Purpose
Pulmonary fibrosis is a progressive disease of the lung parenchyma characterized by varying degrees of interstitial involvement with developement of fibrosis (1).
The clinical course is dismal in the majority of patients,
the median survival is less than 3 years in patients with idiopathic pulmonary fibrosis (1).
Most patients,
however,
are diagnosed late in the course of disease,
when irreversible destruction of lung parenchyma has occurred.
Treatment options are very limited (2,3).
A noninvasive tool to detect changes in lung texture might be helpful for...
Methods and Materials
Method:
Normally the speed of sound is characterized by compressibility of the medium (Longitudinal waves).
In the case of transversal waves (Shear waves) elasticity is the main component and helps to quantify the stiffness of tissues (Fig.
1).
Shear wave imaging uses a push pulse and several tracking pulsesto achieve an image (Fig.
2).
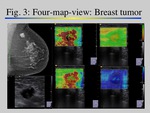
The results are displayed as maps (Fig.
3):
–Shear wave velocity map: Time to peak,
velocity estimates (m/sec)
–Shear wave quality map: Signal to noise level,
displacement magnitude
–Shear wave travel...
Results
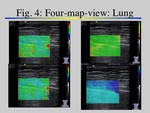
A good quality of the displacement map was achievable in 21/25 healthy patients (Fig.
4).
20/25 had a clear delineation between normal lung and pleura (Fig.
5).
Shear wave velocities varied between 1.8 to 2.5 m/s.
Four false positives seen in the control group are explained by congestion,
a peripheral infiltrate,
one subpleural metastasis and post radiation effects (Fig.
6).
16/20 patients of the fibrosis group had a reduced displacement in the subpleural space correlating with fibrotic areas and honey combing in CT (Fig.
7)....
Conclusion
Although measurements of shear wave velocities in the subpleural space showed a great variation,
the semiquatitative analysis of the displacement map of subpleural lung parenchyma could be a useful tool for diagnosing and noninvasive follow-up controls of early stages of lung fibrosis.
Factors that should be standardized:
–Frequency,
push pulse intensity
–Compression and depth of inspiration
References
1) American Thoracic Society,
European Respiratory Society.
Idiopathic pulmonary fibrosis: diagnosis and treatment..
Am J Respir Crit Care Med 2000; 161: 646–64.
2) Raghu G.
Idiopathic pulmonary fibrosis: new evidence and an improved standard of care in 2012.
Lancet.
2012 Aug 18;380(9842):699-701
3) Raghu G,
Collard HR,
Egan JJ,
for the ATS/ERS/JRS/ALAT Committee on Idiopathic Pulmonary Fibrosis.
An official ATS/ERS/ JRS/ALAT statement: idiopathic pulmonary fibrosis: evidence-based guidelines for diagnosis and management.
Am J Respir Crit Care Med 2011; 183: 788–824