Imaging features associated with ABCB4/MDR3 mutations are not specific and correspond to a wide spectrum of biliary abnormalities.
The main findings is the presence of intrahepatic lithiasis :
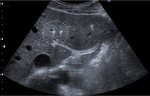
US examination is very accurate in detecting intrahepatic stones : they appear as heterogeneous and echoic foci centered on the intrahepatic ducts,
or as "comet-tail artifact" due to US reverberation (figure 1).
If Endoscopic Retrograde Cholangiopancreatography (ERCP) has been considered as the gold standard for diagnosing bile duct stone,
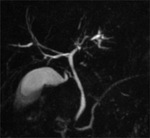
Magnetic Resonance Cholangiopancreatography (MRCP) is a non-invasive alternative technique that has been shown equivalent to ERCP in choledocholithiasis diagnosis and superior to ERCP in intrahepatic lithiasis diagnosis.
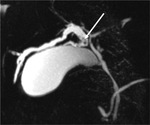
Magnetic Resonance Cholangiopancreatography (MRCP) shows the presence of round or oval shape signal voids in the lumen of the bile ducts on heavily T2-weighted sequences (figures 8,9).
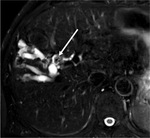
Stones may have high signal on T1-wheighted sequences (figure 7) or strong hypointensities on T1-weighted acquisitions (figure 11). The stones appear as endoluminal signal voids on T2-weighted acquisition (figures 6,
10).
A complementary exploration by US and MRI should be recommended because MR is not able to detect very small stones,
while US may be difficult in case of massive intraluminal stones (figure 2).
Atypic features are :
- Bile ducts dilatations :
When bile duct dilatations are present,
they appear as mild to moderate.
Rarely,
patients may present with more severe dilatations (<10%).
Such severe bile duct dilatation may only involve one or two liver segments (figures 3,4,5) or may be diffuse.
In such cases,
and as opposed to ductal plate malformations (Caroli disease,
congenital hepatic fibrosis,
congenital cystic anomalies of the common bile duct,
etc),
which are directly related to abnormal embryologic development of the bile ducts,
abnormalities are related to a biliogenesis disorder developed on initially normal ducts.
Anomalies are a consequence of the chronic alteration of the bile composition and the aggression of the bile epithelium and consist in uni or multifocal noncystic large spindle-shaped bile duct dilatations that can concern one to several hepatic segments,
associated with regular non-dilated ducts.
However,
ductal plate malformations,
particularly the Caroli disease,
have to be ruled out by the absence of specific features,
such as the “central dot sign”,
dilated bile ducts associated with focal area of cystic ectasia,
or the fact that no biliary dilatation can be found in LPAC syndrome without underlying biliary stones.
Other possible differential diagnosis is bile duct dilatations related to focal obstacle on the biliary ducts.
Traditionally,
downstream-acquired stenosis (iatrogenic,
biliodigestive anastomosis,
sclerosing cholangitis,
cholangiocarcinoma) may lead to obstructive dilatations that appear more central without intrahepatic lithiasis.
- Sclerosing cholangitis (figure 12,
13)
In mice,
the multidrug resistance (MDR) glycoproteins that mediate the translocation of phosphatidylcholine across the canalicular membrane of the hepatocyte,
and corresponding to MDR3 in man,
is called MDR2.
Whereas the main feature in mdr2 knock-out mice,
which corresponds to the equivalent animal model of human MDR3 deficiency,
is sclerosing cholangitis,
controversies exist whether a genetically determined dysfunction of MDR3 plays a pathogenic role in primary biliary cirrhosis and primary sclerosing cholangitis (PSC) in humans.
Pauli-Magnus et al.
found no genetic argument supporting the role of MDR3 in PSC.
Since then,
concepts in PSC understanding have evolved and many authors consider that PSC may represent a mixed bag of diseases of different etiologies in which several genes such as ABCB4/MDR3 may play a disease modifier role .
To support this conceptual view,
our group recently reported for the first time,
in a series of 13 patients with MDR3 deficiency,
imaging presentations mimicking sclerosing cholangitis in 2 patients at MR (Figure 12).
They corresponded to small duct fibro-obliterative lesions at pathology,
and may be due to the direct toxic effect of biliary acids on epithelioma.
To our knowledge this is the only report of such association of MDR3 deficiency and secondary sclerosing cholangitis but the two patients presented with recurrent cholangitis and not LPAC syndrome per se.
All complications associated with chronic cholangitis and/or cholelithiasis have been described in patients with LPAC syndrome: intrahepatic cholangiocarcinoma (figures 14,
15,
16,
17),
portal hypertension,
superinfection (figure 18),
hepatic fibrosis or cirrhosis.
Intrahepatic cholangiocarcinoma is a rare primary liver tumor (10-20%).
Recently,
Tougeron et al.
reported 2 cases of IHCC in different and unrelated families with MDR3 deficiency.
In both cases,
no argument supporting the direct relation between ABCB4 mutations and tumorogenesis was found and IHCC may be considered as a consequence of the chronic biliary abnormalities.
Genetic polymorphisms in biliary transporters genes have been studied but,
to date,
no relation has been established between IHCC and ABCB4 mutations.