Thyroid cancer is the most common endocrine malignancy.
It is classified into well differentiated and undifferentiated carcinomas.
The well differentiated thyroid cancer (DTC) derives from follicular epithelial cells and includes papillary,
follicular,
Hürthle cell and a mixed variety carcinomas.
The undifferentiated thyroid cancer includes medullary carcinoma,
anaplastic cancer,
lymphoma and metastatic tumors.
DTC represents more than 90% of primary thyroid cancers and is best treated with total thyroidectomy (TT) and functional lymph node dissection,
followed by radioactive iodine ablation therapy and performance of a post treatment whole-body scan,
followed by thyroid stimulating hormone (TSH) suppression (L-thyroxine therapy) (1).
Thyroid cancer,
especially DTC,
metastasizes most often to the cervical lymph nodes,
and it is not unusual for occult thyroid cancer lymph node metastases to be present at the time of presentation (2).
However,
prophylactic lymph node dissection for all patients with DTC is controversial.
Thus,
early detection of metastases is of great clinical importance because it enables more successful surgical results and radiation therapy treatment outcomes (3-5).
Ultrasonography is a useful imaging tool for evaluating cervical lymphadenopathy in patients with DTC.
Identifying characteristics of cervical lymph nodes,
using gray-scale and color and power Doppler U/S,
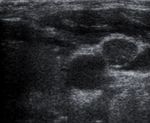
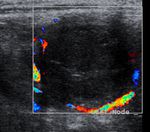
can help to distinguish normal and reactive lymph nodes from potentially metastatic lymph nodes. Round shape ( Fig. 1 ),
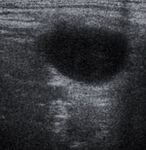
cystic changes ( Fig. 2 ),
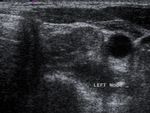
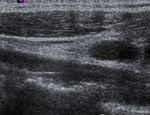
lymph node echogenicity –hypoechogenicity or hyperychogenicity ( Fig. 3 ),
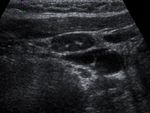
presence of nodal microcalcifications ( Fig. 4 ), peripheral vascularity ( Fig. 5 ) and absence of hilus ( Fig. 6 ) are the most common features in thyroid cancer lymph node metastases.
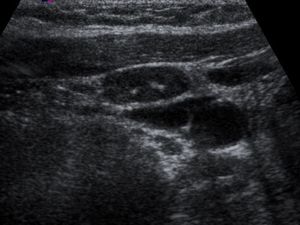
Fig. 4: Gray-scale sonogram of patients with unpalpable metastatic nodes. Image of 23-year-old woman with DTC and associated occult metastatic node in right middle cervical region shows metastatic node that appears hyoechoic with intranodal microcalcifications. These sonographic features are common in metastatic nodes from papillary thyroid carcinoma.
Often,
U/S-guided biopsy is needed to identify a cervical lymph node as being metastasis (6-10).
After initial treatment,
the aim of post-surgical follow-up for DTC is to maintain adequate thyroxine therapy and the early identification of the small proportion of patients who have residual disease or develop a recurrence through the combined use of neck ultrasound (U/S) and serum Tg and (131)I Whole Body Sintigraphy after TSH stimulation.
At the same time,
highly skilled screening neck U/S can identify a few additional patients with subcentimeter,
occult residual,
or recurrent neck lymph node metastases not detected by TSH-Tg (11-13).
The purpose of this study is to determine whether real-time (Rt) ultrasonography-guided (Ug) fine-needle non-aspiration cytology (FNNAC) -Rt-Ug-FNNA- is an effective method for diagnosing non palpable cervical lymphadenopathy in patients with known thyroid malignancy without clinical known recurrent or residual thyroid cancer.