Radiological aspects,
that often characterize fibromatoses,
are not discriminative compared to more frequent conditions allocated in the mesentery,
such as mesenteryal cysts,
adenocarcinomas,
lymphomas,
GISTs,
desmoplastic reaction from carcinoids or metastases.
However,
their recognition is essential for proper management.
US and CT are the methods that best provide a diagnostic orientation,
identifying the lesion,
mesenteric origin,
size,
low-grade malignancy and the absence of distant metastases.
The CT iconographic aspect of fibromatosis is directly related to the histology of the lesion,
and in particular to the degree of cellularity and stromal component,
as well as its vascularization.
Lesions with abundant collagenous stroma will be homogeneous,
with soft-tissue attenuation on CT,
while the predominance of myxoid component,
will result in a CT hypoattenuation density.
Blood-supply and so the contrast-enhancement of fibromatosis’ lesions are very variable; more frequently it will be a ‘low-contrast-enhanced’ mass.
On the basis of the degree of aggressiveness,
in our experience,
we ditinguish two patterns of lesions :
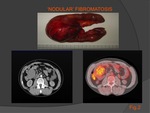
it stands a ‘nodular’ form,
characterized by ‘mass-expansion’ and a diffuse infiltrative one (simple or malignant diffuse mesenteric fibromatosis -the latter more aggressive).
________________________________________
‘NODULAR’ PATTERN:
the lesion appears as a single noncapsulated mass,
characterized by well-defined margins ; it lies on the loops of the small intestine,
which appear not to be infiltrated ,
even if it could be happened microscopically, but compressed by the mass (see Fig.2).
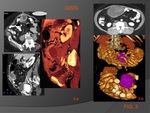
Differential diagnosis – the nodular form can be confused more frequently with GIST lesions (see fig.3); the fibromatosis’ mass generally presents homogeneity,
related to abundant collagenous stroma in the absence of areas of necrosis,
even if a myxoid component ,
less or more conspicuous in the different nodules,
could mimic necrotic area,
making the lesion more heterogeneous; a central myxo-hyaline degenerative core is a CT-pattern more tipical for GISTs.
For both lesions,
mesenteric neighboring appears homogeneous,
with no signs of infiltration.
May be present in GISTs liver metastases and lymph nodes,
absent in fibromatosis.
The contrast administration has not provided discriminative elements in GISTs and fibromatosis,
the contrast enhancement is more or less homogeneous.
It should be noted,
moreover,
that GISTs have submucosal origin (Cajal’s cells) and may have intra,
endo,
eso- or endo-/eso-phytic growth’s pattern respect to the bowel loop of origin or ,
more rarely,
it could be also primitively mesenteric,
without any relationship of contiguity with the loops; instead,
histological element typical of mesenteric fibromatosis are the fibroblastic elements,
which originate from the mesentery and than infiltrate the muscularis propria of the intestinal wall .
The overlap of the radiological aspects,
does not allow,
in the nodular form,
a differential diagnosis with GISTs in all cases; it requires,
in conclusion,
the immunohistochemical examination.
‘DIFFUSE’ PATTERN:
Benign form
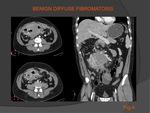
Mesenteric fibromatosis with pattern of diffuse mesenteric mass has simple appearance of intra-abdominal expansive process,
often characterized by considerable size,
which envelops the adjacent structures,
especially the small-bowel loops,
which may appear stenotic,
stretched with irregularities and ulcers of their wall ; sometimes the lumen caliper can be enlarged.
The mass has a density of soft tissue,
the perilesional fat appear ‘nebolous’ (see Fig.
4).
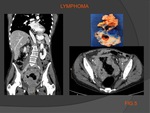
Differential Diagnosis – the benign diffuse pattern can be confused with lymphoma.
In advanced abdominal lymphoma,
the differential diagnosis with fibromatosis can be complicated (see fig.5) : both these entities may present as diffusive mass expansion,
which envelops bowel loops and vascular structures.
Elements suggesting the diagnosis of fibromatosis are the absence of lymphadenopathy and the non-involvement in the pathological process of other abdominal organs such as the liver and spleen,
instead present in lymphoma; lymphoma rarely presents with occlusion.
Finally,
the diagnosis of diffuse mesenteric fibromatosis should be always considered in presence of an expansive intra-mesenterial process,
which grows around the bowel loops,
in the absence of lymphadenopathy and hepatosplenomegaly,
especially in patients with clinical history of previous abdominal surgery and FAPS.
-------------
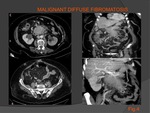
Malignant (or aggressive) form
Morphological features of mesenteric fibromatosis,
diffuse malignant form,
are similar to the previous one,
but with more rapid growth of the lesion,
a greater tendency to recur after surgery and an higher rate of perforation or abdominal obstruction,
that complicate fibromatosis (see Fig.6).
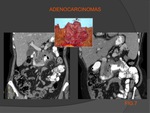
Differential diagnosis – the malignant diffuse pattern can be confused with adenocarcinoma (see fig.7),
when this one is in an advanced stage (with abundant trans-mural and exophytic growth).
These two pathological entities are different for their origin: adenocarcinoma arises from the mucosa and only later invades the intestinal wall,
and then the mesenteric fat,
while in fibromatosis,
the process is exclusively extra-intestinal,secondary there is the invasion of muscolaris propria tunica and the ulceration of the mucosa,
due to ischemic insults.
There is also a different extension of the pathological processes: fibromatosis is,
in general,
more widespread,
compared to adenocarcinoma.
The latter is also richly vascularized with intense contrast enhancement,
while the fibromatosis is less vascularized and presents a more heterogeneous contrast enhancement.
Adenocarcinoma presents often metastatic lymphadenopathies ,
generally absent in fibromatosis.