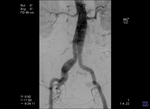
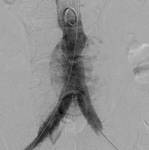
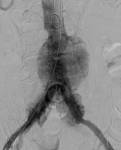
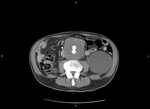
Endovascular Aneurysm Repair (EVAR)
Endovascular aneurysm repair with stent-graft placement is a rising endovascular treatment option for abdominal aorta aneurysms.
It consists on placement of a stent-graft for the "total exclusion" of the aneurysm.
However this total exclusion sometimes fails because of an endoleak of blood flow to the aneurysm lumen,
which is the main cause of complications and failure of the EVAR.
When an endoleak happens,
it causes continued pressurization of the aneurysm sac,
with risk of aneurysm rupture.
Advantages and disadvantages:
The advantages of endovascular repair are lower invasive treatment than open surgery,
lower surgical morbidity and mortality rate,
and reduction of the hospitalization stay after treatment.
The disadvantages (which are likely to reduce over time) are its cost (stent-grafts and their delivery system are very expensive),
the life-long follow-up imaging,
and that the long-term durability of graft material is not yet demonstrated.
Complications and Contraindications:
With the rise of endovascular abdominal aortic aneurysm repair (EVAR),
so have risen its complications,
mainly endoleaks:
- endoleaks
- continued growth of the aneurysm sac without recognizable endoleak
- delayed aneurysm rupture
- graft migration
- branch vessel occlusion (with organic ischemia or infarction)
- infection
- stent-graft structural rupture
- place of puncture complications
Endoleaks
An endoleak is a persistent blood flow out of the endoluminal graft into the aneurysm sac after an endovascular aneurysm repair (EVAR).
Endoleaks are due to incomplete sealing or exclusion of the aneurysm sac,
causing reflux of blood flow into the sac.
Epidemiology and clinical presentation
An endoleak is a common complication of EVAR:
- 30-40% of patients intraoperatively (seen on angiography inmediately after stent deployment)
- 20-40% of patients during the follow-up (even many years after),
so a lifelong imaging surveillance is necessary
Endoleaks are asymptomatic,
however the flow within the aneurysm sac,
if untreated,
may expand it and cause risk of rupture.
Classification
There are several causes of endoleak and can be classified into 5 types as follows:
- type I : leak at graft ends
- type II : aneurysm sac filling via branch vessel (most common)
- type III : leak through a rupture of the graft
- type IV : leak through graft fabric due to graft porosity.
- type V : continued expansion of aneurysm sac without demonstrable leak on imaging
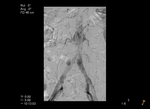
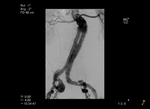
Type I endoleak: due to incomplete or ineffective seal at the proximal (type Ia) Fig. 1 or distal (type Ib) ends Fig. 2 of the graft.
This type of endoleak usually occurs soon after treatment,
but may also occur later.
It happens in 10% of cases,
often because of unsuitable patient or graft selection,
or due to migration of the graft.
They don’t resolve spontaneously.
Type II endoleak: due to retrograde blood flow from branch vessels.
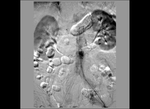
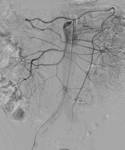
The most frequent branch vessels are lumbar arteries Fig. 5 inferior mesenteric artery (through superior mesenteric artery and Riolano’s arch) Fig. 4 and internal iliac artery Fig. 3
It’s the most common type,
80% of endoleaks.
It has been reported in up to 25% of cases of EVAR
Most spontaneously resolve and require no treatment.
Embolization of branch vessels is required when the aneurism sac expands in size.
Type III endoleak: due to rupture of the graft fabric or separation of the modular components (the graft joints).
This endoleak usually occurs late due to device breakdown.
It may be because of defective device material,
extreme angulation of a segment or improper overlap of the graft joints during insertion.
Type IV endoleak: there is a blood blush through the graft into the aneurysm sac due to its porosity Fig. 6 Fig. 7 while the patient is fully anticoagulated
It resolves spontaneously when coagulation normalizes.
Type V endoleak: continued expansion of the aneurysm sac without demonstrable leak on imaging.
It’s usually referred to as “endotension” and it’s believed to be due to transmission of the pulsation from the graft wall to the aneurysm wall.
Multiple imaging is important to confirm this diagnosis.
Radiographic features and Surveillance
Patients require life-long imaging surveillance to monitor for appearance of endoleaks,
and aneurysm expansion.
Endoleaks are seen as a contrast opacification of the aneurysm sac outside the graft. Monitoring can be made with CT,
MRI or US.
It’s most commonly performed via CTA.
- MRA is an alternative but metallic stents,
in particular stainless steel ones,
cause major susceptibility artifacts that limit its sensitivity.
- Doppler US is limited by the length of the study,
operator dependence,
and sometimes patient’s body habitus.
CT
Different CT techniques have been proposed – single phase CTA,
dual phase CTA,
and triple phase CTA (non contrast,
arterial phase and delayed phase).
The need for non-contrast and delayed phase images may be controversial (particularly because of the cumulative radiation dose the patient will receive over his/her life)
The most appropriate approach for accurate diagnosis and evaluation of endoleaks is a three-phase protocol: non-contrast,
arterial phase and delayed phase: [Stavropoulos SW,
J Vasc Interv Radiol 2005]
- Non-contrast establishes the base density within the thrombosed sac (without this phase,
calcification density could mimic contrast)
- Contrast may be seen as an enlarging focal region of increased density Fig. 9 Fig. 10 or a diffuse increase in the density of the sac (easily seen placing a ROI to measure density) Fig. 8
- Delayed phase is important in order to detect slow endoleaks that do not show in the arterial phase
Treatment
Treatment depends on the type of endoleak:
Type I leaks (above,
below of between graft components) are generally treated as soon as detected.
We can use balloons,
stents or extension cuffs at the leaking graft end to improve the seal.
Embolization with glue or coils has also been described.
[Seehan MK,
Vasc Surg 2004]
Type II leaks (retrograde flow through branch) usually spontaneously thrombose (on 40% of cases).
In most cases they are not treated immediately.
If the leak persists during the watching surveillance,
we must treat it by embolising the branch vessel with glue or coils.
Type III leaks (graft mechanical failure) must be treated immediately,
usually placing additional stent-graft components.
[Teruya TH,
Ann Vasc Surg 2003]
These leaks are believed to be the most dangerous due to quick pressurization of the aneurysm sac.
Type IV leaks (graft porosity) are self-limited and require no treatment.
Type V leaks (endotension) are controversial,
but when continued growth of the aneurysm sack without a visible endoleak is demonstrated,
it is usually necessary to perform an open repair.