Crohn´s disease is a multifactorial disease where different etiologic elements: genetic,
enviroment,
lifestyle,
food etc generate in the early beginning a segmental affectation of the mucosa consisting in aphthous ulcers alternating with normal mucosa.
The evolution of the disease can stand there or progress to merge those mucosal lesions as well as to extend keeping a transmural and extramural way.
1.
Active Inflamation.
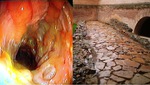
The typical features in active inflamation are edematous mucosa and ulcers giving an appareance called "cobble stone".
(Fig 5)
The proccess afects to mucosa with a neutrofilic infiltrate generating the apthous ulcers wich can fissure the mucosa and progress to the rest of the layers of the bowel generating submucosal edema and inflammatory changes in serosa.
From the radiological point of view,
radiologists must evaluate in this stage:
A. Wall thickness.
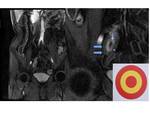
There will be enchacement of mucosa and serosa resembling the typical appareance in "target" (Fig 6). This feature can be evaluated in CT and MRI with more accuracy.
Barium procedures only will show the luminal narrowing during the transit of the oral contrast ("rope sign").
(Fig 7 and Fig 8)
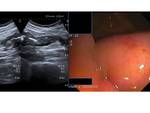
Ultrasound can show also the terminal ileum thickness but sometimes miss thickness in other segments of the bowel or doesn´t depict neither mesenteric changes nor asociated complications in all its extension.
(Fig 9)
Diffusion sequences in MRI can be very useful to depict mural inflamation viewed as a increased signal intensity.
The absence of increased signal in this sequence is very suggestive of not active inflamation.
B.
Increased vascularity/engorgement of vessels.
The involvement of all bowel layers with inflammatory changes generates an increased blood flow in the affected zone that can be evaluated by radiologist as an increase in size and number of vascular branches resembling a comb (the "comb" sign).
(Fig 10 and Fig 11).
Those vessels will be surrounding the affected segments of the bowel.
C.
Lymphadenopaty.
(Fig 10)
It is possible to asses number and distribution of lymph nodes in mesentery. Neither barium procedures nor ultrasound will be able to offer a proper of view of the mesentery and the lymh nodes affected so MRI and CT are the most appropiated techniques.
In our experience we mainly use Coronal views in MRI to this purpose (Coronal FIESTA and Coronal LAVA Post-gadolinium sequence).
D.
Edema/stranding in mesenteric fat.
Mesenteric fat have to be reviewed in order to depict posibility of flemonous areas or incipient abscesses wich would change the status of the disease adding a complicated event.
E.
Motility,
adhesions and dilatation.
With MRI cine sequences it is possible to asses how is the behaviour of the different parts of the bowel in an acute or cronic event of the disease.
We cover the entire abdominal cavity in coronal view displaying the different acquisitions like a movie (Fig 13) in wich the intestinal transit can be easily evaluated giving us a very important information.
It is pretty important the patient has a good distention of the bowel.
In cases of wall thickening and stenosis it can be evaluated the increase in the movement of the small bowell as well as dilatation.
(Fig 13)
2.
Complicated features.
The transmural inflammation may progress generating an extraintestinal extension of the disease creating fistulous tracts that will extend towards the abdominal cavity leading to abscess formation and/or interconnection between bowel loops.
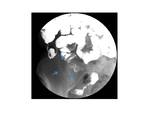
This interconnection usually takes a stellated appearance (Fig 12),
with traction of loops and anfractuous development, being very difficult to erradicate with medical therapy.
3.
Cronic changes.
After acute inflammation and over time and medical therapy the disease progress to fibrotic changes within the different layers of the bowel.
Fibrotic changes will never respond to medical therapy and its main complication is the creation of strictures and stenosis that may progress to bowel obstruction.
Those features will require surgical treatment.
(Fig 14)