Type:
Educational Exhibit
Keywords:
Ischaemia / Infarction, Dissection, Angioplasty, Perception image, Diagnostic procedure, Catheter arteriography, MR-Angiography, CT-Angiography, Emergency, Vascular, Arteries / Aorta
Authors:
G. P. Abrão, V. E. C. Oliveira, A. A. S. M. D. Santos, M. M. Barbosa, A. S. A. Severo; Niterói- Rio de Janeiro, RJ/BR
DOI:
10.1594/ecr2013/C-1683
Imaging findings OR Procedure details
We describe the main angiographic findings of intracranial arterial dissection,
in the differents imaging methods: computed tomography, CT angiography,
magnetic resonance angiography (MRA) and digital angiography,
with review of clinical and therapeutic aspects.
Computed tomography and CT angiography:
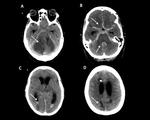
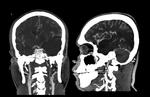
- Computed tomography (CT) without contrast can identify subarachnoid hemorrhage in cases of intramural intradural dissections,
topografar the mass effect resulting from giant pseudoaneurysm and parenchymal ischemic areas affected (Figure 8) 6.
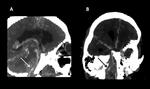
- CT with contrast can show wall mural thickening crescent shaped,
eccentric stenosis of the arterial lumen and enhancement with standard ring by intravenous contrast (Figure 9) 6.
- The multiplanar reconstruction is an important resource that should always be used in the evaluation of DAI as it facilitates the identification of the progressive narrowing of the arterial lumen and pseudoaneurysmatic dissection (Figure 10) 15.
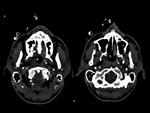
- The computed tomographic angiography (CTA) with multiple detectors shows small residual lumen and pseudoaneurysms that cursem with slow or turbulent flow,
since independent of flow phenomena 15.
- High sensitivity and specificity resulting from the identification of luminal stenosis for eccentric type stenotic artery dissection (Figures 11-12) and increasing the outer diameter for occlusive arterial dissections type.
Thickening of the arterial wall has lower sensitivity but higher specificity.
Ring enhancement by intravenous contrast in the arterial wall is the least reliable signal.
Patchwork of discrete tunica intima,
intramural thrombus and outer wall of the vessel may have a Review hampered by CTA 15.
- The Intramural hematoma due to occlusive dissection may not be differentiating mural thrombus occluding the CT 15.
- Causes of false-positive findings on CT and intramural hematoma ATC: atherosclerosis,
arterial wall thickening,
pulsation artifacts,
dental amalgam,
motion artifacts (breathing and swallowing),
ulcerated atheromatous plaques.
Although fibromuscular dysplasia is a recognized cause of DAI,
the contour deformities resulting from arterial disease may provide false positive finding 16.
Magnetic Resonance Imaging and Magnetic resonance angiography
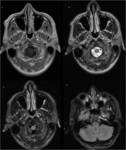
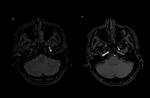
- The sensitivity of magnetic resonance imaging (MRI) and magnetic resonance (MRA) are respectively 84% and 95%,
with a specificity of 99% for both techniques,
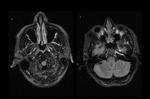
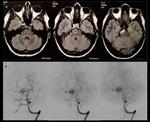
compared with angiography (Figures 13-17) 6,15.
- MRI allows morphological evidence,
measuring the size of the dissection and document intraluminal blood flow,
and the abnormalities identified until months after the initial clinical picture.
The main sequences used in the evaluation of intramural thrombus weights are the spin-echo T1-and T2 with fat suppression techniques in T1 weighting.
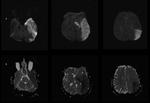
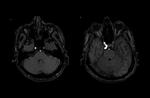
Evaluation protocol for parenchymal ischemic stroke,
as in diffusion weighted (DWI) / ADC map and the evaluation of subarachnoid hemorrhage as GRE T2 weighting,
should be part of the initial evaluation 6.
- The intramural hematoma may present as oval,
or crescent-shaped circumferential and chronological changes in signal intensity varies according to the stage of hemoglobin degradation 3,6.
- The deoxyhemoglobin (acute phase) in intramural hematoma manifests with signal isointense or slightly hyperintense on T1-weighted,
relative to adjacent tissues and hypointense signal on T2 weighting in the intramural hematoma during their initial 48 hours.
Thickening and narrowing of the lumen may be the only signs of dissection in the acute phase,
with greater sensitivity in the anterior circulation DAI due to higher arterial calibers 2,3,6,18.
- The methemoglobin increases the signal strength from the second day until about 3 months (subacute phase),
and the identification of intramural hematoma that more evident estágio.9 technique with fat suppression T1-weighted is an important feature in the subacute phase because differentiates intramural hematoma of atheromatous plaques,
both equally hyperintense without the use of this technique,
accurately identifying the location and extent of the hematoma and its relationship with the anatomical areas involved 6.
- The T2 weight image has a lower weighting in diagnostic value in the individualization of intramural hematoma since the hyperintense signal can be confused with the cerebrospinal fluid.
Lack of signal flow or flow void T2 suggests vessel occlusion14.
The lumen with absent flow signal indicating arterial patency is usually true residual light 6,16.
- Stenosis eccentric,
aneurysmal dilatation and vascular occlusion are important signs of DAI in MR evaluation6,16.
- The dual lumen or pseudolúmen (flap),
considered pathognomonic of DAI,
not always evident on MRI.
However,
Yoshimoto et al,
claim that pseudolumen is best evidenced on MRI than on angiography 2.
- The irregularity of the intimal intramural hematoma due to reduction of the internal diameter of the true lumen or intimal or "rosette signal" can be identified on MRI 19.
- The appearance of a pseudoaneurysm is variable,
depending on their size and the presence of thrombus.
Areas of no signal,
representing residual lumen and areas with mixed signal intensity,
representing thrombi in different phases can be found.
One advantage of MRI angiography relative to this case,
is that it allows to demonstrate the actual size of the aneurysm,
including patent lumen and the intraluminal thrombus,
while angiography shows only the lumen patent 20.
- The MRA can identify changes that are complementary to MRI.
A technical time-of-flight (3D TOF) without gadolinium can demonstrate double lumen (string sign) as pathognomonic of arterial dissection6,12.
- The signal Kantor ( or string sign) is sensitive and specific in angiography and with 3D TOF MRA .
Differential diagnoses are in relation to this signal: stenosis,
hypoplasia and dysplasia with or without dissection.
Important to remember that reducing the flow and turbulence can also simulate this signal 17.
- Identification of intramural hematoma in the subacute phase TOF MRA is an important advantage over CTA9.
Another advantage of TOF MRA is to allow direct identification of the hematoma compared with the phase contrast technique in which tissue is removed altogether static subtraction 20.
- Identification of intramural hematoma in the subacute phase TOF MRA is an important advantage over CTA 9.
Another advantage of TOF MRA is to allow direct identification of the hematoma compared with the phase contrast technique in which tissue is removed altogether static subtraction 20.
- Motions artifacts,
a tendency to overestimate the degree of stenosis,
difficult to detect hematoma in the acute phase and the distinction between slow flow and intraluminal thrombus are the main limitations of MRI and MRA 6.
- Flow turbulent MRI and MRA can manifest with no signal on T1-weighted and be interpreted as a false-positive finding for dissection,
since the arterial wall presents with hyperintense and be confused with hematoma.
Stenosis in major extracranial internal carotid artery can also generate slow flow distal or absence of signal flow and intracranial erroneously be interpreted as resulting from a dissection.
With respect to this finding false-positive,
the CTA is considered a more sensitive method for detection of capillary permeability,
even compared with digital subtraction angiography 20
- The causes of false-positive findings for intramural hematoma on MRI and MRA are: periarterial fat,
periarterial veins near the vertebral arteries,
highlighting flow in veins and periarterial with hypoplastic artery atheromatous plaques 20.
- Conditions are false negative DAI on MRI and MRA,
the diminishment of the hematoma on T1 weighting that behaves isointense deoxyhemoglobin due to the smaller diameter of the vertebral artery dissected be interpreted as normal asymmetry of vertebral and abnormal flow in pseudoaneurysm be judged as solid tumor formation of neural origin or meningioma20
Digital angiography
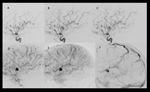
- Cerebral angiography is the gold standard method for diagnosing intracranial arterial dissection,
allowing to accurately identify the location and extent of the dissection,
the integrity and shape of the arterial lumen,
the degree of vascular dilatation,
the degree of stenosis,
irregularities contour of the wall,
the formation of pseudoaneurysms and extravasation of contrast 6.
- The method for being invasive and risk of complications restricts indications in selected cases as aneurysmal dilatation in the vertebral arteries or when the diagnosis remains uncertain after noninvasive methods 6,12.
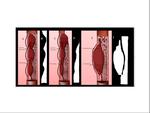
- The cranial arterial dissection is classified into three angiographic patterns: stenotic (most common),
occlusive or aneurysmal (Figure 18).
Since the two dissections can not follow a specific pattern,
Kwak et al also add two angiographic standards: combined and unclassifiable 4.
- The sign of twine / string signal is more frequent angiographic finding of stenotic artery dissections pattern,
defined as segmental narrowing of the lumen,
usually conical and irregular,
with irregular parietal symmetric or asymmetric,
with variable extent4,5.
- The sign of the candle flame (flame sign) can be evidenced in the standard occlusive dissection,
defined as gradual taper that begins cm distal to the carotid bifurcation.
Embolic occlusions can behave with such characteristics,
with a low specificity of this sign for DAI 5.
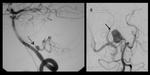
- The pattern is defined as aneurysmal ratio greater than or equal to 1.5 between the diameter of the dissection and normal caliber of the affected artery (Figure 19) 4.
- Dissected segments that determine stenosis associated with dilation of the vascular lumen set the standard and combined its main signal is a "pearl necklace" 4.
- The sign of the "string of pearls" sign or pearl (the string of pearls sign) is the most reliable finding for the angiographic diagnosis of VA dissection,
defined as a focal narrowing associated with dilatation immediately proximal or distal to stenosis (figure 20) 3,16,19.
- In intradural vertebral artery dissection,
the most common pattern is the pattern of aneurysmal dissection followed by combined pattern (Figure 21) 4,5.
- Late retention of contrast medium in the arterial wall,
represented by its influx intramural false,
and another important sign of arterial dissection (Figure 22) 16.
- The intracranial ICA dissections are present on angiography as a sign of string (string sign),
double lumen sign,
irregular stenosis and occlusion of the vessel,
usually seen when the dissection involves the subintimal wall and intramedial 21,22.
- Rarely identify lumens double flaps of the tunica media and external arterial wall. However,
the irregularity of the vessel wall may be the only alteration identified in ICA dissections 6.