Ring Enhancing Lesions:
May be single or multiple ,unilocularor multilocular
Causes:
- Bacterial- Tuberculoma ,Pyogenic abscess
- Fungal- Histoplasmosis,
Aspergilosis,
Nocardiosis,
Mucormycosis
- Parasitic- Neurcysticersosis,toxoplasmosis,Amebic abscess ,Echinococcosis
- Neoplastic- Primary brain tumors,
Metastasis Primary CNS Lymphoma in AIDS
- Demyelination - Multiple sclerosis ,Tumefactive demyelination
- Others - Subacute infarct,Resolving hematoma,
Cavernous hemangioma ,Radiation necrosis. Aneurysm wit central hthrombus,
post operative ,ADEM,
Sarcoidosis
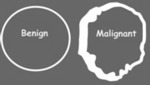
- Pattern of contrast enhancement: Fig.1,2.
-
- Benign:
- Round and convex
- Smooth ,uniform
- Thin(<20mm)
- Malignant:
- Undulating
- Irregular,variable
- Thick(>20mm
Intracranial tuberculoma can occur with or without tuberculous
meningitis.
Multiple tuberculomas are common with miliary
pulmonary tuberculosis.The enhancing lesions usually ranges
from 1 mm to 2 cm.
CT :
°Hypodense to hyperdense round or lobulated nodule/mass
with moderate to marked edema
° Ca++ uncommon (approximately 20%)
°TBM :Isodense to hyperdense basal exudate effaces CSF
spaces,
fills basal cisterns,
sulc
°CECT
°Tuberculoma: Solid or ring-enhancingT
°"Target sign": Central Ca++ or enhancement
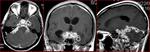
° TBM : Prominent leptomeningeal and basal cistern
enhancement (fig.4)
° Ependymitis: linear periventricular enhancement
° Ventricular dilatation due to hydrocephalus may be seen
° Often,
low-attenuating focal infarcts in the deep gray
matter nuclei,
deep white matter,
and pons; these resul
from associated vasculitis.
MRI:
°Non-caseating tuberculoma : Hyperintense on T2
and slightly hypointense on T1-weighted images
°Caseating tuberculoma: Iso- to hypointense on both T1and
T2-weighted images,
with an iso- to hyperintense rim on
T2-weighted images.
°CEMR: Nodular or ring-like enhancing lesions
°Magnetization transfer MRI : A higher number of
tuberculomas is seen on the magnetization transfer
magnetic resonance images compared with routine spin
echo images.
Magnetization transfer MRI has also been
found to be effective in the reliable differentiation of
tuberculomas from cysticercosis
- Neurocysticercosis :Fig.5,6.
-
Caused by the larva of Taenia solium, is the most common parasitic infection of the central nervous system.
The lesion can be located anywhere within the CNS,
though the parenchymal corticomedullary junction is the most common site in the brain.
Imaging reveals the four distinct stages of neurocysticercosis which are pathognomonic.
Usually,
the lesions are <20 mm in diameter.
Calcified eccentric scolex is often seen in a cysticercal lesion.
The lesions are often multiple and most often do not have extensive edema.
CT:
- Vesicular stage (viable larva): Cystic lesion with a central hyperdense "dot" (nodule),
representing the scolex . No edema or enhancement
- Colloidal vesicular stage (degenerating larva):Degenerating larva induces edema .Hyperdense cyst with thicker ring-enhancing fibrous capsule
- Granular nodular (healing) stage: Mild edema As the lesion heals,
it becomes isodense or mildly hyperdense with a calcified scolex Involuting enhancing nodule and edema are both characteristic.
- Nodular calcified stage: The final stage.
Shrunken,
calcified nodule without edema or enhancement
- Subarachnoid lesions: Multiple isodense cysts without scolex,
may cause meningitis
- Intraventricular cysts: not well seen on CT,
may see hydrocephalus
MRI:
- Vesicular stage: Cystic lesion isointense to CSF on T1 T2 and FLAIR.
May show discrete,
eccentric hyperintense scolex No surrounding edema
- Colloidal vesicular stage: Cyst is mildly hyperintense to CSF on T1,T2 and FLAIR (useful to detect intraventricular cysts)
- Surrounding edema,
mild to marked
- Granular nodular stage: Thickened,
retracted cyst wall; edema decreases
- Nodular calcified stage: Shrunken,hypodense Ca++ lesion
- T1 and FLAIR useful to detect intraventricular cyst
- T2* GRE: Useful to demonstrate calcified scolex
- DWI: Cystic lesion typically isointense to CSF
CMR
- Vesicular stage: No enhancement typical,
May see discrete,
eccentric scolex enhancement
- Colloidal vesicular stage: Thick peripheral enhancement with enhancing marginal nodule (scolex)
- Granular nodular stage: May have nodular or ring-enhancement
- Nodular calcified stage: Small calcified lesion,
rare minimal enhancement
- Intraventricular cysts may cause ventriculitis and/or hydrocephalus.
- Abscess:Fig.7
- Most abscesses occur in the supratentorial region in the frontal or parietal lobes at the gray-white interface.Up to 14% occur infratentorially.
Brain abscess has:
-
- Thin uniform wall (2‐7mm),
- Smooth inner and outer margins
- Convex all around
- Homogeneous center
- Rim of surrounding Edema
MRI:
- Capsule is isointense or hyperintense to white matter on T1 and hypointense on T2
- Area of Central Necrosis- Low signal on T1,high signal on FLAIR and T2 (low density on CT)
- Restricted Diffusion
- MRS :Central necrotic area shows,
alanine ,succinate and acetate peaks
- Contrast‐enhanced CT and MR:
- Well defined rim of enhancing capsule with low density/intensity center
- Necrotic Tumor vs.
Pyogenic Abscess: Differentiation by DWI and ADC
- Necrotic Tumor: Decreased signal intensity on DWI.
Increased signal intensity on ADC maps
- Pyogenic Abscess :Increased signal intensity on DW I Markedly decreased signal intensity on ADC maps
•Glioma: Fig.8
- Most of the tumors are large in size,
are often located deep in the white matter. Primary brain tumors frequently cross the midline.
- CT or MRI: Expansile mass with central necrosis
- Large surrounding vasogenic edema
- CT :
- Typically heterogeneous
- Calcification,
occasionally
- MRI:
- Tumor Nidus,
hypointense on T1 and hyperintense on T2
- T1 hyperintensity,
if hemorrhage is present
- CE CT / MR :Ring enhancement
- Multilocular ring patterns.
- Large enhancing cystic wall with a brightly enhancing mural nodule (Pilocytic astrocytoma)
-
Metastasis: Metastatic lesions are single or multiple,
typically subcortical,
occurring in or near the gray matter-white matter junction,
and are usually associated with severe perilesional edema.
- CT
- Iso to hypodense,Hyperdense if hemorrhagic
- Intense nodular or ring enhancement
- MRI
- T1:
- Typically iso to hypointense
- Hyperintense -Hemorrhagic metastases and Melanoma have intrinsic high signal
- Enhancement - Punctate,
or ring-enhancing,usually intense. Delayed sequences may show additional lesions,
CE MR is the current standard for small metastases detection.
- T2 and FLAIR
- Typically hyperintense
•Ganglioglioma: Fig.10.
- Partially cystic,
enhancing,
cortically-based mass in child/young adult with temporal lobe epilepsy
- Location -Most commonly,
temporal lobe
- Typically 2-3 cm in adults,
Larger 4 -6 cm in children
- Calcifcation (35-50%)
- CT: Variable density
- 40% hypodense,
30% mixed hypodense (cyst),
isodense (nodule)
- 15% isodense or hyperdense
- CECT
- Approximately 50% enhance
- Varies,
rim or nodular
- MRI:
- TIWI-Hypointense to isointense to gray matter
- May see associated cortical dysplasia
- T2WI- Hyperintense mass typical
- 2* GRE: May show Ca++ as areas of "blooming"
- Contrast CT/MR-
- Variable enhancement,nodular or ring-like
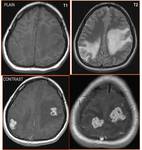
•Demyelinating disorders:Fig.11,12
- Hypodense on CT
- Multiple enhancing ring lesions are encountered in several active demyelinating disorders.
- Open or incomplete ring enhancement.
Rim is hypointense on T1.
Fig 11.
- No mass effect
- Little or no vasogenic edema
- Tumefactive demyelinating lesions are large (usually 2 cm) Fig 12.
- Vessel-like structures running through the center of lesions on dynamic T2*
•Resolving hematoma: Fig.13
- CT-Hypo/Hyperdense with mild edema and mass effect
- MRI-Deoxy-Hb:Isointense on T1 and hypointense on T2
- Extracellular methemoglobin (subacute) : Bright on T1- and T2
- Hypointense foci "bloom" of T2*GRE
- CECT/MRI Uniform rim of enhancement