Imaging features:
Ultrasound (US) should be the first line imaging modality in imaging the premenopausal female pelvis.
In some patients will be necessary others diagnostic devices like computed tomography (CT) or magnetic resonance (MR),
especially to evaluated complicated or confusing cases,
if the symptoms are nonspecific and the differential diagnosis is extensive,
when processes beyond the pelvis and a global view is needed,
after-hours availability of CT scanners sometimes CT is the first used.
On the other hand,
MR is not traditionally used in the acute setting for evaluating PID,
only in evaluation of a complex mass in the setting of a confusing clinical picture,
aid in identifying the ovary and to help differentiate pyosalpinx from hematosalpinx (Fig. 3).
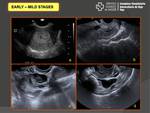
Imaging findings in early stages:
Typically the findings are completely normal in US or often subtle and sometimes non-specific.
Often the only finding is mild enlargement or indistinctness of the uterus.
Patients may also have endometritis,
endocervicitis: Cavities are dilated due to the presence of fluid.
The normal diameter of the fallopian tubes does not exceed 4 mm and they are not visualized by US unless there is fluid in them or they are surrounded by fluid.
In case of salpingitis,
the fallopian tubes become edematous.
There is not tubal dilatation but wall thickening,
enhancement,
and surrounding inflammation.
Enlarged ovaries with increased numbers of small cysts- “polycystic ovary” appearance have been described in ovarian involvement,
as well as fluid in the cul-de-sac (50% of patients with PID) (Fig. 4).
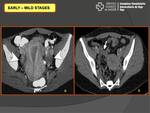
Early imaging findings on CT included:
- Mild salpingitis with inflammatory thickening of the fallopian tubes (Fig. 5)
- Mild oophoritis with enlarged and abnormally enhancing ovaries that may demonstrate a polycystic appearance (Fig. 5)
- Periovarian stranding and enhancement of the adjacent peritoneum
- Endometrial enhancement with intracavitary fluid.
At MDCT the enhancement is slightly less than the adjacent myometrium.
Similar changes in uterine cervix (cervicitis)
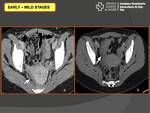
- Mild pelvic edema that results in thickening of the uterosacral ligaments and haziness of the pelvic fat with obscuration of the pelvic fascial planes (Fig. 6).
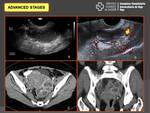
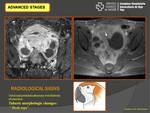
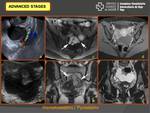
Imaging findings in advanced stages:
HYDRO-PYOSALPINX
- The fallopian tube becomes elongated,
dilated and tortuous,
and contains fluid which,
depending upon its consistency,
may appear anechoic (clear) or with echogenic elements (“string sign”) such as pus (pyosalpinx) or blood (hematosalpinx) (Fig. 7).
- Tubo-ovarian abscess (TOA),
depending on its consistency,
may appear as a homogeneous,
hypoechoic cystic mass or as a mass containing mixed echogenicity areas (more common) (Fig. 8).
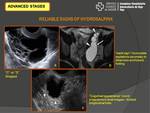
- The most accurate sonographic diagnosis of hydrosalpinx is its tubular nature,
waist sign or small round projections (Fig. 9).
Another sign of hydrosalpinx,
on axial imaging,
is the cogwheel sign (Fig. 9).
DD: The most common feature is the tubular shape which may be distinguished from a pelvic vein by the lack of flow in it and from a loop of bowel by lack of peristalsis.
More specific sign of PID on CT are:
- Pelvic fat stranding and tubal thickening and dilatation filled by complex fluid (pyosalpinx).The wall enhances after the intravenous administration of contrast media.
- TOA: inflammatory mass with solid and cystic components,
with enhancement of all or part of the solid components.
The most frequent appearance of a TOA is the presence of a fluid-containing mass with a thick wall.
Septations may also be present.
A more specific sign of tubo-ovarian abscess,
which is not frequent,
is the presence of gas bubbles.
Anterior displacement of thickened mesosalpinx indicates that the mass is of adnexal origin.
Fluid-filled tubular lesions with enhancing thick walls are findings of pyosalpinx and are frequently seen adjacent to or in a portion of TOAs.
Lymphadenopathy is usually present in the paraaortic region at the level of the renal hila.
Sometimes the ovaries may be detected in the mass.
In such cases the diagnosis of tubo-ovarian abscess is not difficult; if not,
the inflammatory mass may be indistinguishable from inflammatory processes arising from the appendix (appendicular abscess) or diverticula (diverticular abscess).
MR findings in PID are:
The tubular structure is readily identified as cystic,
with high signal intensity on T2- weighted images which is lower than that of a pure cyst and may present lack of internal enhancement (Fig. 8).
Signal intensity on T1-weighted images is variable depending on the protein content of the fluid (Fig. 8).
There is enhancement of the thickened fallopian tube walls and pelvic fat stranding (Fig. 8).
Although the differentiation of pyosalpinx from hydrosalpinx is difficult,
the thick hyperenhancing tubal walls and surrounding inflammation serve as clues to the diagnosis.
TOA
MR imaging findings depend on the hemorrhagic and protein content of the mass.
The abscess is usually hypointense at T1-weighted imaging; however,
hemorrhagic or proteinaceous material can be hyperintense.
A hyperintense rim along the inner wall of the abscess cavity has been described at T1-weighted imaging and is thought to correspond to granulation tissue and hemorrhage.
T2-weighted imaging demonstrates a heterogeneous mass with low- signal-intensity septa,
as well as hypointense linear stranding in the adjacent pelvic fat.
After the intravenous administration of gadolinium-based contrast material,
there is septal and thick rim enhancement in the mass and the surrounding inflammatory stranding.
The meshlike stranding in the pelvic fat corresponds to adhesions and fibrosis,
generating fimbrial obstruction that produces the “beak sign” (Fig. 10).
Edema of the parametrial fat is hyperintense on T2-weighted images.
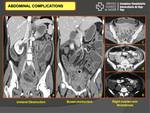
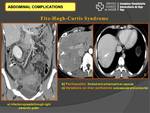
PID complications:
The most frequent complications of PID are the abscesses or pelvic collections and intrabdominal extension with secondary peritonitis (Fig. 11).
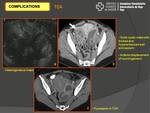
Patients with TOA respond to parenteral therapy.
The rest will need surgical (laparotomy,
laparoscopy,
or image guided percutaneous) drainage (Fig. 12).
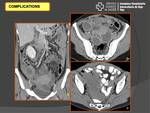
Another frequent manifestation is the presence of heterogeneous and solid - cystic masses with thicked and enhanced with septum that may produce displacement of the round ligament (Fig. 13).
Fitz-Hugh-Curtis Syndrome: peritoneal spread of infection through the right paracolic gutter to involve the peritoneal surfaces of the right upper quadrant (Fig. 14).
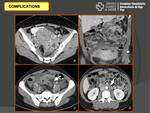
Likewise manifestations related to the size and location of the lesion like urinary obstruction or retention,
bowel obstruction or constipation,
and ovarian vein thrombosis (Fig. 15).
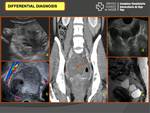
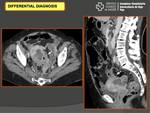
Differential diagnosis:
- Ectopic pregnant
- Ovarian cyst rupture: corpus luteum,
endometrial cyst,
follicular (Fig. 16)
- Anexial torsion (Fig. 16)
- Other pelvic mass (Fig. 16)
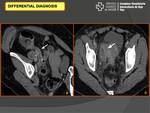
- Appendicitis (Fig. 17)
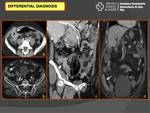
- Terminal ileitis (Yersinia enterocolitica,
Y.
pseudotuberculosis,
Campylobacter jejuni,
and M.tuberculosis) (Fig. 18)
- Inflammatory bowel disease (Crohn,
ulcerative colitis) (Fig. 18)
- Diverticulitis (Fig. 19)
- Bladder and terminal ureter infection.