Type:
Educational Exhibit
Keywords:
CNS, MR, MR-Diffusion/Perfusion, MR-Spectroscopy, Radiation therapy / Oncology, Biological effects
Authors:
V. Vukovic, J. Mihailovic, M. Gajic Dobrosavljevic, J. STEVANOVIC; Belgrade/RS
DOI:
10.1594/ecr2013/C-1063
Background
A total of 37 patients,
24 male and 13 female,
mean age about 51±18 years,
were evaluated from July 2011 to December 2012.
We used RANO criteria to compare radiological signs prior to three weeks after RT/HT,
then our patients were followed up every two months.
Early radiological progression (ERP) was defined as the qualitative interpretation of radiological progression based on abnormal post contrast enhancement on T1-Weighted Images (T1W) and T2- Weighted Images (T2W),
Fluid Attenuated Inversion Recovery (FLAIR) non enhancement,
non target lesions.
Advanced MRI techniques were used in study,
Diffusion Weighted Images (DWI),
Perfusion Weighted Images (PWI),
Magnetic Resonance Spectroscopy (MRS),
in order to improve radiological conclusions.
Based on RANO criteria respond of patients could be classified like complete remission (CR),
partial response (PR),
stable disease (SD) or progression disease (PD).
CR and PR which is not confirmed within for weeks was perceived like SD.
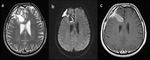
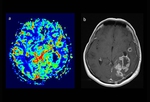
It was noticed that early radiological progression which correlate with clinical deterioration could be recognize like progression disease witch has to be confirmed in ≥12 weeks to exclude pseudoprogression . Fig. 1 presents the first postoperative scans of 58 year old male patient with confirmed GBM located deep in frontal white matter with obvious corpus callosal extension on the right side,
after maximal surgical resection.
On Fig 1a there is restricted diffusion within postoperative injury.
On Fig 1b and 1c we have clearly demarcated postoperative changes on T2W and T1W postcontrast scan.
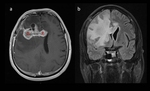
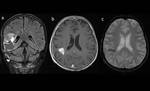
After completion HT-RT we observed signs of early radiological progression with extension T2W/FLAIR elevated SI,
mass effect and defined target lesions on T1W/postcontrast axial scans Fig. 2 (a,
b,c).
PWI was elevated in target lesions.
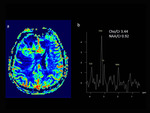
MR multi voxel spectroscopy wich was done with TE135ms and included postcontrast target lesions showed elevatation ratio Cho/Cr with decreased NAA Fig. 3 ( a and b).
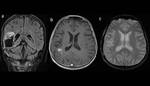
Our other patient who is undergone surgical tumor reduction,
especially because of multifocality was 59 years old male .On postoperative scan,
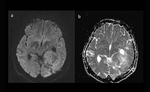
prior RT-HT we want to indicate significance role of DWI and ADC which can give us possibility to differentiate tumor rest and postoperative injury.
We can notice lower ADC value which origin of tumor hypercelularity than in surgical resection Fig. 4 (a and b).
PWI was elevated in DWI suspected regions of tumor rest ,
while after contrast administration we have signs of multifocality around postoperative cavum Fig. 5 (a and b).
We can use it to differentiate postterapy tumor necrosis.
Among pseudoprogressors we demonstrated 61 years old female who was undergone maximall surgical resection.
The first postterapy scans demonstrated focal lesion FLAR and postcontrast increasing SI Fig. 6 (a ,b,c) wich was recognized like progression desease with suspicious hemorrhage in tumor progression.
Patient was without clinical deterioration.On the follow up after 12 weeks we had discreate regression of findings Fig. 7 (a and b).