Unenhanced-MRA was performed in 24 patients (14 men; mean [±SD] age,
54 ± 17 years) with clinical suspicion of main renal artery disease.
Two radiologists independently evaluated the ability of U-MRA for depiction of the renal arteries and detection of the main renal artery disease by comparing the results with the gold standard tests: CE-MRA (14 patients) and Digital Subtraction Arteriography (DSA) (8 patients).
All examinations were performed with a 1.5 T GE Hdxt MR system.
Unenhanced-MRA was perform using a respiratory-triggered 3D fat saturated fast imaging employing steady state adquisition (FIESTA) with inversion recovery pulses (Inhance 3D inflow IR [GE]).
Inhance 3D inflow IR is an unenhanced-MRA sequence based on the inherent in-flow effects of blood.
A selective inversion recovery RF pulse is applied to invert all the spins in the specific region.
As soon as the longitudinal magnetization recovers to the null point,
FIESTA is used for signal acquisition.
The stationary background signal and the slow flow venous blood signal are suppressed by this inversion recovery (IR) RF pulse.
The arteries generate a significantly bright signal due to the in-flow effects of the fresh blood (4,13).
An eight-channel phased-array body coil was used for signal reception.
First,
the patient underwent MRI feet first with the arms above the head.
Respiratory trigger is used to reduce motion artifacts and SPECIAL (a chemical saturation technique) is implemented to obtain good fat saturation.
Parallel imaging (array spatial sensitivity encoding technique [ASSET]) was used in the in-plane phase encode direction.
The MR parameters are shown in Table 1.
The CE-MRA sequence was a 3D fast spoiled gradient echo (FSPGR).
Automatic triggering (Smart prep) was used to start MR data acquisition when the contrast agent reached an optimal concentration in the renal arteries,
detected by positioning a “tracker” in the aorta just superior to the renal arteries.
The maximum monitoring period was 40 s.
Suspension of respiration was required during MR data acquisition.
Parallel imaging (ASSET) was used in the in-plane phase encode direction with an acceleration factor of 2.
The MR imaging parameters are presented in Table 2.
Gadobutrol 10 ml (GADOVIST 1.0,
BAYER,
Berkshire,
UK) was injected at 2 ml/s,
followed by 20 ml normal saline while Smart Prep monitored the change of signal that determines the time of arrival of contrast medium.
Intraarterial DSA was performed with a flat panel DSA system.
Angiography was performed by an interventional radiologist through the right femoral arterial route with a 5F pigtail catheter and injection of 30 mL of iodinated contrast medium at a flow rate of 15mL/sec.
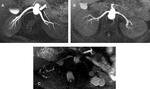
The MR image quality of the renal arteries was graded as follows (Fig.1):
- Excellent: Homogenous vessel signal intensity without flow artifacts,
sharp and complete delineation of vessel borders and less interference from venous system.
- Good: Homogeneous vessel signal intensity with slight flow artifacts,
good delineation of vessel borders,
including the main renal artery and segmental branches up to the renal parenchyma.
- Poor: Inhomogeneous vessel signal intensity and irregular delineation of vessel borders and unclear depiction of the main renal artery.
- Not assessable: Vessels not visible or diagnostic information cannot be obtained because of severe blurring artifacts.
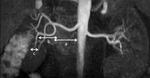
The following segments were evaluated: main renal artery,
first order segmental branches and secondary order arteries within the renal parenchyma (Fig.
2).
The presence of renal artery disease and the ability to depict main renal artery stenosis were recorded.
The degree of stenosis was classified as hemodynamically non-significant (<50%),
and stenosis hemodynamically significant (>50 %).
After the independent reviews,
a consensus reading was performed to resolve discrepancies.
These consensus data were used as the reference for the Unenhanced-MRA reading.