CONGENITAL CYSTIC MALFORMATIONS AFFECTING THE LUNGS
CPAM
Formerly called congenital cystic adenomatoid malformation or CCAM,
the congenital pulmonary airway malformation or CPAM is the result of an abnormal development of the bronchial tree.
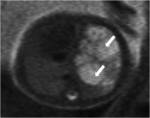
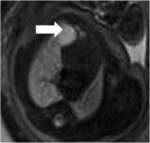
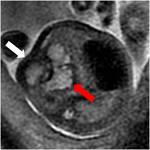
Most of these lesions appear in prenatal imaging as a multicystic mass (Fig.1) occupying one lobe.
Macrocystic or microcystic types can be determined by imaging. Evolution of these lesions can widely vary in each patient:while some lesions may even disappear others may cause foetal hydrops and stillbirth.
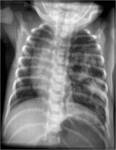
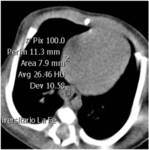
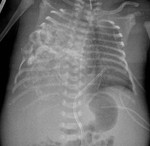
Postnatal imaging must start with a chest plain film (Fig.2) to confirm the diagnosis and evaluate its extent and complications like mediastinal shift,pleural effusions,etc.
Symptomatic CPAM are normally managed with surgical resection in first week of life.
On the other hand,
management of asypmtomatic CPAM is controversial although most advocate elective resection because of risks of infection and malignancy.
In our Hospital these patients are postnatally followed and at 6 months of age a CeCT is performed as a previous step to elective surgery.
DIAPHRAGMATIC HERNIA (DH)
We include congenital DH in this group as an important differential diagnosis of CPAM in prenatal imaging.
Although currently DH are usually detected prenatally some may present late in pregnancy and suddenly present at birth or in the first days of life,being one of the most important surgical causes of neonatal respiratory distress to be recognised by radiologists.
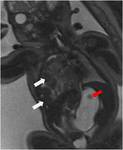
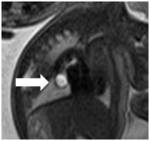
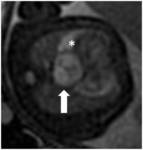
DH may be prenatally diagnosed by US but lately MRI (Fig.3) has proven its capability to better determine DH important features like contralateral pulmonary hypoplasia,liver-up herniation,etc.
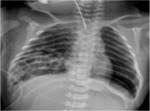
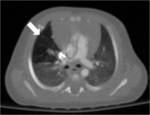
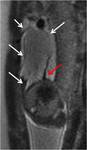
Postnatally,a neonatal chest radiography showing bubble-like lucencies within the chest with a dilated gastric bubble and paucity or absence of abdominal gas (Fig.4) is usually enough to make the right diagnosis.
Surgery will be necessary to repair the diaphragmatic congenital defect.
BRONCHOPULMONARY SEQUESTRATION (BPS)
BPS is a congenital area of abnormal lung whose origin is similar to the other entities like CPAM.
It is a dysplastic lung without connection to the bronchial tree but with systemic arterial supply (typically arising from descending aorta).
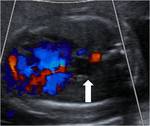
It usually presents as an echogenic lung mass in prenatal US with doppler demonstration of the arterial supply.
BPS seldom has cystic nature but it may occur in conjunction with cystic lesions as CPAM.
This form of BPS+CPAM is called hybrid lesion and in our experience is not so rare as an association.
Therefore,
one should always try to detect arterial supply in a CPAM or in a congenital solid pulmonary lesion to rule out this sort of lesions.
BRONCHOGENIC CYST (BC)
BC are developmental lesions that are part of the family of foregut duplication cysts.
They most commonly appear as a solitary well-defined cystic mass in the paratracheal or subcarinal region of the mediastinum,although some of them can be located intrapulmonary and can be indistinguishable from CPAM.
BC are homogenously hypoechoic in US and hyperintense on a T2-weighted prenatal MRI sequence (Fig.5).
Postnatally, depending on the size and location of the BC the clinical impact will be different.
When they are big,
airway or esophageal compression can be present.
If they are small they cannot even be identified in a chest radiograph. Usually CT or MRI are needed for further evaluation (Fig.6).
Surgical resection is recommended.
BRONCHIAL ATRESIA (BA)
BA is a rarecongenital atresia of a proximal segmental bronchus with normal distal architecture.
It normally affects apicoposterior segment of Left upper lobe.
It can be detected in utero or most commonly in neonatal period being similar to CPAM in appearance.
CT usually allows for more definite diagnosis showing a tubular branching mass surrounded by hyperinflated lung (Fig.7)
CONGENITAL CYSTIC MALFORMATIONS NOT AFFECTING THE LUNGS
LYMPHANGIOMAS (LYMPH.)
Lymph.
can be detected as early as in fetal period with prenatal US.
They appear like big cystic masses normally arising in the lateral regions of the neck.
20 % of them do not affect the neck but may affect the chest region.
The most frequent here are axillary limph. growing as cystic masses between the arm and the chest wall (Fig.8).
Sometimes,the patients can show multiple lymphangiomas and the medastinum is commonly affected (Fig.9).
MEDIASTINAL and PERICARDIAL TERATOMA
Fetal tumors are very rare.
The most common are teratomas but those growing in fetal chest are even rarer.
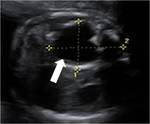
They may appear as a heterogeneous mass with calcifications in the superior mediastinum so the diagnosis is quite easy, but sometimes it can adopt a confusing "benign"aspect in prenatal US (Fig.10) and finally continue growing next to the heart and then develop as a mass within the pericardium.
MRI can add valuable information.
In pericardial teratomas the presence of pericardial effusion is the key point (Fig.11).
CHEST WALL TUMOR (mesenchymal hamartoma,
MH)
It is very uncommon to find chest wall tumors in fetal period.
There are some of them described in the literature.
When they grow within the chest,
and present cystic nature like the MH, they could mislead to a CPAM diagnosis (Fig.12).
Fetal MRI here is very useful to identify and determine the origin of these confusing lesions (Fig.13).
Anyway,most of these extremely rare tumors are normally diagnosed postnatally (Fig.14).
Mesenchymal hamartomas are benign lesions arising from the ribs and can be detected in utero.
Despite its benign origin they can produce fetal demise secondary to mediastinal compression.