1.
INTRODUCTION
2.
INFLAMMATORY ARTHRITIS
- Rheumatoid arthritis
- Seronegative Spondyloarthropathies
3.
CRYSTAL DEPOSITION ARTHROPATHIES
- Gouty Arthritis (Monosodium Urate Crystal deposition disease)
- Calcium Pyrophosphate Dihydrate (CPPD) Crystal Deposition Disease
4.
CONNECTIVE TISSUE ARTHRITIS
- Scleroderma
- Dermatomyositis
5.
ARTHROPATHIES COMPLICATIONS
...........................................
1.
INTRODUCTION
- The arthropathies specific diagnosis is based upon:
1.
Clinical data
2.
Laboratory features
3.
Radiographic features:
A slow,
insidious onset,
with developing symptoms over several months required an X-ray study including:
- PA and oblique projection of both hands
- AP projection of both knees
- AP projection of pelvis
- Lateral projection in cervical spine flexion.
2.
INFLAMMATORY ARTHROPATHIES
2.1 RHEUMATOID ARTHRITIS (RA)
- It is an autoimmune disease characterized by chronic inflammation of synovial joints.
- It is more common in women (2-3:1).
Starting age between 20 and 55 years.
- Clinical presentation: polyarthralgia,
morning joint stiffness,
nonspecific general symptoms (fatigue,
weight loss,
fever).
Positive rheumatoid factor (75%).
- Localization: HANDS AND FEET (80-90%) (Figures 1 and 2),
knees (80%),
cervical spine (50%)
- Peripheral skeleton injuries distribution is BILATERAL and SYMMETRICAL
- Typical radiologic changes in involved joints:
Subluxations
Osteoporosis
Uniform decreased joint space
Erosions
Soft tissue swelling
- There are two phases with early and late radiographic changes:
Radiologic Changes of Early Rheumatoid Arthritis (figure 3)
1.
Joint space widening (earliest and most transient finding)
2.
Soft tissue swelling usually symmetrical at the metacarpophalangeal (MCP) and proximal interphalangeal (PIP) joints
3. Periarticular osteoporosis
4.
Partial or complete interruption of the cortical white line on the radial aspect of the fourth and fifth metacarpal heads representing subtle erosions.
5.
Marginal erosions on the bare areas of bone,
at MCP and PIP joints.

Fig. 3: Radiograph (detail view) of the hand shows radiologic changes of early RA
a. Periarticular osteoporosis
b. Subtle erosions on the radial side of proximal phalanges
c. Soft tissue swelling
Radiologic Changes in late-stage rheumatoid arthritis
(figures 4,
5,
6 and 7)
- Soft tissue inflammatory destruction causes joint subluxation or luxation,
most frequently ulnar deviation of the second to fifth MCP joints
- Erosions may lead to severe destruction and mutilation with bone deformity.
- Diffuse osteoporosis
- Uniform and symmetrical joint space narrowing
- In advanced stages the inflammatory injury may lead to bony ankylosis

Fig. 4: Radiograph of the hand shows radiologic changes of late-stage RA: Subluxations with ulnar deviation of the second to fifth MCP joints, diffuse osteoporosis and symmetrical joint space narrowing of the MCP, PIP and carpal joints.
- Bilateral and symmetrical involvement of foot joints (80-90%) (Figure 8) is another typical manifestation of RA.
Later in the course of the disease,
large joints like knees (80%) (Figure 9),
and cervical spine (50%) may be affected.
(Figure 10)

Fig. 8: Radiograph of the feet shows Subluxation with peroneal deviation of the 2th to 5th metatarsaphalangeal (MTP) joints, hallux valgus and erosions on the phalanges base and metatarsals head. Tarsal ankylosis.
2.2 SERONEGATIVE SPONDYLOARTHROPATHIES
- It is a general term for a group of arthritis disorders that involve predominantly cartilaginous joints and entheses and may have overlapping symptoms (low back pain,
back stiffness...).
The subtype of spondyloarthropathies is usually distinguished on the basis of patient history and clinical findings.
2.2.1 Ankylosing spondylitis
2.2.2 Psoriatic arthritis
2.2.3 Arthritis associated with inflammatory bowel disease
2.2.1 ANKYLOSING SPONDYLITIS
- It is a chronic and progressive inflammatory arthritis.
- It is more common in men (3:1).
Starting age between 20 and 55 years.
- It has been shown to have a strong association with HLA B27.
- It manifests as a bilateral and symmetrical arthritis of the axial skeleton that involve the sacroiliac joint and the spine.
- Typical radiologic findings:
Sacroiliac joint (Figure 11)
The early changes of the disease are detected at the sacroiliac joint as a loss or blurring of the subchondral cortex.
It is followed by the development of small erosions (“rat bite erosions”) along the iliac side of the joint.
As the disease progress the erosions become larger and sclerosis around the joint becomes more prominent.
In late stages joint ankylosis develops.

Fig. 11: Radiograph of the pelvis shows changes at the sacroiliac joint.
a. Small erosions (grade II sacroiliitis)
b. Bone ankylosis at the sacroiliac joint. Right hip joint space narrowing. Left hip prothesis. Bamboo cane column.
Spine (Figure 12)
Radiologic changes begin symmetrically at lumbar spine and extend to dorsal and cervical spine.
- Romanus lesions: small erosions at the anterior corner of the vertebral body.
- Syndesmophytes: new bone formation along the anterior aspect of the vertebral body.
- Square vertebral bodies
- The ligaments may ossify and give the image of “bamboo cane column”.
- Ankylosis of the facet joints.

Fig. 12: Radiograph (detail view) of the lumbar spine
a. Syndesmophytes
b. Square vertebral bodies
c. Bamboo cane column
Enthesitis: typical locations include the iliac crest,
ischial tuberosity,
greater trochanter,
calcaneus and greater tuberosity)
Other joints involved include hip,
shoulder and knee.
2.2.2 PSORIATIC ARTHRITIS
- Psoriasis is a chronic inflammatory disease of the skin.
It has a prevalence of 1-2% of the population.
- Psoriatic arthritis affects 5-8% of the psoriatic population.
Nail involvement is the only clinical feature indicating that patients with psoriasis are likely to experience arthritis.
- It has and equal male to female ratio.
Starting age between 30 and 50 years.
- Patients may have variable clinical presentation: monoarthritis or oligoarthritis with enthesitis,
or axial involvement (sacroiliac joint and spine).
- The most frequent presentation is as a bilateral and asymmetric oligoarthritis that involve PIP and distal interphalangeal (DIP) joints of hand and foot.
- Dactylitis,
a fusiform soft tissue swelling,
is a characteristic feature of psoriatic arthritis seen in one third of patients.
- Typical radiologic findings: (Figure 13)
- Normal mineralization
- Bone erosions: typically begin at the margins of the joint and progress along the articular surface giving “pencil in cup” images in late stages.
- Bone proliferation is prominent and is the most typical feature (adjacent to erosions or at the enthesis).
- Soft tissue swelling (sausage toe)

Fig. 13: Radiograph (detail view) of the hand shows:
a. Bone erosions at DIP joints
b. Bone proliferation adjacent to PIP joints and soft tissue swelling (sausage toe)
c. "Pencil in cup" erosions in late stage psoriatic arthritis.
2.2.3 ARTHRITIS ASSOCIATED WITH INFLAMMATORY BOWEL DISEASE
- It is an arthritis associated with inflammatory bowel disease (ulcerative colitis,
Crohn disease,
Whipple disease)
- Arthritis lesions may affect the axial and peripheral skeleton
- It is more frequent as a bilateral and symmetrical sacroiliitis,
similar to ankylosing spondylitis.
Changes that affect the spine can include syndesmophytes and square vertebral body (Figure 14)
3.
CRYSTAL DEPOSITION ARTHROPATHIES
3.1.
GOUTY ARTHRITIS
- It is a metabolic disease characterized by acute arthritis in early stage and monosodium urate monohydrate crystals deposits (tophi) within or around the joints in advanced stages (chronic tophaceous gout)
- More frequent in males (20:1) and postmenopausal women.
Predominant in males (20:1).
- Articular involvement distribution is variable,
but it is most frequently as an asymmetric and POLYARTICULAR disease.
- The disease shows predilection for lower extremity joints.
The most common sites are the feet (first toe),
ankle,
knee and elbow.
- Typical radiologic findings of chronic tophaceous gout (Figure 15)
- Normal mineralization
- Normal joint space
- Eccentric erosions with sclerotic borders
- Overhanging edges bones
- Tophi: usually asymmetric soft tissue masses around the joint.Tophi may also locate intraosseous,
intraarticular or around enthesis or extensor tendons (quadriceps,
triceps,
Achilles tendon)

Fig. 15: Radiologic findings of chronic tophaceous gout
a. Radiograph (detail view) of the foot shows erosion with sclerotic rim in the 1st MTF
b. Radiograph (detail view) of the hand shows overhanging edges bones
c. Radiograph (detail view) of the elbow shows a calcified tophus
3.2 CALCIUM PYROPHOSPHATE DIHYDRATE (CPPD) CRYSTAL DEPOSITION DISEASE
- It is the most common crystal deposition disease.
It is characterized by acute,
subacute or chronic joint inflammation with deposition of CPPD crystal in hyaline cartilage,
fibrocartilage and other soft tissue structures.
- It affects middle-aged and elderly people.
- The clinical presentation is highly variable.
Indeed the disease has been called a “great mimicker” of other arthritides.
- It is frequently presented as a form of arthritis that simulates osteoarthritis with an acute inflammatory component.
It most common affects knee and hand (MCP) joints.
- Typical radiologic findings: (figure 16)
- Chondrocalcinosis (knee,
symphysis pubis,
wrist)
- Normal mineralization
- Joint space uniform narrowing
- Subchondral cysts are one of the hallmarks of this arthritis.
They are usually larger and more numerous than in osteoarthritis
- Osteophytes are common but less frequent than in osteoarthritis.
4.
CONNECTIVE TISSUE ARTHROPATHIES
4.1.
SCLERODERMA
- It is a multisystemic disease characterized by dermal or internal fibrosis (localized and generalized forms)
- Affects young women.
Age: 30-40 years old.
- Most frequent: CREST Syndrome
- Typical radiologic findings (figure 17)
- It usually causes no articular erosions
- Acroosteolysis (distal phalanges of the hand)
- Subcutaneous and periarticular calcification
- Distal fingers soft tissue atrophy
4.2.
DERMATOMYOSITIS
- Soft tissue calcification in upper and lower extremities proximal musculature.
- Usually no articular erosions
- Juxtaarticular osteoporosis
5.
ARTHROPATHIES COMPLICATIONS
- Arthropathies progression and complications due to pharmacological treatments side effects (corticoid,
nonsteroidal antiinflammatories,
immunosuppressives,
and biologic therapies) are assessed with computed tomography (CT) and MRI.
- We describe complications,
on one hand because of the immunosuppression therapy,
and on the other hand due to osteoporosis,
either because of the disease or as a secondary pharmacological effect that facilitates the appearance of fractures.
We show the most outstanding cases.
CASE 1.
Osteomyelitis in a patient with RA.
A 72-year-old man with RA.
He had been treated with leflunomide.
In the right foot sole he suffered ulceration with swelling and erythema.
Radiograph of the foot (figure 20) and MRI are requested to complete the study (figures 21,
22 and 23)

Fig. 21: Right foot MRI. Sagittal unenhanced fast spin-echo T1 weighted image (fig 21) shows a hypointense lesion in the distal half of the 5th metatarsal bone marrow. This lesion is bright in short tau inversion recovery (Stir) (fig 22), and shows peripheral enhancement after contrast administration (fig 23) . It is consistent with osteomyelitis and intraosseous abscess. A plantar ulcer with inflammatory changes in the subcutaneous cellular tissue is shown.

Fig. 22

Fig. 23
CASE 2.
Vertebral fractures in a patient with ankylosing spondylitis.
A 65 year-old-patient with ankylosing spondylitis.
He had intense dorsolumbar pain after a traumatism.
Figures 24 and 25. Spine MRI

Fig. 24: Spine MRI.Lower half T9 and upper half T10 vertebral bodies bone marrow shows low signal intensity in unenhanced fast spin-echo T1-weighted image (fig 24) and increased signal on fat-saturation fast spin-echo T2-weighted image (fig 25) relative to trabecular fractures and bone bruises. A fracture line is seen on the right lamina of T9 (fig 24).An interspinous ligament tear with liquid, bright in T2-weighted image(fig 25)

Fig. 25
Figure 26.
Spine MRI (sidebar)
CASE 3
Right hip avascular necrosis in a patient with RA
A 41 year-old- women with RA treated with corticoids and methotrexate.
She began suffering pain at the right hip several months ago.

Fig. 27: Radiograph of the pelvis shows asymmetrical joint space narrowing at the right hip. The left hip appears normal.
The study was completed with a pelvis MRI (figures 28 to 31)
CASE 4
Trabecular fracture of the tibia in a patient with psoriatic arthritis
A 67 year-old-woman with Psoriatic arthritis treated with leflunomide and methotrexate.
She had pain at the left ankle without previous trauma.
Fig.
32.
Left ankle MRI
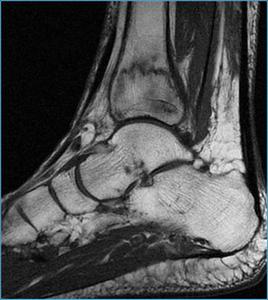
Fig. 32: Left ankle MRI. Sagittal unenhanced fast spin-echo T1-weighted image shows multiple irregular hypointense lines in the lower third of the tibia relative to trabecular fractures.

Fig. 33: Left ankle MRI. Sagittal Stir image shows a diffuse area of signal increased relative to bone bruise
CASE 5
Severe osteoporosis complicated with vertebral fractures in a patient with RA.
A 76 year-old-woman with RA. She had received multiple treatments (gold salts,
leflunomide,
infliximab).
She was in treatment with corticoids and methotrexate.
She had acute dorsolumbalgia after a traumatism.
Figure 34 and 35.
Spine MRI

Fig. 34: Spine MRI.Sagittal unenhanced fast spin-echo T1-weighted (fig 34) image shows severe fracture of the T8 vertebral body with bone marrow edema (fig 35) and a trabecular fracture line of the T9 vertebral body. T8 vertebral body shows a slight displacement of the posterior wall that decreases the anterior subarachnoid space.

Fig. 35




































