Patients
This study was approved by our hospital ethics committee,
and informed consent was obtained from all patients.
From January through June 2011,
we prospectively selected patients scheduled for total knee arthroplasty due to severe osteoarthritis (Kellgren-Lawrence grades 3 and 4).
Patients with inflammatory or infectious arthritis,
and those with a history of a previous knee injury or previous knee surgery were excluded.
Initially,
61 ACLs were harvested from 58 patients (49 women,
9 men,
age range; 52-84 years,
mean age; 70.4 years).
Cases in which pathologic and imaging studies were difficult to perform due to severely deformed or missed bundles were excluded.
Finally 53 ACLs in 50 patients (43 women,
7 men,
age range; 55-84 years,
mean age; 69.3 years) were included in this study.
In addition,
10 healthyl volunteers (8 men,
2 women,
age range; 25-35 years,
mean age; 30.4 years) without any knee joint symptom or previous knee injury were included.
MR examinations
All patients underwent MR examinations one day before surgery.
MR imaging was performed with a 1.5 T magnet (Magnetom Avanto TIM; Siemens Medical Systems,
Erlangen,
Germany) using a dedicated send/receive 8-channel phased array knee coil.
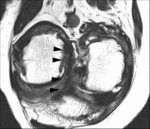
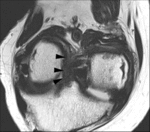
The MR imaging protocol consisted of oblique coronal turbo spin echo T2-weighted and T2* mapping images.
Oblique coronal planes were obtained in the plane parallel to the course of the femoral intercondylar roof on sagittal scout images to maximize visualization of the AM and PL bundles of the ACL.
Although the use of sagittal oblique MRI,
parallel to the long axis of the ACL,
has been advocated by some authors,
we used oblique coronal MRI parallel to the femoral intercondylar roof,
as was previously used by Hong et al’s (17).
Oblique coronal T2-weighted imaging parameters were TR/TE 3000 ms/ 101 ms,
3-mm slice thickness,
384 x 269 matrix,
160 x 160 mm field of view (FOV),
and an echo train length (ETL) of 7.
The total scanning time for this sequence was 3 minutes 23 seconds.
Oblique coronal T2* mapping parameters were TR/TE of 689 / 4.2,
3-mm slice thickness,
256 x 179 matrix,
180 x 180 mm FOV,
ETL of 1 and the total scanning time for this sequence was 3 minutes 32 seconds.
Imaging analysis
Oblique coronal T2-weighted MR images were reviewed by consensus of two musculoskeletal radiologists with 9 and 2 years of MRI experience on a PACS monitor.
The two reviewers were unaware of pathologic results or gross findings.
To evaluate ACL status,
AM and PL bundles were analyzed separately.
As previously described (2,
5) it was found that the AM and PL bundles originated from the anterior-proximal and posterior-distal aspect of the femoral attachment.
At the tibial insertions,
the AM bundle inserted anteromedially and the PL bundle posterolaterally.
Image analyses of oblique coronal T2-weighted image were performed using different two methods as previously described (6,
18,
19).
First,
the statuses of the AM and PL bundles were graded using a 5-point system (grades 0-4) for comparison with pathologic findings.
A grade 0 indicated an intact bundle,
that is,
a continuous band of low signal intensity from the femoral to the tibial attachments; a grade 1 indicated abnormal high intrasubstance signal or a subtly wavy contour with definable intact ligamentous fibers in less than quarter of a bundle; grade 2 indicated a signal change and a wavy contour in less than half of a bundle; grade 3 a signal change and a wavy or lax contour or severe atrophy affecting more than half of a bundle; and grade 4 indicated a complete disruption or complete replacement of the bundle by an edematous mass.
Second,
ACL tear statuses were simply classified as normal (grade 0,1),
partial (grade 2,
3),
or complete tear (grade 4) for comparison with gross finding in the operative field.
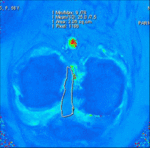
On T2*-mapping images,
we measured regions of interest (ROIs) on AM and PL bundles at a workstation (Leonardo,
Siemens Medical Solution).
An ROI was drawn over the whole area of bundles in each image slice.
Corresponding oblique coronal T2-weighted images served as references for the accurate placement of ROIs within bundles.
If AM or PL bundles are visible in more than one slice,
the mean value of summed ROI values in each slice was obtained and used in the analysis.
To standardize the procedure,
all measurements were performed by a single investigator.
To test the reproducibility of measurements,
ROI measurements were carried out a second time for each AM and PL bundle by the radiologist who had performed the original assessment.
The radiologist was blinded to histologic and operative gradings and to first measurement results.
Operation and Pathology
ACL statuses were determined by two orthopaedic surgeons (KDJ,
SJT),
who separated AM and PL bundles,
before and after ACL harvest in the operative field.
The analysis list was as follows; the presence or absence of synovial coverage and synovial inflammation,
and continuity,
fraying,
delamination and shrinkage of bundles.
Gross findings also were graded according to the imaging grades; grade 0 – normal appearance,
grade 1 – only one finding among synovial problem such as no synovial coverage or synovial inflammation,
fraying or delamination with maintenance of continuity,
grade 2 – a synovial problem plus delamination or fraying with maintenance of continuity,
grade 3 – a synovial problem plus fraying or delamination and shrinkage with maintenance of continuity,
and grade 4 – discontinuity or poor fiber delineation due to severe shrinkage.
In addition,
for comparison with imaging grades,
we also modified the above grading with normal (grade 0,
1),
partial (grade 2,3) or complete tear (grade 4).
ACLs were harvested by sharp incision from the bone-ligament junctions of femurs and tibiae.
Proper specimen orientation was maintained by placing a mark on the anterior tibial side of harvested ligaments.
AM and PL bundles were gently separated by one pathologist (C.K.W),
in consultation with an orthopaedic surgeon (K.D.J).
Each specimen was fixed in 10% formalin,
embedded in paraffin,
cut longitudinally,
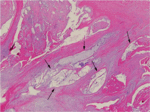
and stained with Hematoxylin and Eosin for histological evaluations.
Histological appearance was evaluated using a semiquantitative scoring system,
which included the amount of loose collagen fiber,
fibrosis,
cystic changes,
chondroid metaplasia and mucoid degeneration.
The degenerative changes were categorized as normal,
slight,
mild,
moderate or marked according to Kleinbart’s criteria (20).
Normal (0) was defined as no microscopic abnormalities,
slight (1) when microscopic changes were observed in one high-power microscopic field (magnification ×400),
mild (2) when histologic changes were noted in several fields,
moderate (3) when a significant portion of the ligament was involved,
and marked (4) when there was a confluence of the microscopic fields.
The sections were examined and graded by the pathologist in a blind manner.
Statistical analysis
Linear regression analysis and Pearson correlation coefficients were used to establish the correlation between the ROI values of AM or PL bundles on T2* mapping images and pathologic,
operative grades and imaging grades on T2-weighted MR images.
In addition,
the correlations between ROI values,
pathologic,
gross and imaging grades,
and age and sex were sought using linear regression analysis.
Wilcoxon’s signed-rank test was used to investigate the difference between 1st and 2nd measurements of ROI values.
Kappa statistics were used to evaluate degree of agreement between pathologic grades,
visual grades from operative fields or gross specimens,
and imaging grades on oblique coronal T2-weighted and T2* mapping images.
Level of agreement were assessed using kappa values as previously described by Landis and Koch: a negative kappa value was interpreted as poor agreement,
0.00 – 0.20 as slight agreement,
0.21 – 0.40 as fair agreement,
0.41 – 0.60 as moderate agreement,
0.61 – 0.80 as substantial agreement,
and greater than 0.81 as almost perfect agreement.
Using operative findings as reference standards,
sensitivity,
specificity,
and accuracy of oblique coronal T2-weighted images and T2* mapping images for the diagnosis of complete and partial tears about each AM and PL bundle were calculated using simple bundle status.
Statistical software (SPSS version 13; SPSS Inc.) was used for analyses and statistical significance was accepted for p values < 0.05.