This pictorial review illustrates the imaging findings of multiple cases of peritoneal disease of our Department.
Lymphangioma
Cystic linfangioma is considered to be a benign cystic tumor due to a congenital malformation of the lymphatic system.
90% occur in the neck and axila while 5% are reported to occur in the mesentery,
abdominal viscera,
retroperitoneum,
lung and mediastinum (5).
However,
they are the most common tumors of the mesentery.
At CT cystic lymphagioma typically appears as a thin walled,
multiloculated cystic mass,
with attenuating values that range from that of fluid to of fat (2).
Both cystic and septa can show enhancement after contrast administration.
Calcification is uncommon.
The cystic nature of the tumor can be obscured by cystic walls which can lead to an ill defined opacification of the mesenteric fat.
Surgical excision is the treatment of choice,
since lymphangioma can produce complications such as intestinal obstruction,
volvulus and infarction (5) (fig.
1).
Bile Leak
Bile leaks are the most common complication of laparoscopic cholecystectomy.
Other common etiologies include trauma,
spontaneous perforation of gallbladder/bile ducts and iatrogenic perforation.
CT cannot demonstrate whether a fluid collection contains bile or if it communicates with the biliary tree,
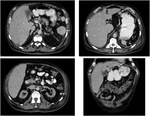
however an encapsulated fluid collection with the same density of water at porta hepatis or at hepatic margin in a patient with previous history of iatrogenic manipulations and trauma is highly suggestive of biloma (6) (fig.2).
Abscess
Intra-abdominal abscesses are localized collections of pus confined to the peritoneal cavity by an inflammatory barrier.
Risk factors include viscus perforation and surgery.
Abscess formation occurs more frequently in the right subphrenic space,
the Morison’s pouch and on the pouch of Douglas (2).
It typically appears as a loculated fluid collection with internal debris,
with fluid-fluid levels and sometimes gas bubbles.
Contrast enhancement may be used to define the cavity wall which usually has irregular thickening (fig.3).
Peritonitis
Acute peritonitis is most often caused by spread of an infection (or other irritants) into sterile peritoneal environment through an organ perforation.
It can have a diffuse extent or it may be a localized process.
Infection of female genital organs (pelvic inflammatory disease) can spread to peritoneum causing the majority of times localized peritonitis.
On contrast enhanced CT images,
acute peritonitis is characterized by ascites,
dilatation of mesenteric vascular structures as well as thickening and enhancement of the peritoneum (fig.4).
Haemorrhage
CT is the modality of choice to detect the presence of an intraperitoneal hematoma,
because of its ability to differentiate between low-attenuation fluid and blood,
which has higher attenuation (30-45 HU).
However blood attenuation depends on the duration,
extent and location of the haemorrhage.
The hyperdense sentinel clot sign is useful in localizing the major site of source of hemoperitoneum.
Active bleeding is diagnosed by extravasated contrast in the arterial phase of contrast enhanced CT study,
characterized by hyperdense foci within areas of lower density liquid blood (7) (fig.5).
Mesothelioma
Peritoneal malignant mesothelioma is a rare aggressive tumor of the peritoneum with a rapid fatal course (median survival 6-12 months) (8).
The majority of all malignant mesotheliomas occur in men with 50-69 years old.
While pleura is the most common site of the disease,
peritoneal mesothelioma accounts for about 6-10% of all mesotheliomas cases diagnosed through the world making it the second most common form (3).
Most people who develop mesothelioma have worked on jobs where they have inhaled asbestos particles (main etiologic factor).
There is a reported association with exposure to simian virus 40 but is controversial (3,8).
Peritoneal malignant mesothelioma must be differentiated from more benign processes such as well-differentiated papillary mesothelioma and multicystic mesothelioma which occur predominantly in women and have no association with asbestos exposure.
In malignant mesothelioma CT may reveal to different patterns: diffuse involvement of peritoneal cavity (characterized by an irregular sheet like thickening of the peritoneum),
or multiple circumscribed peritoneal masses (3).
Both these CT findings show enhancement after IV contrast administration.
Large masses of the great omentum,
separating the colon and the small bowel from the anterior abdominal wall (omental cakes) are usually present.
There is frequently a variable amount of ascites,
thickening of small bowell mesentery as well as thickening of small bowel walls.
In contrast to pleural mesothelioma,
focal calcifications are uncommon.
Unlike lymphomatosis,
peritoneal granulomatous peritonitis and peritoneal carcinomatosis,
lymphadenopathy within the abdomen is uncommon (fig.6).
Carcinomatosis
Peritoneal carcinomatosis is the most common secondary tumor of the peritoneum.
The most common tumors to metastasize to the peritoneal surface are ovarian carcinoma in female and stomach,
pancreas and colon in both sexes.
It is generally associated with loculated haemorrhagic ascites.
The deposition of peritoneal implants depends on the preferential flow of ascites within the peritoneal spaces.
Ascites in a tumor patient should rise suspicion to the presence of peritoneal carcinomatosis.
The CT findings include intravenous contrast material enhancement soft tissue masses/ thickening of the parietal peritoneum.
The neoplastic infiltration of the greater omentum can range from a thickened nodular appearance to large masses that separate the colon and the small bowel from the abdominal wall (omental cakes) (9).
Infiltration of mesenteric fat can produce a stellate pattern mesentery .
This pattern is produced by stiffening and thickening of the mesentery that causes straightening of the mesenteric vessels (4).
Enlarged lymph nodes may be seen.
Both a focal mass or thickening/infiltration of small bowel wall can cause obstruction which is the most common complication of peritoneal carcinomatosis (4) (fig.7).
Sarcomatosis
Peritoneal sarcomatosis is defined as the widespread of a sarcoma in the absence of extra abdominal sites of disease.
It is a rare disease and is more commonly seen in gastrointestinal stromal tumors,
liposarcoma and leiomyosarcoma.
CT imaging findings show are similar to peritoneal carcinomatosis .
However,
peritoneal implants may be hyper vascular and more often spherical and deforming.
They are generally associated with minimal ascites (10) (fig.8).
Splenosis
Splenosis is defined as an implantation of one or more focal deposits of splenic tissue after disruption of the splenic capsule after abdominal trauma or splenectomy.
They can be implanted anywhere in the peritoneal cavity.
At CT they are typically small and multiple nodules with the same attenuation enhancing pattern as a normal spleen.
In contrast to accessory spleens they are acquired ,
not congenital,
and they are not supplied by splenic vessels (11) (fig.9).