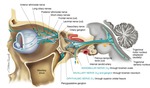
The cranial nerve V originates from a large nucleus in the brainstem and divides into three peripheral branches: ophthalmic,
maxillary and mandibular.
State-of-the-art MRI is the imaging modality of choice for the investigation of trigeminal neuropathy.
Pathological conditions may arise in any of these segments.
A broad spectrum of primary or secondary conditions can affect the trigeminal nerve at specific levels; including ischemic,
inflammatory,
vascular and neoplastic disorders.
Common and uncommon pathologies are reviewed and illustrated with clinical cases and images.
Localizing a lesion to a specific level allows us to narrow the differential diagnosis,
facilitating a therapeutic election.
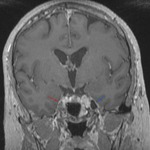
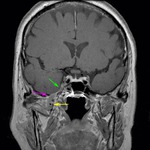
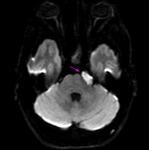
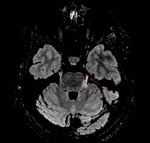
1. NORMAL ANATOMY (Fig.
1)
The trigeminal nerve or fifth cranial nerve is the largest of the nerves emerging from the skull base,
and takes this name by splitting in three branches at the gasserian ganglion: the ophthalmic (V1),
the maxillary (V2) and the mandibular (V3) nerves. Its main role is to provide the sensory input from the face and motor output to the muscles of mastication.
A segmental approach is preferred when describing the distribution of this nerve both in cadaveric dissections and imaging studies.
These segments are: brainstem,
cisternal,
Meckel´s cave,
cavernous sinus,
skull base and extracranial/peripheral branches.
A. Brainstem segment:
Here we find the central component of the trigeminal nerve,
it´s nuclei,
both motor and sensory,
being the latter the largest of the cranial nerves nuclei,
extending from the midbrain caudally to the C2 level of the spinal cord,
where it becomes continuous with the dorsal horn grey matter.
The sensory nucleus has three subnuclei: the mesencephalic,
the pontine and the spinal.
The mesencephalic nucleus is composed by first-order sensory neurons,
carrying propioceptive information of muscles of mastication and mechanoreceptors in gums,
teeth and hard palate.
The pontine nucleus (also called “the chief”) is composed by secondary sensory neurons,
located near the point of entrance of the nerve,
carries mainly discriminative touch sensation from the face.
The spinal nucleus is concerned both in tactile and thermalgesic signals.
The small motor nucleus (or masticatory nucleus) is located in the midpons,
medial and anterior to the sensory nucleus,
supplying innervation to the muscles of the first branchial arch.
B. Cisternal segment:
The trigeminal nerve emerges from the lateral pons at its equator as two trunks,
a bigger sensory root and a smaller motor root,
placed slightly antero-medial to the former.
The nerve travels in an anterior-lateral and inferior direction through the prepontine cistern to reach the "porus trigeminus",
a hole in the dura mater placed medially and posterior to the petrous apex,
reaching the Meckel's cave.
C. Meckel´s cave:
The Meckel`s cave,
a dural lined space filled with cerebrospinal fluid,
placed on the trigeminal recess,
a bony depression located at the antero-medial aspect of the petrous bone,
is where the trigeminal ganglion is placed.
This ganglion (also called semilunar or gasserian) contains the sensory neurons soma and divides in its three branches (from medial to lateral): the ophthalmic (V1),
the maxillary (V2) and the mandibular (V3).
The motor root passes below the ganglion and follows the mandibular nerve to reach the masticatory muscles.
D. Cavernous segment:
The first two roots of the trigeminal nerve (V1 and V2) transverse the cavernous sinus from posterior to anterior located lateral to the carotid artery,
inferior to the III and IV cranial nerves and superior to the VI cranial nerve.
E. Skull base:
The three branches of the trigeminal nerve emerge from the cranium through different foramina; the ophthalmic division (V1) reaches the orbit through the superior orbital fissure,
the maxillary nerve (V2) exits the intracranial compartment through the foramen rotundum to reach the pterygopalatine fossa,
and the mandibular nerve (both motor and sensory nerve) traverses through the foramen ovale to reach the infratemporal fossa.
F. Peripheral segment:
V1: The ophthalmic division further divides into three mayor branches when it reaches the orbit: the lacrimal,
the nasocillary and the frontal nerves,
being a subdivision from the latter (the supra-orbital nerve) the terminal branch.
V2: Once in the pterygopalatine fossa,
the maxillary nerve gives off 4 branches: the zygomatic,
pterygopalatine,
meningeal and superior alveolar nerves.
The main root continues anteriorly and enters the infraorbital canal as the infraorbital nerve emerging through the infraorbital foramen.
V3: The mandibular division has both sensory and motor components,
and is the principal branch to carry the sensory input from the lower third of the face and motor output to the muscles of mastication.
The sensory divisions are the buccal,
lingual,
auriculotemporal,
meningeal and inferior alveolar nerve (the terminal branch) that reaches the mental foramen as the mental nerve.
The motor root supplies innervation to the temporal,
masseter,
pterygoid,
mylohyoid and anterior belly of the digastric muscles.
2. MRI TECHNIQUES
A.
T1 Weighted Images:
Traditionally used in the evaluation of anatomy and morphological changes,
but today other sequences have achieved higher spatial resolution.
In areas with plenty of fat,
such as skull base,
fat saturation techniques,
with and without contrast,
allow to differentiate pathological deposits of fat.
3D FSPGR T1 post gadolinium: the administration of contrast agents,
allow detection of pathology with greater contrast in T1 since these substances act by promoting relaxation of the hydrogen nuclei.
The acquisition of volumetric sequences,
allows visualizing the anatomy in the three spatial planes.
Contrast enhanced MR imaging may also be valuable for differentiating between inflammatory and neoplastic process.
Inflammatory process,
such as multiple sclerosis plaques,
enhance transiently and resolve in 1-2 months,
while neoplastic lesions don't.
B.
T2 Weighted Images:
Has classically been utilized for detection of pathology due to the sensitivity in the detection of free water,
which occurs as a manifestation of several pathologic processes prior to alteration in the morphology.
It is often combined with fat saturation to increase sensitivity.
FLAIR (Fluid Attenuated Inversion Recovery): is a T2-weighted sequence,
which removes the signal sequence of cerebrospinal fluid,
but not the signal from pathological lesions which tend to increase its water content or edema.
FLAIR and CUBE sequences are especially useful in suspected multiple sclerosis and other inflammatory processes.
GRE: is a T2 * or magnetic susceptibility sequence,
sensitive to magnetic field inhomogeneities caused by multiple factors,
including degradation products; therefore its use is based on the detection of bleeding and in the evaluation of hemorrhagic lesions,
such as cavernous hemangioma
SSFP (Steady State free precession):
This T2-weighted volumetric sequence,
provides high resolution anatomical images of the cranial nerves,
with high contrast resolution between cerebrospinal fluid and solid structures,
allowing the reconstruction of multiplanar images that highlight the curse of the trigeminal nerves.
This sequence depicts trigeminal cisternal segment in greater detail and can provide important information about the relationship of the nerves to pathologic processes.
Together with the angiographic sequence are especially useful in suspected neurovascular compressions
C.
Angiographic sequences
3D TOF- MRA: it is used routinely to assess the circle of Willis.Gets isotropic voxels allowing steaks and MIP reconstruction in other planes of space without artifacts ladder.It is especially useful in suspected ischemic lesions and,
together with the sequence SSFP,
to study neurovascular conflicts.
D.
Diffusion Weighted Imaging (DWI)
Based on the Brownian movement or diffusion of the particles in tissue.
Ideally the movement is free (free diffusion) and when it is limited,
there is a restriction in the diffusion,
resulting in a hyperintense area on diffusion images.
This sequence is especially useful in posterior and inferior cerebellar artery infarcts (PICA),
which may affect the dorsal trigeminal nucleus.
A restriction in diffusion may also be result of a hypercellular processes such as meningiomas and lymphomas.
Epidermoid cysts,
composed of desquamated cellular debris,
keratin,
lipids and cholesterol,
also generate a restricted diffusion.
DTI (Diffusion Tensor Imaging): based on the same physical concept as DWI (diffusion of hydrogen molecules) can be used to track the nerve fibers direction,
number and relation with pathologic conditions such us neoplastic processes.
(Fig.
2)
3. PATHOLOGICAL CONDITIONS
|
Lesions Involving the Trigeminal Nerve
|
|
A.
Vascular
|
Neurovascular compression,
infarct,
cavernous malformation.
|
|
B.
Neoplastic
|
Primary: schwanomma,
meningioma,
lipoma,
epidermoid cyst,
neurogenic tumors
Other: metastasis,
perineural spread of tumor.
|
|
C.
Inflammatory
|
Multiple sclerosis,
viral (herpes) rhombencephalitis,
neuritis,
Tolosa-Hunt syndrome,
sinusitis.
|
|
D.
Other
|
Syringobulbia,
toxic metabolic conditions,
trauma,
masticator space abscess
|
A wide spectrum of pathological conditions may affect the fifth cranial nerve in its different segments.
Magnetic resonance imagining techniques allows the examination of trigeminal nerve in its full curses: brainstem,
cisternal,
Meckel´s cave,
cavernous sinus,
skull base and extracranial branches.
A.
Vascular:
Vascular affection of trigeminal nerve may arise from brainstem,
cisternal or Meckel`s cave and cavernous sinus segments.
The differential diagnoses of lesions involving the trigeminal nerve are neurovascular compression,
infarct,
arteriovenous malformation and carotid artery aneurysm.
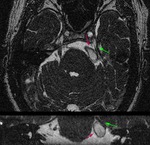
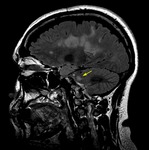
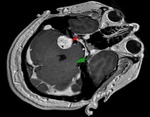
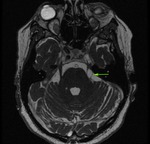
Neurovascular compression is the main cause of trigeminal neuralgia (Fig.
3).
An elongated superior cerebral artery,
and less frequently an elongated anteroinferior cerebellar artery,
vertebrobasilar dolichoectatic and venous compression is found.
B.
Neoplastic:
Neoplastic conditions (primary and other),
may affect the trigeminal nerve.
The common primary tumors are meningioma,
trigeminal schwannoma,
lipoma and epidermoid cyst.
Malignancy can also involve the nerve either with arachnoid seeding or perineural spread.
Meningioma (Fig.
2): is the second more frequent tumor in cerebellar pontine angle and arise from arachnoid cap cell.
In T2 WI sequences,
they show a wide range of possible signals,
with isointense or hypointense signal.
Focal or diffuse parenchymal low signal can be seen if calcified or highly fibrous.
On contrast enhanced images the margins of meningioma are clearly defined with dural-based mass and dural tail centered along posterior petrous wall.
Schwannoma (Fig.
4): the majority of trigeminal schwanomma develop at the gasserian ganglion and the ophthalmic branch,
however they may arise in any segment of the nerve.
A dumbbelled shaped or tubular mass along course of trigeminal nerve is characteristic.
In T1 WI sequences schwannomas show isointense or hypointense signal and hyperintense on T2 WI and variable enhancement.
Large tumors can have heterogeneous signal intensity due to degenerative changes,
including cyst changes and fatty degeneration.
Epidermoid cyst (Fig.
5): is a congenital inclusion of ectodermal epithelial elements during neural tube closure.
The cyst grows by progressive desquamation of epithelial cells and conversion to keratin and cholesterol crystals.
Most have low to intermediate signal intensity on T1 WI sequences,
usually between that of cerebrospinal fluid and brain parenchyma.
On T2 WI they are markedly hyperintense similar to cerebrospinal fluid.
Hyperintensity on DWI sequence makes the diagnosis.
Lipoma: usually located en subarachnoid space.
Is not a true neoplasm.
They arise from a congenital abnormality of the leptomeningeal membranes.
Is isointense to subcutaneous fat on T1 and T2 WI and becomes hypointense with fat saturation.
Malignancies: are associated with extensive and rapidly progressive neurologic symptoms.
Can involve any segment of the nerve but commonly the extracranial branches are compromised.
Perineural tumor spread appears as a focal or segmental thickening (Fig.
6) of branches or abnormal nerve enhance (Fig.
7). T1 WI contrast enhance FAT SAT sequence is the best imagining tool for perineural tumor search.
The differential diagnosis includes other neoplastic conditions,
such primary neural tumor or meningeal carcinomatosis,
and inflammatory disorders such viral neuritis,
meningeal sarcoidosis and hystiocitosis.
Metastatic lesion can rarely affect the trigeminal nerve in any fo its segments (Fig.
8).
C.
Inflammatory (Fig.
9):
Inflammatory conditions can cause trigeminal neuropathy are rare.
Differential diagnoses include multiples sclerosis,
neuritis,
Tolosa-Hunt syndrome and others.
To exclude multiples sclerosis,
a T2 WI of the whole brain must be performed.
Trigeminal neuralgia associated with multiple sclerosis is more often bilateral.
Demyelinating plaques in trigeminal system,
are causally related.
On contrast-enhanced images,
they show a transient nodular or ring shaped contrast during active demyelination.
Other benign inflammatory condition such as herpes rhombencephalitis may also show transient enhancement.
D.
Others:
Other conditions can cause trigeminal neuropathy such syringobulbia; toxic-metabolic conditions related,
trauma or masticator space abscess.
In such cases the examination must be tailored according to clinical suspicion.