DISCUSSION:
Introduction
Congenital cystic masses of the neck include thyroglossal duct cysts,
branchial cleft cysts,
cystic hygromas,
dermoid cysts and bronchogenic cysts.
These lesions vary in prevalence from common (thyroglossal duct cysts,
branchial cleft cysts,
and cystic hygromas) to very rare (thymic and cervical bronchogenic cysts).
The clinical history and physical examination of the patient are the most important factors in the evaluation of a congenital neck mass.
An appropriate knowledge of the embryology and anatomy of the cervical region frequently allows the differential diagnosis to be narrowed.
The evaluation of a patient suspected of having a congenital cervical cystic mass should follow an orderly progression.
Because most congenital lesions manifest during infancy and early childhood,
the patient's age provides important diagnostic information.
Congenital cervical cystic lesions are usually slow-growing masses and typically cause symptoms only because of enlargement or infection.
A painless soft or fluctuant cervical mass is the first clinical manifestation in most cases.
Following physical examination,
ultrasonography (US) is usually performed.
US define the size and extent of the mass,
demonstrate its relationship to surrounding normal structures,
and confirm the cystic nature of the lesion.
Computed tomography (CT) also provides this information and is ideally suited for evaluation of soft-tissue planes adjacent to larger masses that cannot be entirely visualized with US.
Moreover,
CT is superior for detecting calcification and,
when contrast material is administered,
the vascularity of lesions.
Magnetic resonance (MR) imaging,
with its multiplanar capability and superior contrast resolution,
demonstrates the full extent of the mass and gives important supplemental information for accurate preoperative planning.
This can be especially relevant in cases of extension into the mediastinum or deep spaces of the neck.
Furthermore,
MR imaging offers superior resolution for evaluating masses located in anatomically complex areas,
such as the floor of the mouth.
THYROGLOSSAL DUCT CYST
Thyroglossal cysts are the most common midline masses in children,
accounting for 70% of all congenital cervical lesions.
They can occur at any age,
and one-third become obvious in adult life.
Embryology
The thyroid gland develops as a diverticulum from the foramen caecum of the tongue,
descending in front of the trachea in company with the thymus and the inferior parathyroid glands.
It reaches its final position by the 7th week of embryonic life.
The hyoid bone develops at about the same time,
from the second and third arches,
and fuses anteriorly so that the thyroglossal duct may pass anterior to,
through or posterior to the body of the hyoid bone.
The duct usually spontaneously obliterates,
but remnants may be found anywhere from the base of the tongue to the pyramidal lobe of the thyroid gland although 80% are juxtaposed to the hyoid bone.
Clinical Characteristics
Most thyroglossal cysts are clinically evident before the child is 10 years old.
Males and females are affected equally.
The cysts present as round masses in the midline of the neck that move up and down with swallowing and with protrusion of the tongue because of their connection to the hyoid bone.
They are soft to firm in consistency,
mobile,
and nontender unless infected.
Pathologic Characteristics
Thyroglossal duct cysts contain a colorless,
viscous secretion.
At histologic examination,
stratified squamous epithelium or ciliated pseudostratified columnar epithelium lining the cyst wall is usually seen.
Mucous glands may also be present.
Ectopic thyroid tissue along the course of the duct is variably reported in up to 62% of cases.
Radiologic Features
On all radiologic images,
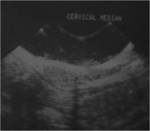
a thyroglossal duct cyst manifests as a cyst like mass either in the midline of the anterior neck at the level of the hyoid bone or within the strap muscles just off the midline.
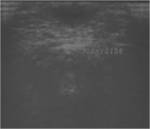
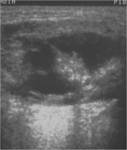
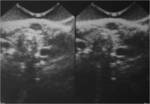
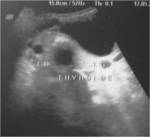
At US,
the finding of an anechoic mass with a thin outer wall in this characteristic location easily establishes the diagnosis of a thyroglossal duct cyst.
However,
this “classic” appearance is seen in less than half (42%) of the cases.
More commonly,
these cysts manifest as hypoechoic masses,
often with increased through-transmission.
They may be either homogeneous or heterogeneous in appearance with variable degrees of fine to coarse internal echoes.
There is no correlation between the sonographic appearance and pathologic evidence of infection and inflammation .
Heterogeneity seen in thyroglossal duct cysts on sonograms is more likely due to the proteinaceous content of the fluid secreted from the cyst wall rather than to infection.
.
Heterogeneity seen in thyroglossal duct cysts on sonograms is more likely due to the proteinaceous content of the fluid secreted from the cyst wall rather than to infection.
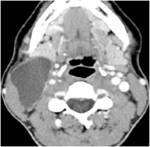
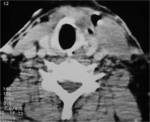
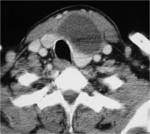
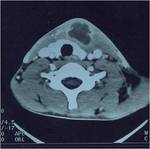
On CT scans,
a thyroglossal duct cyst usually appears as a smooth,
well-circumscribed mass anywhere along the vertical course of the vestigial thyroglossal duct.
The mass has a thin wall and homogeneous attenuation,
the values of which correspond to those of fluid (10–18 HU).
Elevated attenuation values of the fluid cyst reflect its increased protein content and generally correlate with a history of prior infections.
Although thyroglossal duct cysts are usually unilocular,
septations may be seen occasionally.
Peripheral rim enhancement is usually observed on contrast-enhanced scans.
In case of infection or hemorrhage,
a thick irregular rim may be visualized,
and the signal intensity of the fluid becomes variable from the presence of proteinaceous debris
BRANCHIAL CLEFT ANOMALIES
Embryology and Pathology
By the end of the 4th week of embryonic life,
the branchial arches (derived from neural crest cells) and the mesenchyme (derived from the lateral mesoderm) are easily recognizable.
Five pairs of ectodermal clefts (grooves) and five endodermal branchial pouches separate the six arches,
with a closing membrane located at the interface between the pouches and the clefts.
The first branchial cleft normally gives rise to the eustachian tube,
tympanic cavity,
and mastoid antrum and contributes to the formation of the tympanic membrane.
It is the only cleft to contribute to an adult structure,
the external auditory canal.
The second,
third,
and fourth branchial clefts are part of an ectodermally lined depression known as the cervical sinus of His.
As the second and fifth branchial clefts merge with each other,
this cervical sinus is obliterated.
The second branchial pouch,
lined by endoderm,
gives rise to the palatine tonsil and tonsillar fossa.
The third branchial pouch forms the inferior parathyroid gland,
thymus,
and pyriform sinus; the fourth branchial pouch leads to the formation of the superior parathyroid gland and apex of the pyriform sinus.
First Branchial Cleft Cyst
A first branchial cleft cyst,
or parotid lymphoepithelial cyst,
arises along the residual embryologic tract of the first branchial cleft or arch extending from the external auditory canal through the parotid gland to the submandibular triangle.
These cysts account for only 5%–8% of all branchial cleft defects and are most commonly seen in middle-aged women
Clinical Characteristics
Cysts of the first branchial cleft usually manifest as recurrent abscesses or other inflammation either around the ear or at the angle of the mandible.
The patient typically has a history of recurrent parotid abscesses unresponsive to antibiotic therapy and drainage.
Otorrhea commonly occurs if the cyst drains into the external auditory canal.
Occasionally,
a sinus tract extending to the hyoid bone may be seen.
These cystic anomalies often mimic the clinical characteristics of parotid neoplasms and may even be associated with facial nerve palsy.
Radiologic Features
On CT scans,
a first branchial cleft cyst appears as a cystic mass either within,
superficial to,
or deep to the parotid gland.
Cyst wall thickness and enhancement are variable and increase with recurrent infections.
In most cases,
neither the CT nor MR imaging appearance of these cysts is characteristic enough to allow differentiating a first branchial cleft cyst from any other cystic mass of the parotid gland.
As with any lesion of the deep margin of the parotid gland,
a first branchial cleft cyst in this location may extend into the adjacent fat-containing parapharyngeal space.
Second Branchial Cleft Cyst
Clinical Characteristics
Most second branchial cleft cysts are located in the submandibular space.
However,
because of the anatomic relationship of the second branchial apparatus and the cervical sinus,
they can occur anywhere along a line from the oropharyngeal tonsillar fossa to the supraclavicular region of the neck.
These cysts usually appear as painless,
fluctuant masses in the lateral portion of the neck adjacent to the anteromedial border of the sternocleidomastoid muscle at the mandibular angle.
The mass enlarges slowly over time and may become painful and tender if secondarily infected.
In a young patient,
a history of recurrent inflammation in the region of the mandibular angle is highly suggestive of a second branchial cleft cyst.
If a fistula is present,
the ostium is usually noted at birth just above the clavicle in the anterior neck.
Radiologic Features
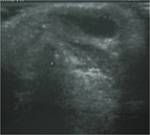
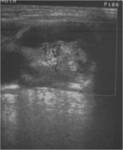
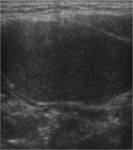
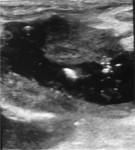
At US,
a second branchial cleft cyst is seen as a sharply marginated,
round to ovoid,
centrally anechoic mass with a thin peripheral wall that displaces the surrounding soft tissues.
The mass is compressible and shows distinct acoustic enhancement.
Occasionally,
fine,
indistinct internal echoes,
representing debris,
may be seen.
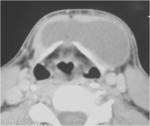
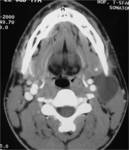
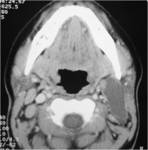
At CT,
these cysts are typically well-circumscribed,
homogeneously hypoattenuated masses surrounded by a uniformly thin wall .
The mural thickness may increase after infection.
The “classic” location of these cysts is at the anteromedial border of the sternocleidomastoid muscle,
lateral to the carotid space,
and at the posterior margin of the submandibular gland.
The cyst typically displaces the sternocleidomastoid muscle posteriorly or posterolaterally,
pushes the vessels of the carotid space medially or posteromedially,
and displaces the submandibular gland anteriorly.
It may also be seen more medially within the parapharyngeal space after extending through the stylomandibular tunnel and middle constrictor muscle.
.
The mural thickness may increase after infection.
The “classic” location of these cysts is at the anteromedial border of the sternocleidomastoid muscle,
lateral to the carotid space,
and at the posterior margin of the submandibular gland.
The cyst typically displaces the sternocleidomastoid muscle posteriorly or posterolaterally,
pushes the vessels of the carotid space medially or posteromedially,
and displaces the submandibular gland anteriorly.
It may also be seen more medially within the parapharyngeal space after extending through the stylomandibular tunnel and middle constrictor muscle.
MR imaging better depicts the deep tissue extent of a second branchial cleft cyst,
which allows accurate preoperative planning.
Third and fourth branchial cleft cysts
Clinical Characteristics.
As with other branchial cleft cysts,
a third branchial cleft cyst usually manifests as a painless,
fluctuant mass in the posterior triangle area of the neck.
Like a cystic hygroma (lymphangioma),
the mass often distends during a viral infection of the upper respiratory tract.
Surgical excision is the recommended therapy of choice for these lesions because of the increased frequency of secondary infection
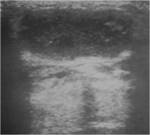
Radiologic Features
A third branchial cleft cyst most commonly appears as a unilocular cystic mass centered in the posterior cervical space on CT and MR images.
As with other branchial cleft cysts,
the cyst fluid may vary in signal intensity on T1-weighted images depending on the protein concentration and is typically hyperintense relative to muscle on T2-weighted images.
Benson et al reported a fourth branchial cleft cyst that connected with the pyriform sinus and appeared similar to an external or mixed laryngocele.
DERMOID CYSTS
Dermoid cysts usually manifest during the 2nd and 3rd decades of life.
There is no gender predilection.
Only 7% of dermoid inclusion cysts occur in the head and neck,
with the lateral eyebrow being the most common location .About 11.5% of dermoid cysts of the head and neck are in the floor of the mouth,
the second most common location.
Clinical Characteristics
The most common clinical appearance of a dermoid cyst in the neck is a midline,
suprahyoid,
slowly growing mass.
Occasionally,
rapid growth may occur secondary to a sudden increase in the amount of desquamation,
pregnancy,
or association with a sinus tract.
The size of the cyst ranges from a few millimeters to 12 cm.
The most common cervical location of a dermoid cyst is the floor of the mouth.
In rare cases,
it may arise within the tongue or from the palate.
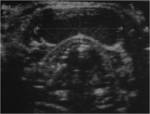
Radiologic Features
Dermoid cysts appear as moderately thin-walled,
unilocular masses,
located in the submandibular or sublingual space.
On CT scans,
the central cavity is usually filled with a homogeneous,
hypoattenuating (0–18 HU) fluid material.
It may appear to be filled with “marbles,” due to the coalescence of fat into small nodules within the fluid matrix.
This “sack-of-marbles” appearance is virtually pathognomonic for a dermoid cyst in this location.
Alternatively,
the cyst may be heterogeneous on CT scans because of the various germinal components.
Fluid-fluid levels with supernatant lipid are possible.
The rim of these cysts often enhances following administration of contrast material.
MR imaging depicts the topographic relationship of these cysts to the mylohyoid muscle in the floor of the mouth and helps determine the surgical approach.
Most dermoid cysts are located superior to the mylohyoid muscle and will be removed with an intraoral approach.
Less commonly,
the lesion is inferior to this muscle and will be removed with an external submandibular approach.
The coronal plane is optimal for determining the location of the mass with respect to this muscle pair.
Dermoid cysts have variable signal intensity on T1-weighted images.
They may be hyperintense (because of the presence of sebaceous lipid) or isointense relative to muscle on T1-weighted images.
They are usually hyperintense on T2-weighted images.
The mass has a clearly demarcated rim but frequently has a heterogeneous internal appearance.