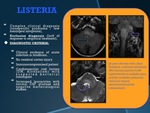
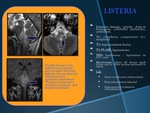
LISTERIA
•Complex clinical diagnosis (nonspecific prodrome / few meningeal symptoms),
•Exclusion diagnosis (lack of response to empirical treatment).
DIAGNOSTIC CRITERIA:
•Clinical evidence of acute infection in hindbrain.
•No cerebral cortex injury.
•Immunocompromised patient
•Cardiovascular risk factors (DM,
Alcoholism) with suspected bacterial meningism
•Increased leucocytes with normal CSF glucose and negative bacteriological studies.
•Extensive damage / patchy: fuzzy in brainstem,
cerebellar peduncles,
cerebellum.
•No exophytic component (vs.
neoplasm).
•T1: hypo-isointense lesion.
•T2/FLAIR: hyperintense.
•DWI: hyperintense / hypointense on ADC map.
•Spectroscopy: allows dd abscess (peak lactate and aa + little increase perfusion) vs tumor
•Gd:
•linear cranial nerve enhancement
•Ring enhancement (abscess)
•heterogeneous if extensive inflammation.
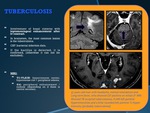
TUBERCULOSIS
•Involvement of basal cisterns with leptomeningeal enhancement after iv contrast.
•In brainstem,
the most common lesion is the tuberculoma.•CSF: bacterial infection data.
•If the bacillus is detected,
it is confirmed,
(otherwise it can not be excluded).
•MRI:
•T2/FLAIR: hyperintense center,
hypointense rim + peripheral edema.
•Gd: peripheral enhancement / nodular (depending on if there is central necrosis).
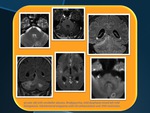
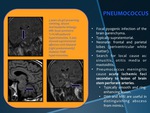
PNEUMOCOCCUS
•Focal pyogenic infection of the brain parenchyma.
•Typically supratentorial.
•Neonate: frontal and parietal lobes (periventricular white matter).
•Search for local cause as: sinusitis,
otitis media or mastoiditis.
•Pneumococcus meningitis cause acute ischemic foci secondary to lesion of brain stem perforant arteries.
•Typically smooth and ring-enhancing lesion.
•DWI and MRI are useful in distinguishing abscess from mimics.
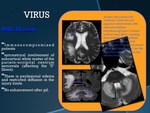
PML: JC virus
•Immunocompromised patients•symmetrical involvement of subcortical white matter of the parieto-occipital centrum semiovale (affecting the ‘U’ fibers).
•There is perilesional edema and restricted diffusion in the injury limits.
•No enhancement after gd.
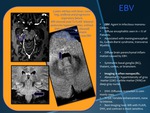
EBV
•EBV: Agent in infectious mononu-cleosis.
•Diffuse encephalitis seen in < 1% ofpatients.
•Associated with meningoencephalitis,
Guillain-Barré syndrome,
transverse myelitis.
•Diffuse brain parenchymal inflammation caused by EBV.
•Symmetric basal ganglia (BG), thalami,
cortex,
or brainstem.
•Imaging is often nonspecific.
•Abnormal T2 hyperintensity of gray matter (GM) ± white matter (WM) or
deep gray nuclei.
•DWI: Diffusion restriction is commonly seen.
•T1 Gd: Variable enhancement,
none to intense.
•Best imaging tool: MR with FLAIR, DWI,
and contrast is most sensitive.
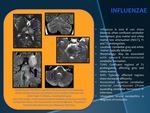
INFLUENZAE
•Influenza A and B can show bilateral,
often confluent cerebellar hemispheric gray matter and white matter low attenuation (NECT),
T1 and T2 prolongation.
•Location: Cerebellar gray and white
matter,
typically bilateral.
•Morphology: May be associated with upward transtentorial cerebellar herniation.
•T2WI: Confluent regions of T2 prolongation,
affecting gray and white matter
•DWI: Typically affected regions show increased diffusivity.
•Associated superior cerebellar arterial compression (from ascending cerebellar herniation) ⇒ infarction.
•Idiopathic acute cerebellitis is diagnosis of exclusion.
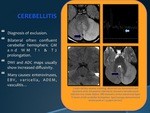
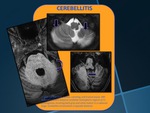
CEREBELLITIS
•Diagnosis of exclusion.
•Bilateral often confluent cerebellar hemispheric GM and WM T1 & T2 prolongation.
•DWI and ADC maps usually show increased diffusivity.
•Many causes: enteroviruses,
EBV,
varicella,
ADEM,
vasculitis…
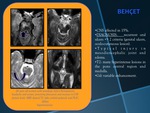
BEHÇET
- CNS affected in 15%.§DIAGNOSIS: recurrent oral ulcers +> 2 criteria (genital ulcers,
oculo-cutaneous lesion).
- Typical injury in mesodiencephalic joint and edema.
- T2: many hyperintense lesions in the pons central region and medulla.
- Gd: variable enhancement.
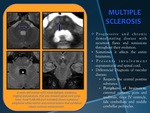
MULTIPLE SCLEROSIS
Progressive and chronic demyelinating disease with recurrent flares and remissions throughout their evolution.
•Sometimes it affects the entire brainstem.
•Presents involvement supratentorial and spinal cord.
•Differencial Diagnosis of vascular disease:
•Respects the central pontine substance.
•Periphery of brainstem: cisternal surfaces,
pons and midbrain,
floor IV ventricle,
falx cerebellum and middle cerebellar peduncles.
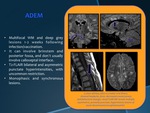
ADEM
•Multifocal WM and deep grey lesions 1-2 weeks following infection/vaccination.
•It can involve brinstem and posterior fossa,
and don´t usually involve calloseptal interface.
•T2-FLAIR bilateral and asymmetric punctate hyperintensities,
with uncommon restriction.
Monophasic and synchronous lesions.
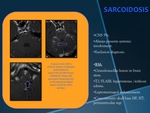
SARCOIDOSIS
- CNS 5%.§Always presents systemic involvement.§Exclusion diagnosis.
- RM:
- Granuloma-like lesion in brain stem.
- T2/FLAIR: hyperintense /without edema.
- Leptomeningeal enhancement
- Concomitant: skull base HF,
HT,
periventricular regions.
CENTRAL PONTINE MYELINOLYSIS:
•Quick replacement from hyponatremia,
RCI,
liver pathology,
MD,
rapid dialysis,
SIADH,
children with AML,
hepatic trasplant,
lymphoma,
Wilson disease,
craniopharyngioma).
•It affects the bridge central region,
without ventral and external affection.
There are two isointense structures = ventral pyramidal tracts.
• no mass effect.
• many areas affected at once: cortical /subcortical (thalamus,
basal ganglia,
caudate,
internal capsule,
external,
extreme,
amygdala,
insula and cerebellum).
• MRI:
•T2: hyperintense lesions.
•No enhances after administration.
•Increased diffusivity.
PONTINE GLIAL TUMORS
•Mass effect / edema / swelling.
•Sometimes extend the cerebellar peduncles.
•Gd: enhancement variable (some degree of uptake,
no significant uptake).
•Exophytic growing lesion
•SPECTROSCOPY / PERFUSION: peak hill.
Perfusion by grade.
Diffuse gliomatosis
•Diffuse infiltrating,
frequently bilateral glial tumor involving at less 3 lobes.
•T2 hyperintense infiltrating mass with enlargement of envolved structures.
•Tipically no or minimal enhancement (enhancement may indicate malignant progression or focus of malignant glioma)
•MRS: Increased choline,
decreased NAA.
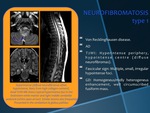
NEUROFIBROMATOSIS type 1
•Von Recklinghausen disease.
•AD
•T2WI: Hyperintense periphery,
hypointense centre (diffuse neurofibromas).
•Fascicular sign: Multiple,
small,
irregular hypointense foci.
•GD: Homogeneus/midly heterogeneus enhancement,
well circumscribed fusiform mass.
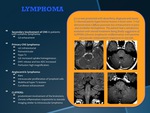
LYMPHOMA
•Secondary involvement of CNS in patients with systemic lymphoma.
•Gd enhacement
•Primary CNS lymphoma:10% infratentorial
•Periventricular Hypo T2
•Gd: increased uptake homogeneous.
•DWI: release and low ADC increased
•Perfusion: high magnification.
•Angiocentric lymphoma:Rare
•Intravascular proliferation of lymphoid cells
•Multifocal hyper T2 lesions
•Curvilinear enhancement
•CLIPPERS:
•predominant involvement of the brainstem,
•Chronic inflammation responsivle to steroids
•Imaging similar to intravascular lymphoma
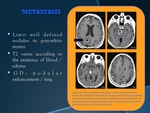
METASTASIS
•Limit well defined nodules in gray-white matter.
•T2 varies according to the existence of blood / edema.
•GD: nodular enhancement / ring.
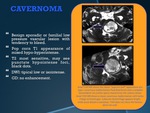
CAVERNOMA
•Benign sporadic or familial low pressure vascular lesion with tendency to bleed.
•Pop corn T1 appearance of mixed hypo-hyperintense.
•T2 most sensitive,
may see punctate hypointense foci,
black dots.
•DWI: tipical low or isointense.
•GD: no enhancement.
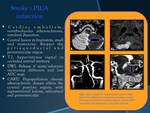
Stroke : PICA infarction
•Cardiac embolism,
vertebrobasilar atherosclerosis,
vertebral dissection.
•Central lesion in brainstem,
small and numerous.
Respect the periaqueductal and periventricular region.
•T2: hyperintense signal in occluded arterial territory.
•DWI: Release if acute/subacute: increasing diffusion and low ADC map.
•CARE! Hypoperfusion chronic atherosclerotic disease affects the central pontine region,
with supratentorial lesions,
subcortical and periventricular.
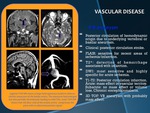
V-B aneurysm
•Posterior circulation of hemodynamic origin due to underlying vertebral or basilar aneurysm.
•Clinical: posterior circulation stroke.
•FLAIR: sensitive for recent areas of ischemis/infarction.
•T2*: detection of hemorrhage associated with infarction.
•DWI: most sensitive and highly specific for acute ischemia.
•T1-T2: Posterior circulation infarction.
Acute: mass effect in vascular territoy.
Subacute: no mass effect or volume loss.
Chronic: encephalomalacia.
- 3D TOF: VB aneurysm with probably mass effect.
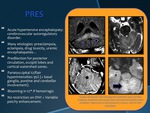
PRES
•Acute hypertensive encephalopaty: cerebrovascular autoregulatory disorder.
•Many etiologies: preeclampsia,
eclampsia,
drug toxicity,
uremic encephalopaties…
•Predilection for posterior circulation,
occipitl lobes and cortical watershed zones.
•Parietoccipital t2/flair hyperintensities 95% (+ basal ganglia,
pontine and cerebellar involvement).
•Blooming in t2* if hemorragic
•No restriction on DWI + Variable patchy enhancement.