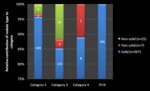
Reference standard
Eighty-one (27.9%) of the 290 CT studies did not contain any nodules.
The reference standard consisted of 599 nodules in the remaining 209 (72.1%) CT studies.
Figure 1 illustrates the frequency of the number of reference standard nodules per scan.
The majority of scans had one (74/209,35.4%),
two (48/209,
23.0%) or three (45/209,
21.5%) nodules.
The median number of reference standard nodules per scan was one,
with a range of 0 to 18 nodules.
567/599 (94.7%) of the reference standard nodules were solid.
260/599 (43.4%) nodules were Category 2,
135/599 (22.5%) were category 3,
and 9/599 (1.5%) were Category 4.
195 nodules were classified as IPLNS (i.e.
34.4% of solid nodules,
and 32.6% of the total number of reference nodules) (Figure 2).
Overall performance of radiographers and radiologists
Radiographers 1,2,3 and 4 had sensitivities of 67.6%,
77.8%,
79.4% and 61.6% respectively (mean sensitivity 71.6 ± 8.5%).
Radiologists A,
B and C had sensitivities of 88.9%,
87.0% and 74.0% (mean sensitivity 83.3 ± 8.1%).
The average FP rate per case for radiographers 1,
2,
3 and 4 were 1.2 ± 2.1,
2.9 ± 2.8,
0.6 ± 1.0 and 1.1 ± 1.3 respectively,
while that of radiologists A,
B and C were 0.5 ± 0.8,
0.7 ± 1.0 and 0.2 ± 0.5 respectively.
Comparison of radiographer and radiologist performance
The sensitivities of each radiographer compared to those of the corresponding radiologists within a particular radiographer-radiologist combination are illustrated in Figures 3-6.
Radiographers 1 and 2 could only be compared with their corresponding local site radiologists (i.e.
radiologists A and B respectively) and the central site radiologist (radiologist C).
Radiographer sensitivity was significantly lower than radiologist sensitivity in 7 of 10 radiographer-radiologist combinations (range of difference,
9.7%-32.8%,
p<0.05),
and not significantly different in 3/10 combinations.
The average FP rates per case for each reader in each radiographer-radiologist combination are illustrated in Table 2.
Radiographers had significantly higher false-positive rates than radiologists in 8/10 combinations (range of difference,
0.4-2.6,
p<0.05),
and there was no significant difference in the remaining two combinations.
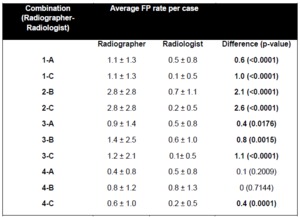
Table 2: Average false-positive detection (FP) rates per case for radiographers and radiologists in each radiographer-radiologist combination.
Reader performance in P1 compared to P2
The two radiographers with the lowest overall sensitivity (Radiographers 1 and 4) showed a significant improvement in sensitivity between P1 and P2 (sensitivity 50.0% in P1 versus 74.1% in P2 for Radiographer 1,
41.8% in P1 versus 67.2% in P2 for Radiographer 4,
p<0.005),
but their sensitivity in P2 still did not reach the level of Radiographers 2 and 3,
who showed no significant difference in their sensitivity between the two periods.
Radiologists’ sensitivity did not significantly differ between the two periods.
No radiographer or radiologist demonstrated a significant difference in their average FP rates per case between the two periods.
As such,
the improved sensitivity of Radiographers 1 and 4 in P2 did not come at the expense of an increased average FP rate.