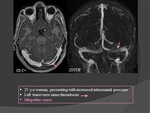
46 patients (33 women) with a mean age of 38,7 years were analyzed.
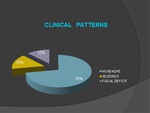
- In our study The most frequent clinical pattern was headache (70%) followed by seizures (15 %) and focal neurologic deficits (12%).(Fig.
9)
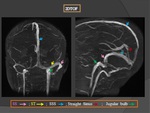
- The most frequent site of venous occlusion was superior sagittal sinus followed by lateral sinus.
Clinical Manifestations
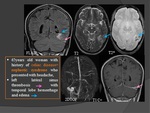
Cerebral venous thrombosis has a wide spectrum of clinical manifestations and modes of onset that may mimic many other neurological disorders and lead to frequent misdiagnoses or delay in diagnosis.
1.
Headache:
- The most common symptom of CVT.
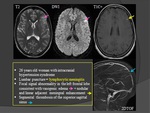
- May occur in a context of isolated intracranial hypertension.
- May also be the only symptom and occurs in the absence of intracranial hypertension,
subarachnoid hemorrhage or meningitis.
2.
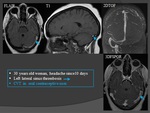
Isolated focal neurological deficits:
The diagnosis is sometimes easy because of the pre-existence of unusual headache or a predisposing condition known to be at high risk of CVT,
such as puerperium.
3.
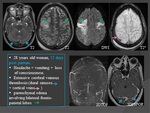
Diffuse encephalopathies with seizures:
In patients with parenchymal lesions,
the clinical picture is more severe and may include at various degrees:
- coma,
- motor deficits or aphasia,
- seizures (focal or generalized seizures,
including status epilepticus).
4.
Other clinical presentations:
- attacks of migraine with aura,
- isolated psychiatric disturbances,
- pulsatile tinnitus,
- isolated or multiple cranial nerve involvement,
- subarachnoid hemorrhage.
Diagnosis of CVT
I) Neuroimaging of the thrombosed vessel and parenchymal abnormalities
1) CT FINDINGS
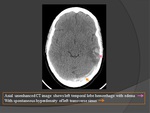
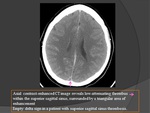
a) UNENHANCED CT : (Fig.
10)
- Hyperdense dural sinus or cortical vein ("cord sign")
* Cortical/subcortical petechial hemorrhages,
edema
* Thrombosis of internal cerebral veins,
vein of Galen: thalami/basal ganglia hypodense
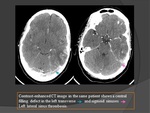
b) CONTRAST-ENHANCED CT : (Fig.
11;12)
- "Empty delta" sign in 25-30% of cases
* Enhancing dura surrounds non enhancing thrombus
- "Shaggy," irregular veins (collateral channels)
c) CT-VENOGRAPHY
- early stage : non-enhancement of the thrombosed vein
- later stage : non-enhancement of the thrombus with surrounding enhancement : empty delta sign.
- Unlike MR,
CT-venography virtually has no pitfalls..
- we advocate 45-50 seconds delay after the start of contrast injection.
- We use at least 70 cc of contrast
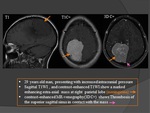
2) MRI FINDINGS
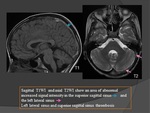
a) T1WI : (Fig.
13)
- Acute thrombus (0–5 days): isointense.
- Subacute thrombus (6–15 days): becomes hyperintense.
- Chronic thrombosis with incomplete recanalization of the sinus (>15 day-old): isointense
b) T2WI: (Fig.
13)
- Clot initially hypointense.
* Caution: If thrombus is hypointense,
can mimic normal sinus "flow void" on T2WI
- Subacute thrombus appears hyperintense.
- Chronically occluded,
fibrotic sinus eventually appears isointense or hyperintense.
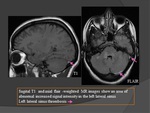
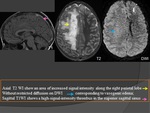
c) FLAIR: (Fig.
14)
- Thrombus: hyperintense.
- Venous infarcts: hyperintense.
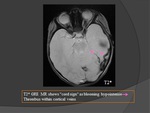
d) T2* GRE: (Fig.
15)
- 90% have hypointense clot in occluded vessel on the first MRI-scan
- Additional value for the diagnosis of CVT,
particularly:
- in isolated cortical venous thrombosis
- at the very early stage when T1 and T2- sequences are not sensitive enough.
- Petechial and/or parenchymal hemorrhages: hypointense
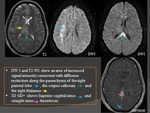
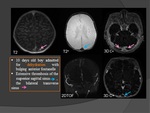
e) DWI(Fig.
16;20)
- 40% have hyperintense clot in occluded vessel.
- DWI findings in parenchyma variable,
heterogeneous:
- vasogenic edema (with increased ADC values presumably related to venous congestion),
- cytotoxic edema (with decreased ADC values related to cellular energy disruption),
- Hemorrhage may occur with both types of edema,
- Various patterns may coexist in the same region.
In contrast with arterial ischemic states,
many parenchymal abnormalities secondary to venous occlusion are reversible.
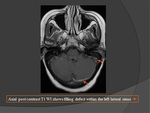
f) T1 C+(Fig.
17)
- Peripheral enhancement around acute clot.
- Chronic sinus thrombosis can enhance due to organizing fibrous tissue.
- Contrast enhancement of the sinus on MR images does not definitively indicate patency,
and venography usually is necessary for a definitive diagnosis.
- Parenchymal enhancement,
may be seen in areas of cytotoxic or vasogenic edema and in the presence of either irreversible or reversible brain abnormalities.
- Increased tentorial enhancement,
adjacent leptomeningeal enhancement,
prominent cortical venous enhancement also may be visible.
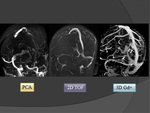
g) MRV
The MR-techniques that are used for the diagnosis of cerebral venous thrombosis are:
Time-of-flight (TOF),
phase-contrast angiography (PCA) and contrast-enhanced MR-venography (3D Gd+) (Fig.
18)
- TOF angiography is based on the phenomenon of flow-related enhancement of spins entering into an imaging slice.As a result of being unsaturated,
these spins give more signal that surrounding saturated spins.
* Absence of flow in occluded sinus on 2D TOF MRV(Fig.
19)
* "Frayed" or "shaggy" appearance of venous sinus
* Abnormal collateral channels
* Tl hyperintense (subacute) clot can masquerade as flow on MRV,
evaluate standard sequences and source images to exclude artifacts
- PCA uses the principle that spins in blood that is moving in the same direction as a magnetic field gradient develop a phase shift that is proportional to the velocity of the spins.
* PCA not limited by Tl hyperintense thrombus
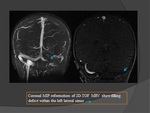
- Contrast-enhanced MR-venography uses the T1-shortening of Gadolinium.
better demonstrates thrombus,
small vein detail,
and collaterals,
much faster than 2D TOF (Fig.
20).
II) other investigations
1.
Lumbar Puncture:
- There are no pathognomonic features
- Abnormalities are found in up to 84% of cases and include raised CSF pressure,
increased protein content,
the presence of red blood cells and pleocytosis.
2.
Screening with D-dimer test:
- Negative D-dimer has high negative predictive value.
- Normal value does not go against CVT.
3.
Etiological investigation:
investigation for:
- prothrombotic states,
- coagulopathies,
vasculitis,
- other biochemical parameters like serum homocystiene are indicated.
Etiology of CVT
The causal factors in our study were:
Infectious (n=11),
gyneco obstetric (n=9),
systemic (n=14),
local (n=2) and unknown(n=10).
(Fig.
21)
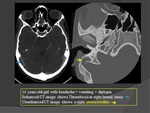
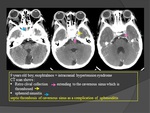
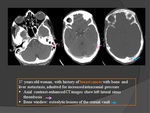
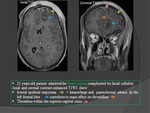
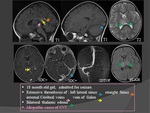
1. Infectious causes :(Fig.
22=>26)
- Intracranial infectious process: abscess,
subdural empyema,
meningitis.
- Parameningeal infections (ear,
sinus,
mouth,
face,
and neck).
- Sepsis and systemic infection.
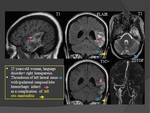
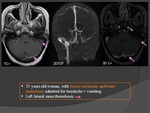
2. Gyneco obstetric causes: (Fig.
27;28)
- In young women,
CVT occurs more frequently during the puerperium than during pregnancy.
- The use of oral contraceptives is associated with an increased risk of CVT+++.
- The great majority of younger nonpregnant women with CVT are oral contraceptive users.
- The risk of CVT with oral contraceptive use in women is greater among those with a hereditary prothrombotic factor.
3.
Systemic causes: (Fig.
29=>35)
a) Genetic prothrombotic disorders:
- The hereditary resistance to activated protein C caused by the mutation in factor V Leiden is the most common.
- Less common are deficiencies in protein C,
protein S,
and ATIII.
b) Acquired hypercoagulable disorders:
- Disseminated intravascular coagulation,
- heparin-induced thrombocytopenia,
- plasminogen deficiency,
- epsilon aminocaproic acid treatment,
- sickle cell disease,
- polycythemia vera,
-
paroxysmal nocturnal hemoglobinuria,
-
thrombocythemia,
-
antiphospholipid antibody syndrome,
-
nephrotic syndrome,
-
dehydration (Changes in blood flow/viscosity).
-
thyrotoxicosis,
-
hypercoagulability associated with malignancy,
-
anemia due to iron deficiency.
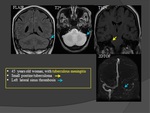
c) Inflammatory disorders:
Cerebral venous thrombosis may be the first manifestation of an inflammatory systemic disease such as:
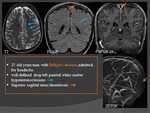
- Behçet disease,
- lupus erythematosus,
- sarcoidosis,
- ulcerative colitis,
- crohn disease,
- Wegener granulomatosis.
4.
Local causes: (Fig.
36)
- Head trauma with skull fractures extending to a dural venous sinus or jugular bulb.
- Intracranial surgeries
5.
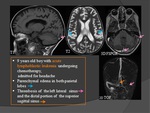
Idiopathic causes: (Fig.
37; 38)
- The proportion of cases of unknown etiology remains high,
between 20% and 35% .
- In these cases,
even after an extensive initial evaluation is performed,
repeated investigations are advisable.
Potential Pitfalls in Image Interpretation
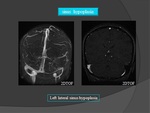
1.
Sinus Hypoplasia: (Fig.
39)
- Hypoplasia and atresia of the transverse sinuses occur frequently.
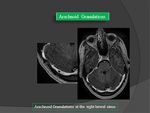
2.
Arachnoid Granulations: (Fig.
40)
- Arachnoid granulations are normal structures that protrude into the dural sinus lumen or lateral lacunae.
- Arachnoid granulations typically have signal intensity and attenuation similar to those of cerebrospinal fluid and appear as focal rounded filling defects with a characteristic anatomic distribution: usually identified in the lateral part of the transverse sinus,
near the entrance sites of the Labbé vein.
- When they are prominent,
they may simulate sinus thrombosis.