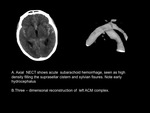
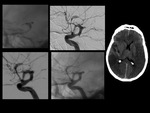
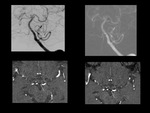
Patient Characteristics:
A total of 23 patients were included (12 female and 11 male).
Hunt and Hess grade was I in 3 cases (75.0%),II in 14 cases (12.5%),
III in 1 cases (8.3%),
and IV - V in 5 patient (4.2%).
Aneurysm Locations:
Anterior circulation 20/23 (83%)
Anterior Communicating artery 14/20 (70%)
Carotid Artery 2/20
Bifurcation MCA 1/20
Coroidea.
3/20
Posterior Circulation: 3/23 (13%)
Posterior inferior cerebellar 3/3
Assisted techniques:
Nineteen (83%) were treated with assistance of assisted techniques: remodeling balloon.
Anatomic results,
Montreal scale:
Seventeen (65%) aneurysms were completely or nearly completed occluded and 4 (17%) were incompletely occluded.
Four of the aneurysms were failed occluded.
Intraprocedural Complications:
Intraprocedural Rupture: 4/23 (17%). Two of them didn’t change your clinical state and they had a mRS score of 2 at six month.
The other two worsened clinically and they had high disability (mRS >3).
Thromboembolism 2/23 (8,6%).
Intra – arterial thrombolytic using was successfully performed and the two patients had no permanent neurologic deficits.
Rebleeding:
There was 1 case of early postoperative hemorrhage in an aneurysm that originally was presented as ruptured.
This aneurysm was coiled but the occlusion was incomplete and had an intraprocedural rupture.
The patient had a bad clinical outcome (mRS 4).
Clinical Outcome:
mRS score was 0 (no symptoms) in 13 patients,
two patients had a mRS score of 1 and two patients had a mRS of 2.
So 17 patients (74%) were independent at six month.
Two patients died (mRS 6) and none of them had procedural complications.
Discussion:
The distribution of the sample is similar to large studies published in the literature,
including the ISAT study and meta-analysis of Brinjikji.
In our study the most frequent location was the anterior communicating artery and Brinjikji meta-analysis of the most common is the internal carotid.
With this distribution we believe that our sample is directly comparable with these two studies.
A significant difference in our sample compared to other studies is the use of balloon remodeling which is used in most cases.
The percentage of complications,
thromboembolic and intraoperative rupture,
are higher than in the series include larger aneurysms.
These findings are similar to those shown by Brinjikji in their meta-analysis.
Therefore it can be deduced that endovascular treatment of aneurysms less than 3 mm are associated with a higher rate of procedure complications.
The prognosis of patients is similar to the series that include larger aneurysms,
so it means that the technical complications not significantly influence the prognosis of patients.
This is because proper management of thromboembolic complications with the use of antiplatelet,
anticoagulants and mechanical thrombectomy by angioplasty with remodeling balloon.
The same applies to the aneurysm rupture; the remodeling balloon closes the neck of the aneurysm and maintains stable microcatheter to complete the closure of the aneurysm.
Our study has many limitations.
The study is retrospective,
nonrandomized and no statistical comparison was made.
The sample is small.
Its conclusions should be confirmed in later studies.