Vacuum biopsy developments in Switzerland between 2009 and 2011
Between the years 2009 and 2011,
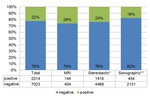
a total of 9113 vacuum-assisted breast biopsies with specification of the biopsy method were performed in Switzerland and entered in the database. Of these,
557 (6%) were performed on an MRI-guided basis,
5391 (59%) on a stereotactic basis (at a dedicated stereotaxis table),
569 (6%) on a stereotactic “upright” device and 2596 (28%) on a sonographically guided basis.
MRI-guided biopsies displayed a growth rate of 97% over the entire period with a growth of 49% between 2009 and 2010 and 32% between 2010 and 2011.
The development of all vacuum biopsies,
including those performed with the use of a stereotaxis table,
“upright” device and ultrasound are displayed in Figure 3.
Family and carcinoma history
A positive family history was deemed present when the patient’s mother,
sister or daughter (1st degree of kinship) exhibited a positive history of breast carcinoma.
The lifetime risk was not taken into consideration.
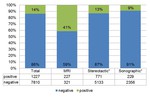
For MRI-guided VAB the family history was positive in 144/548 (26%).
The comparison to the stereotactic and sonographic VAB is shown in Figure 4.
A history of carcinoma was given in 227/548 (41%) of MRI-guided biopsies.
The comparison to stereotactic and sonographic VAB is shown in Figure 5.
Complications
Complications were divided into medical (haemorrhages without or with open revision and infection) and non-medical (technical complications,
missed lesions,
lesion inaccessibility) complications.
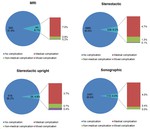
Non specific complications were indicated in 52/9037 cases and terminated intervention was indicated in 19/9037 cases without stating medical or technical grounds.
These 71/9037 cases were therefore not included in the evaluation of the complication rate.
The various vacuum biopsy methods were distributed among these 71 cases as follows: 4/548 wereMRI-guided,
32/5340 were performed with a stereotaxis table,
20/564 with the use of a stereotactic “upright” device and 15/2585 were sonographically guided.
The distribution of the complication rate and the comparison between MRI an the other VAB modalities is shown in figure 6.
We highlight,
that there was not one single case with the need for open revision by MRI-guided VAB
The histology of the vacuum assisted biopsy
The histological result of the vacuum assisted biopsy was specified as “other” in 175/9037 (2%) (21 MRI-guided,
82 stereotactically and 72 sonographically guided),
so that a distinction between malignant,
“high risk” or benign histology was impossible. These data were therefore not included in the analysis of the malignancy rate.
Thus,
vacuum biopsy histologies were available for 527/548 of the MRI-guided cases,
for 5822/5904 of the stereotactic and for 2513/2585 of the sonographic cases.
For the entire study population,
vacuum assisted biopsy revealed malignant lesions in 1853/8862 (21%) cases,
benign lesions in 5524/8862 (62%) cases and high-risk lesions 1485/8862 (17%).
For the entire study population,
MRI-guided vacuum biopsy revealed malignancies in 137/527 (26%) cases,
benign lesions in 283/527 (54%) cases and high-risk lesions in 107/527 (20%) cases.
Stereotactic VAB revealed a malignancy rate of 24% (1408/5822).
Stereotactic VAB revealed benign lesions in 3407/5822 (59%) cases and high-risk lesions in 1007/5822 (17%) cases.
Sonographic VAB verified malignant lesions in 308/2513 (12%) cases,
benign lesions in 1834/2513 (73%) cases and high-risk lesions in 371/2513 (15%) cases.
Histology of a subsequent surgical excision
Of the 8862 findings clarified via vacuum assisted biopsy with known histological results,
a total of 2434 (27%) lesions were further clarified via subsequent surgery,
whereby a histological result of the surgery was likewise available.
No histological result for the surgery was available in 131 cases,
so that these were not included in the analysis. Ninety percent (1660/1853) of the malignant lesions,
5% (255/5524) of the benign lesions and 35% (519/1485) of the high-risk or B3 lesions were surgically excised.
The operationquote dependent on the histological result of the VAB by the different VAB-procedures and also the upgrade rate from a benign or high risk VAB-result to a malignoma by surgical excision is show in Figure 7.