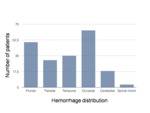
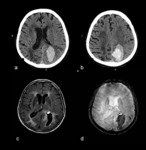
In order to demonstrate the typical features of CAA related cerebral hemorrhage we have browsed through our department’s database for CAA related and other types of bleedings.
Finally,
24 patients with intracranial hemorrhage were selected out of which 8 were suggestive of or proved to be CAA related bleedings.
These CAA patients all showed intracerebral hemorrhage on CT and all were older than 65 years (average 75 years).
Female to male ratio was 6:2.The hemorrhage was often extended,
multilocular (involved 3 lobes on average) and was always situated cortico-subcortically.
At times the hemorrhage showed subdural or subarachnoid propagation or appeared cystic with fluid-fluid levels.
Intraventricular bleeding was rare.
When performed,
MRI scans detected multiplex microbleeds in a cortico-subcortical localization.
The patient data and radiological images were also categorized according to the Boston Criteria.
We classified various clinical and imaging features according to how likely predictors they were for CAA.
Table 2
In the following part we illustrate these findings to highlight the differential diagnostic clues of CAA related bleeding.
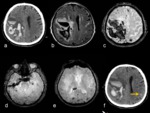
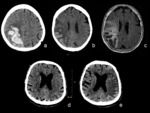
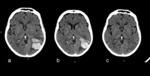
Sample case Fig. 1
Main clues identifiable on imaging:
- lobar hemorrhage defined as: superficially localized bleeding affecting the cortico-subcortical border [6]
- multilocular / multiplex bleeding
- cascade like pattern - multiple ages of hemorrhage indicating slow/steady or rapid/repetitive hemorrhage
- subdural or subarachnoid propagation of the bleeding
- fluid-fluid levels indicating cystic,
cavitated damage
- microhemorrhages detectable on MR
- leukoencephalopathy
- atrophy
Boston Diagnostic Criteria [7]
A,
Histologic sample available - pathology based diagnosis
1.
Definite CAA
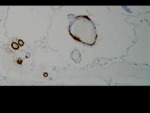
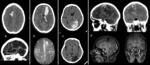
- post-mortem histological examination performed Fig. 2
- gold standard: 100% sensitivity
2.
Probable CAA with pathologic evidence
- some CAA on pathologic specimen (hematoma,
biopsy)
- 67% sensitivity [8]
- increased risk of bleeding
- neurosurgical intervention is often not indicated –> lack of surgical sample –> radiolological image and clinical data remain diagnostic clues
B,
Histologic sample not available - imaging feature based diagnosis
3.
Probable CAA,
based on radiological and clinical data
- multiplex lobar hemorrhage
- age >55 (dementia)
- lack of other cause
Knudsten et al: compared to the post-mortem examination of patients of this “probable” category the radio-clinical image provides a 100% diagnostic accuracy. [9]
Differential diagnostic examples:
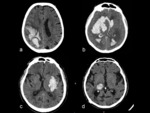
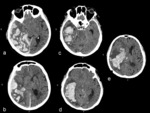
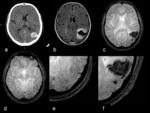
- Hemorrhage localization: cortico-subcortical (lobar) vs. basal ganglia (hypertensive) hemorrhage Fig. 3
- Hemorrhage localization: cortico-subcortical vs.
cortical bleeding Fig. 4
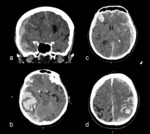
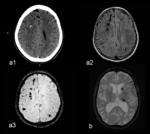
- Multiplex / multilocular hemorrhages Fig. 5
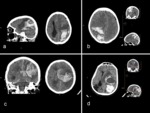
- Multiplex / multilocular hemorrhage + subdural / subarachnoid propagation Fig. 6
- Influence of patient age and clinical history Fig. 7
4.
Possible CAA, based on radiological and clinical data
- unilocular hemorrhage
- age >55
- lack of other cause
Knudsten et al: compared to the postmortem examination of patients of this “possible” category the radio-clinical image provides a 62% diagnostic accuracy. [9]
Differential diagnostic examples of unilocular hemorrhage:
Microhemorrhage (bleedings <5mm) are readily detectable on GRE sequences.
Hemosiderin around these small bleedings cause magnetic filed inhomogenities,
and on sequences which are more prone to magnetic susceptibility microbleeds appear as hypointensities.
In fact,
MR is so sensitive that microhemorrhages in non-symptomatic dementia patients could be used for the screening of CAA. [10]
- MRI microhemorrhage detection,
non-CAA cause.
Fig. 11
- Most common localisation of unilocular bleeding - the occipital lobe Table 3 Possible CAA.
Fig. 12