was 44),
with story of low back pain related to lumbar disc herniation for at least 4 weeks with no or poor clinical improvement after conservative therapy,
were selected for the protocol of prospective double-blind trial.
Based on an assessment of the visual analog scale[5] (VAS) ranging from 0 to 10,
only patients with initial pain value above the cut-off of 3 were included in our study and were randomly assigned to two groups.
Seventy-seven patients (Control Group consisting of 47 men and 30 women; mean age 43.8±11.2) were undergone conservative treatment with intraforaminal injection (L4-L5 ,
4 patients; L5-S1,
73 patients) of 4mg/2ml di bethametasone,
and 2-4 ml of 2% ropivacaine.
Seventy-seven patients (Study Group consisting of 42 men and 35 women; mean age 44.4±9.5) were undergone oxygen-ozone(O2-O3) discolysis and treated (L4-L5,
5 patients; L5-S1,
72 patients) with percutaneous intradiscal oxygen-ozone(O2-O3) injection performed by two neuroradiologists. Thereafter,
patients were undergone follow-up period in which control MRI examinations were performed at the second,
fourth, and sixth month after oxygen-ozone(O2-O3) discolysis.
The outcome was measured the day of the procedure and subsequent follow up,
using a visual analog scale (VAS)[5],
ranging from 0 to 10.
The response to treatment was classified as successful if the pain value was no greater than 2 at follow-up,
and unsuccessful otherwise.
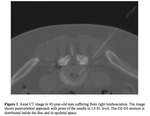
Injection technique - All procedures were performed under CT guidance and with the patient in the prone position.
Before every procedure,
the patients received premedication with intravenously administered of antibiotic and gastric protector.
The O2-O3 gas mixture was achieved by using an ozone generator. After local anesthesia,
the spinal needle (9 or 13 cm 22 gauge) was advanced to the intraforaminal space through paravertebral approach(Fig.1).
Overall,
both in the Control Group than in the Study Group,
the average injected volume of a steroid and anesthetic was 5 ml at intraforaminal space while only in the Study Group was injected in adjunct 10 mL(28µg/ml concentration)of O2-O3,
in particular 4 ml at the intraforaminal level and 6 ml inside the disc.
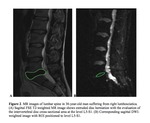
MR Protocol - Each participant underwent MRI exams of the lumbar spine performed at 1.5T MRI scanner,
before and after steroid or oxygen-ozone(O2-O3) discolysis in the subsequent follow-up at the second,
fourth, and sixth month.
Sagittal FSE-T2 and T2 Fat-weighted images were acquired with the following parameters: 4000/108/4 (TR/TE/NEX),
while for sagittal SE-T1 weighted images 500/20/2(TR/TE/NEX). Both T1 and T2 weighted images were acquired using the same values of matrix (256 x 192),
slice thickness 5 mm,
spacing 1 mm and a field of view (FOV) of 26 cm.
Axial T2 weighted images were acquired parallel to the disc space with a field of view(FOV) of 17 cm. Diffusion weighted images (DWI) were obtained in sagittal and axial plane by using isotropic multishot spin-echo-planar MR imaging with followed parameters: 1215/80/6(TR/TE/NEX),
matrix,
128 x 128,
with the same values of slice thickness,
spacing and field of view (FOV) of T2 and T1 weighted images obtained in sagittal and axial plane.
The DWI images were acquired without diffusion weighting (b = 0 sec/mm2) and with diffusion weighting (b=400 sec/mm2).
Qualitative and Quantitative - image analysis with Morphologic Matching- According to the recommendations of the combined task forces of the North American Spine Society,
the American Society of Spine Radiology and the ASNR[6],
on FSE-T2,
FSE-T2 fat and SE-T1-weighted images, the type of herniated disc was classified as protrusion,
extrusion and sequestration while the location was classified as central,
left/right central,
subarticular or foraminal/extraforaminal.
Disc degeneration and hydration was assessed on the MR T2-weighted sagittal images by using a five-point scale according to the method of Pfirrmann et al[7].
The grade of nerve root compression was classified as contact,
deviation,
and compression.
Intervertebral disc Volumetric Analysis(IDVA) was obtained on FSE-T2-weighted images using Osirix® 4.1.
Entire disc and herniated parts were included in the ROI on all slice(Fig.2A).
The effect of ozone on disc water diffusivity was assessed with the DWI images and corresponding ADC maps.
The ADC values were selected through a small,
round regions of interest (ROIs) that measured 40–50 mm2 within the central portion of the disc on the DWI images(Fig.2B).
Before treatment,
a neuroradiologist reviewer selected for patient from the study group,
one matching control subject to exclude potential confounding factors,
according to the following criteria: same sex and age (differing by no more than ± 5 years),
same intervertebral disc level affected,
similar body mass index (BMI) (differing by no more than ± 5 kg/m2),
same extent of disc herniation(ie,
protrusion,
extrusion,
or sequestrion),
same grade of disc degeneration,
same location of the lumbar disc herniation,
same grade of nerve root compression,
similar herniation volume (IDVA) and ADC value(differing by no more than ± 5%).
Statistical analysis - χ2 test was used for assessing the results before treatment and the differences between the responder and non-responder groups.
Student’s T test was used for determining the differences between the study and control groups in terms of reduction of average ADC and whole discs with herniation volume values after treatment.
A logistic regression analysis was used to check for a relationship between age,
BMI and sex before and after O2-O3 injection.
ROC curves analysis was performed for evaluating accuracy of DWI and related ADC values(DWI-ADC) versus intervertebral disc Volumetric Analysis(IDVA) for predicting shrinkage of lumbar disc herniation treated with oxygen-ozone(O2-O3) discolysis.