The best imaging modality for diverticulitis assessment is undoubtedly CT,
especially for its ability to diagnose diverticulitis complications (e.g.: abscesses,
perforation).
Nevertheless,
in our daily practice,
when there is not a clear suspicion of diverticulitis,
the diagnostic algorithm of lower left abdominal pain generally starts with US abdominal and pelvic examination.
US has similar sensitivity and specificity to CT in cases of uncomplicated diverticulitis.
It has some advantages relatively to CT including the lower cost,
the wider availability and the absence of ionizing radiation.
On the other side,
US is operator-dependent and its accuracy is diminished when diverticulitis complications arise.
When the following imaging findings are observed,
the diagnosis of diverticulitis can be assured and CT is not necessary,
unless disease complications are suspected ( Fig. 4 ):
-
- Thickening of the bowel wall.
Mild and uniform wall thickening (wall thickness generally not greater than 5mm on the short axial,
with correctly distended colonic lumen),
that usually extends for a segment larger than 5cm;
- Inflamed diverticulum.
Round echogenic structure with posterior ring-down artifact or a surrounding hypoechoic rim;
- Inflamed pericolic fat.
Increased echogenicity of the pericolic fat.
On the other side,
if diverticulitis is clearly the suspected diagnosis,
there is no need to use US in first place,
and CT is the study to order.
These are the imaging findings that suggest the presence of diverticulitis ( Fig. 5, Fig. 6 ):
- Inflamed diverticulum.
Focal,
paracolic outpouching (diverticulum),
with ill-defined limits,
centered within inflamed fat ;
- Inflamed pericolic fat.
Haziness and stranding of the pericolic fat that is usually very pronounced and disproportionate to the degree of wall thickening;
- Thickening of bowel wall.
As previously described.
The transition between the normal and thickened wall is progressive,
without “shouldering”;
- Microperforation.
Small pockets of extraluminal gas ( Fig. 7 , Fig. 8 );
- Centipede sign.
Representing engorgement of the vasa recta that “feed” the colonic segment where the diverticulum is located ( Fig. 9 );
- Comma sign and reverse comma sign.
These signs represent thickening of the lateroconal fascia,
a finding frequently seen in colonic diverticulitis (it is nevertheless an unspecific finding,
associated to other pathologies).
“Comma sign” is a left-sided finding,
secondary to descending/sigmoid diverticulitis,
while “reverse comma sign” occurs in the right side,
secondary to right-side diverticulitis ( Fig. 10 ).
- COMPLICATIONS OF DIVERTICULITIS
Generally diverticulitis is a self-limited process yet frequently recurrent,
resolving without sequelae when the treatment is adequate.
In most cases treatment is simple,
involving bowel rest,
intravenous hydration and antibiotherapy.
However,
complications can occur,
difficulting the resolution of the inflammatory process and adding long-term morbidity to diverticular disease.
As previously described,
CT is the advised imaging resource to evaluate these possible events.
The most important complications of diverticulitis are:
ABSCESS ( Fig. 11 )
Pericolic abscess is a frequent complication of diverticulitis,
occurring in up to 30% of cases.
Small abscesses (< to 4cm) are generally managed medically,
with antibiotherapy.
When larger than 4cm,
diverticular abscesses should be treated by drainage.
Because of portal venous inflow,
hepatic abscesses can infrequently occur and imaging guided drainage can also be necessary.
Imaging findings: fluid collection with contrast-enhancing walls.
It may present gas in its interior.
PERFORATION ( Fig. 12 )
Gross perforation is a rare complication occurring in 1-2% of the cases.
If not treated quickly and appropriately,
the spillage of colonic content soon induces fecal peritonitis,
aggravating the prognosis.
The risk of colonic perforation is the reason why diagnostic procedures like barium enema or colonoscopy are contraindicated in the evaluation of acute diverticulitis.
Imaging findings: free intra-abdominal air associated with ascites and enhancement and thickening of the peritoneum if peritonitis develops.
FISTULAE ( Fig. 13 )
Fistulization arises when inflammatory changes resulting from perforation erode the skin or adjacent viscera.
It involves most frequently other colonic segments and the bladder (up to 65% of cases).
(Diverticulitis,
nejm) Fistulous tracts to the skin or female pelvic organs can also occur,
but are less frequent.
Imaging findings: colo-colonic fistulae are difficult to detect but occasionally a sinus tract with gas in its interior can be seen communicating two segments of colon,
with inflammatory changes of nearby tissues.
In the case of bladder fistulization,
the most frequent and significant finding is the presence of endoluminal gas bubbles.
OBSTRUCTION ( Fig. 14 )
Small bowel or colonic obstruction can be an acute,
subacute or chronic complication of diverticulitis,
impeding the passage of enteric / fecal bowel content,
with surgical correction being frequently necessary.
When the obstruction is secondary to chronic diverticulitis the findings can be quite similar to colorectal cancer.
Imaging findings: caliper reduction of bowel segment with dilation of upstream intestinal segments.
In cases of chronic diverticulitis,
the presence of diverticula is the single strongest morphological feature pointing to this diagnosis.
Other suggestive finding is the presence of a long segment (generally > 10 cm) of mildly thickened colon.
PYOPHLEBITIS ( Fig. 15 )
Pyophlebitis represents thrombosis of mesenteric or portal veins secondary to intra-abdominal inflammatory or infectious process,
including diverticulitis.
It has a poor prognosis.
Imaging findings: absence of opacification of portal or systemic venous vessels that is generally associated to some degree of vessel engorgement.
The clinical picture of diverticulitis is quite unspecific and can be seen in different pathologies,
from vascular to neoformative,
inflammatory and other kind of insults.
Despite this,
there are some differences that can help attaining a specific diagnosis.
COLORECTAL CANCER ( Fig. 16 )
One of the most important differential diagnosis of diverticulitis is colon adenocarcinoma,
and the imaging overlap between these 2 pathologies is estimated to be around 10%.
Adenocarcinoma of the colon is most frequently seen in the descending or sigmoid segments and,
like diverticulitis,
can also be associated with complications like obstruction,
perforation or fistulization.
Key imaging findings: colorectal neoplasms are generally seen as a short (˂ 5cm) segment of severe,
irregular,
non-stratified and eccentric thickening of the colonic wall,
with sudden transition between the normal and abnormal wall.
The inflammatory changes of pericolic tissues are minimal (except when complications are seen) and local lymphadenopathies are usually present.
DIAGNOSTIC PEARL: the disproportion between the large degree of colonic wall thickening and the slight pericolic fat densification and stranding.
Presence of lymphadenopathies.
Sigmoidoscopy after the resolution of acute symptoms may be useful is doubtful cases.
EPIPLOIC APPENDAGITIS ( Fig. 17 )
This is a relatively rare ischemic and inflammatory condition that occurs with torsion and subsequent ischemia of the epiploic appendages,
pedunculated fatty structures arranged over the external aspect of the colon that extend from the cecum to the rectosigmoid junction.
Imaging findings: at CT there is a small (1-4cm) ovoid paracolic lesion with fat density,
surrounded by hyperdense rim (representing the inflamed visceral peritoneum that covers the appendage),
with a small central dot that represents engorged or thrombosed vessels.
There is densification and stranding of the pericolic fat with mild and asymmetric thickening of the adjacent colonic wall.
DIAGNOSTIC PEARL: thetypical aspect of an ovoid paracolic fatty lesion with inflammatory changes in the pericolic fat and slight thickening of the bowel wall.
OMENTAL INFARCTION ( Fig. 18 )
Like epiploic appendagitis,
infarction of the omentum also occurs with torsion and vascular insults resulting from trauma or spontaneous thrombosis of the omental veins.
It is more frequent at the right quadrants of the abdomen,
but can occur wherever there’s omentum.
Imaging findings: large non-enhancing mass (generally > 5cm) with heterogeneous attenuation,
representing the infarcted tissue and pericolic inflammation.
Slight bowel thickening can occur but is extremely disproportionate relatively to the large ischemic and inflammatory mass.
DIAGNOSTIC PEARL: the disproportion between the large inflammatory mass (greater than epiploic appendagitis) and the slight degree of thickening involving a short segment of colon.
INFLAMMATORY BOWEL DISEASE ( Fig. 19 )
Inflammatory bowel disease is divided in 2 similar idiopathic entities most frequently diagnosed in early adulthood: Crohn disease and ulcerative colitis.
While Crohn disease most frequently involves the small bowel and the right colon with “skip areas” between the pathologic bowel segments,
ulcerative colitis is limited to the colon and rectum (the terminal ileum may also be involved due to “backwash ileitis”) in a continuous pattern – without “skip areas”,
being typically left-sided.
It is important to notest that the rectum is always involved in ulcerative colitis,
constantly presenting inflammatory changes unless the patient is being treated with anti-inflammatory enemas.
The rectum is typically spared in Crohn disease.
In this group of diseases it is acute ulcerative colitis that can be confounded with diverticulitis because,
like diverticulitis,
it generally occurs in the left-sided colon.
Imaging findings: in acute ulcerative colitis the segment of inflamed bowel is generally more extensive than in diverticulitis (sometimes a pancolitis occurs) and the thickening is symmetric and occasionally stratified - “water halo sign” (representing submucosal edema,
an unspecific finding seen in different types of colitis).
DIAGNOSTIC PEARL: the large extension of colonic inflammatory involvement.
There may be sequelae of chronic inflammation as the “fat halo sign” (representing submucosal fat deposition),
proliferation of peri-rectal fat or the “lead pipe sign” (representing loss of normal haustral markings,
luminal narrowing and bowel shortening).
INFECTIOUS COLITIS ( Fig. 20 )
There is a large number of microorganisms that can cause colitis and frequently the clinical and imaging findings overlap.
Most of them can manifest as pancolitis,
while some agents have predilection for the right colon (e.g.: tuberculosis) and others for the left colon (e.g.: shigellosis).
There is a subtype of infection that should be highlighted due to its etiology and severity – pseudomembranous colitis.
Pseudomembranous colitis is caused by Clostridium difficile,
a commensal gastrointestinal organism that overgrows with antibiotherapy or chemotherapy,
causing bowel damage due to the production of exotoxins.
The majority of patients is affected by diffuse diarrhea and abdominal cramps,
consequence of superficial mucosal disease.
However,
severe cases can progress to toxic megacolon with pronounced colonic distension and risk of transmural injury and perforation.
Imaging findings: the different types of infectious colitis are associated to colonic wall thickening,
pericolic densification and stranding,
with possibility of ascites.
Severe cases of pseudomembranous colitis however,
present with markedly thickened and edematous bowel wall with irregular and polypoid mucosal contour.
The degree of wall thickening may reveal the accordion sign,
representing entrapment of positive oral contrast between the thickened bowel haustra.
The colonic diameter may be greatly augmented.
DIAGNOSTIC PEARL: the infectious clinical and laboratorial picture,
and the large extension of colonic inflammatory changes.
ISCHEMIC COLITIS ( Fig. 21 )
Acute ischemic colitis is the most common form of intestinal ischemia,
being almost invariably associated to sudden hypoperfusion,
affecting predominantly the elder generation.
The colonic segments more frequently involved are the “watershed areas” like the splenic flexure (Griffith point,
representing the junction between the distribution of the superior and inferior mesenteric arteries) and the rectosigmoid junction (point of Sudeck,
representing the anastomotic plexus between the inferior mesenteric artery distribution and the hypogastric vascular supply) (CT Imaging of Colitis).
Clinically it ranges from transient episodes of mucosal and submucosal ischemia to catastrophic cases of transmural infarction with bowel necrosis.
Imaging findings: generally there are unspecific findings of segmental involvement of the colon traduced by various degrees of wall thickening.
The length of the involved colon is varied,
ranging from small segments (around 5cm) to involvement of the whole colon (which is infrequent).
The thickened wall is generally edematous,
enhancing homogeneously or heterogeneously.
Varying degrees of pericolic densification may follow and ascites can be seen.
In severe cases circumferential intra-mural air can be seen – pneumatosis coli,
occasionally followed by portomesenteric venous gas,
suggesting transmural necrosis.
DIAGNOSTIC PEARL: theendoscopic visualization of petechiae and eritematous mucosa in the acute phase,
evolving to cyanotic and ulcerated mucosa in severe cases.
It is important to emphasize that the clinical / radiological suspicion of ischemic colitis is confirmed by colonoscopy.
FOREIGN BODY PERFORATION ( Fig. 22 )
Ingestion of a non-digestible item is a relatively common finding,
especially in people who wear dentures as the recognition of small intra-oral objects is reduced due to the incapacity of taking advantage of soft palate tactile sensitivity.
Digestive tract perforation is a rare finding however,
generally associated to sharp objects (animal bones,
toothpicks,
metal objects) and it occurs occasionally in the colon but most frequently in the small bowel.
Clinical findings may vary from slight abdominal pain and nausea to established peritonitis.
Imaging findings: if dense enough,
perforating foreign bodies can usually be seen as linear structures traversing the bowel wall.
It is more probable to identify metallic and bony objects than pieces of wood (like toothpicks).
Additional findings like small bubbles of extraluminal gas adjacent to an area of thickened bowel wall and densified/stratified mesenteric fat,
frequently associated to an extramural abscess,
support this diagnosis.
DIAGNOSTIC PEARL: thevisualization of a linear hyperdense structure traversing the bowel wall associated to colonic and pericolic inflammatory findings.
INFLAMMATORY PELVIC DISEASE (IPD) ( Fig. 23 )
Inflammatory and infectious disease of the upper genital tract is a relatively frequent diagnosis,
generally seen in sexually active young females.
The use of contraceptive intrauterine device is a risk factor.
Clinically,
IPD manifests with lower abdominal pain,
abnormal vaginal discharge,
utero-anexial tenderness and fever with leucocytosis.
The diagnosis is supported by imaging,
mainly ultrasound.
Complications like endometrits,
salpingitis,
tubo-ovarian abscess or even peritonitis can develop in some cases.
Occasionally,
inflammatory changes resulting from advanced or complicated IPD can involve adjacent pelvic segments of bowel and mesenteric fat,
making difficult to distinguish this diagnosis from other pathologies as diverticulitis.
Imaging findings: the first line examination for suspected IPD is endocavitary ultrasound.
Possible sonographic findings include endometrial thickening with or without fluid/gas,
ovarian and uterine enlargement with poorly defined borders,
free intraperitoneal fluid and pelvic mesenteric fat inflammation.
Complicated tubo-ovarian abscesses can originate complex adnexal masses.
CT in IPD is mainly used to evaluate possible complications (e.g.: tubo-ovarian abscesses) or when it is necessary to exclude other possible differential diagnoses.
At CT,
non-complicated DIP does not present significant findings,
except perhaps a small amount of fluid in the cul-de-sac.
With advanced cases and progression to tubo-ovarian abscess,
findings include thick-walled,
septated,
low attenuation complex masses,
occasionally associated to serpiginous structures,
representing the dilated fallopian tubes.
Internal gas is a quite specific but very unusual finding.
Thickening of the uterosacral ligaments,
increased attenuation of the presacral fat and loss of definition of the margins of adjacent bowel loops suggest the diagnosis of IPD.
DIAGNOSTIC PEARL: the clinical picture of a febrile young woman with abnormal vaginal discharge with good response to antibiotics,
associated to utero-anexial positive imaging findings is suggestive of IPD.

![Fig. 4: “Diverticulitis”. (A, B) Abdominal ultrasound study reveals mild and homogeneous thickening of the sigmoid colon wall [*] associated to a round echogenic structure with posterior “ring-down” artifact, representing an inflamed diverticulum [arrow]. There is slight hiperechogenicity of the pericolic fat [Δ]. (C) Abdominal ultrasound study of another patient demonstrates mild thickening of the descending colon wall [*] and round slightly echogenic focus surrounded by a hypoechogenic rim, revealing the inflamed diverticulum [arrow]. There is also hyperechogenicity of the pericolic fat [Δ].](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504307?maxheight=150&maxwidth=150)
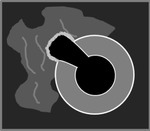
![Fig. 6: “Diverticulitis”. (A, B, C, D) Axial unenhanced abdominopelvic CT study, reveals ill-defined sigmoid diverticula [arrow] associated to mild wall thickening [*] and pericolic fat haziness and stranding [Δ]. The inflamed diverticulum in (D) is spontaneously dense and not air-filled [arrow]. (E) Axial contrast enhanced abdominopelvic CT study reveals ill-defined diverticulum of the sigmoid colon [arrow] (which is redundant and partially located at right), with associated pericolic inflammatory changes [Δ] and wall thickening [*], representing right-sided sigmoid diverticulitis. (F) Axial contrast-enhanced abdominal CT study reveals well-defined air-filled jejunal outpouching, representing a jejunal diverticulum [arrow]. Medially to this diverticulum, there is a heterogeneous image in the mesenteric border of the jejunal wall, with incomplete borders and tiny bubbles of air adjacent to it, representing a perforated jejunal diverticulum with peridiverticular abscess [circle]. There is associated haziness of the mesenteric fat, representing inflammatory changes [Δ]. This is a case of perforated jejunal diverticulitis. Jejunal diverticula are quite rare findings, most frequently asymptomatic.](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504324?maxheight=150&maxwidth=150)

![Fig. 8: “Microperforation”. (A, B) Axial unenhanced abdominopelvic CT study (A) reveals ill-defined air-filled outpouching [arrow] of the descending colon, associated to mild wall thickening [*] and pericolic fat haziness with stranding [Δ], suggesting diverticular inflammation. Axial contrast enhanced images of more cranial segments (B) also reveal wall thickening [*] with pericolic inflammation [Δ] and a tiny bubble of extraluminal gas near the abdominal wall [circle], resulting from microperforation of the inflamed diverticulum in (A). (C) Axial unenhanced abdominopelvic CT study from a different patient reveals a small bubble of extraluminal gas [arrow] and fat haziness [Δ]. These findings result from microperforation of the inflamed sigmoid diverticulum, not represented in this image. There are also tiny diverticula in the proximal sigmoid [circle].](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504338?maxheight=150&maxwidth=150)
![Fig. 9: “Centipede sign”. (A, B) Axial unenhanced abdominopelvic CT study demonstrates wall thickening of the sigmoid colon [*] with engorged pericolonic vessels – “centipede sign” [Δ], surrounding ill-defined air-filled diverticulum [arrow]. (C) Axial unenhanced abdominopelvic CT of a different patient reveals mild wall thickening [*] and the “centipede sign” [Δ]. The inflamed diverticulum is not seen in this image.](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504345?maxheight=150&maxwidth=150)
![Fig. 10: “Comma sign and reverse comma sign”. (A, B, C) Axial contrast enhanced (A, B) and unenhanced (C) abdominopelvic CT studies of three different patients demonstrate thickening of the left lateroconal fascia – “comma sign” [arrow], secondary to sigmoidal diverticulitis. The inflamed diverticulum is only seen in (A) [circle], with pericolic haziness [Δ]. There are also several other non-inflamed diverticula in (A). (D) Axial unenhanced abdominopelvic CT of a different patient reveals thickening of the right lateroconal fascia – “reverse comma sign” [arrow] and pericolic haziness and stranding [Δ], secondary to right sided diverticulitis [circle].](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504347?maxheight=150&maxwidth=150)
![Fig. 11: “Abscess”. (A, B) Axial contrast-enhanced abdominopelvic CT study reveals small pericolic collection [arrow] with air bubbles in its interior (A), representing a peridiverticular abscess, secondary to diverticular perforation. Pericolic haziness and stranding is also seen, supporting the inflammatory diagnosis [Δ]. (C, D) Axial contrast-enhanced pelvic CT study demonstrates a large and heterogeneous pelvic collection with contrast-enhancing walls (arrow). The patient had sigmoid diverticulitis documented three weeks ago. There is still sigmoid wall thickening [*]. (E, F) Abdominal ultrasound study (E) reveals large segment VIII hepatic abscess, heterogeneous, hypoechogenic, with thick echogenic walls. This collection is well-defined, heterogeneous and hypodense in axial contrast-enhanced abdominal CT study (F).](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504411?maxheight=150&maxwidth=150)
![Fig. 12: “Perforation”. Axial abdominopelvic CT study of the same patient at the time of diagnosis (A, B) and two days later (C, D). The initial unenhanced study reveals, in (A), an ill-defined diverticulum [arrow] with associated pericolic haziness and engorged vasa recta – “centipede sign” [Δ]. In (B) there are tiny extraluminal gas bubbles [circle], suggesting microperforation. Two days later a contrast-enhanced CT was performed, due to aggravated abdominal pain. The images reveal greater amount of free and widely distributed intraperitoneal air [*].](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504421?maxheight=150&maxwidth=150)
![Fig. 13: “Colovesical fistula”. Axial contrast-enhanced abdominopelvic CT study reveals an inflamed diverticulum [circle] with associated sigmoid wall thickening [*], thickening of the left lateroconal fascia – “comma sign” [arrow] and small amount of fluid in the cul-de-sac [Δ] (A). Several weeks later the patient was re-examined due to persistent hypogastric pain, repetition cystitis and possible pneumaturia. Marked thickening of the bladder wall and intraluminal air [circle] suggest colovesical fistula secondary to diverticulitis complication.](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504436?maxheight=150&maxwidth=150)
![Fig. 14: “Sigmoid colon obstruction secondary to chronic diverticulitis”. Axial unenhanced abdominopelvic CT study of a patient with diffuse abdominal pain, constipation and personal history of several episodes of diverticulitis in the past. The images reveal a relatively abrupt transition separating practically collapsed distal sigmoid [arrow] and distended proximal sigmoid [Δ]. The point of transition is relatively short and thickened [*], findings not quite suggestive of chronic diverticulitis. Nevertheless, there are several diverticula in this region [circles]. The bowel loops are markedly dilated (B). These findings were firstly diagnosed as secondary to possible sigmoid adenocarcinoma and colonoscopy was suggested. Colonoscopy did not demonstrate any neoformative lesion. Due to the patients personal history and the presence of some diverticula distally, the diagnosis of chronic diverticulitis is most likely.](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504446?maxheight=150&maxwidth=150)
![Fig. 15: “Portal pyophlebitis”. Axial (A) and coronal (B) contrast-enhanced abdominal CT reveals absence of contrast opacification and dilation of the portal vein [Δ], secondary to septic thrombosis. There are multiple hepatic abscesses associated [*]. These septic vascular catastrophe was secondary to complicated diverticulitis, as seen in axial contrast-enhanced pelvic CT images acquired a week earlier (C), demonstrating diverticular perforation [arrow] with extraluminal air [*].](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504462?maxheight=150&maxwidth=150)
![Fig. 16: “Colorectal cancer”. Axial (A), coronal (B) and sagittal (C) contrast-enhanced abdominopelvic CT reveals severe and irregular thickening of the colonic wall [Δ], contrast enhancing, non-stratified, with slight haziness of the pericolic fat, conditioning abrupt transition from the upstream bowel segments, which are markedly dilated. These findings were highly suspicious and sigmoid adenocarcinoma was confirmed at colonoscopy and histology. There is at least one prominent satellite metastatic lymph node in these images [circle]. Abdominal ultrasound of a different patient (D, E, F) demonstrates severe, irregular and eccentric parietal thickening of the descending colon (D, E), with little satellite metastatic lymph nodes (F). This was also confirmed as colorectal cancer.](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504484?maxheight=150&maxwidth=150)
![Fig. 17: "Epiploic appendagitis". Axial unenhanced (A) and contrast-enhanced (B, C) abdominopelvic CT shows a well-defined paracolic lesion with fat density [*], surrounded by a hyperdense rim and presenting a discrete central density (A, B). There is also some pericolic haziness [Δ], with occasional thickening of the lateroconal fascia [arrow]. There is no significant parietal thickening of the colon.](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504500?maxheight=150&maxwidth=150)
![Fig. 18: “Omental infarction”. Axial unenhanced abdominal CT of the same patient at different levels (A, B) shows an ill-defined, heterogeneously dense paracolic mass [Δ]. There is no significant colonic wall thickening. Abdominal ultrasound of the same patient reveals a hyperechogenic and relatively homogenous mass [*] adjacent to the descending colon [arrow].](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504506?maxheight=150&maxwidth=150)
![Fig. 19: “Ulcerative colitis”. Axial contrast enhanced pelvic CT study (A) reveals diffuse parietal hyperenhancement and thickening of the sigmoid colon [arrow], a finding compatible with active phase of ulcerative colitis. The sigmoid and some small bowel segments are moderately distended by liquid / semi-liquid content [*]. In (B) axial contrast enhanced pelvic CT study shows significant proliferation of peri-rectal fat [circle], suggesting chronic disease. However the peri-rectal fat is quite densified and the rectal wall is stratified and edematous – “water halo sign”, findings that suggest disease activity in long term ulcerative colitis. Coronal contrast enhanced abdominopelvic CT (C) clearly demonstrates the “lead pipe sign” in the descending colon, with loss of normal haustrae [arrow]. This colonic segment is nevertheless edematous and stratified, suggesting disease activity. The ascending colon preserves its normal haustration pattern and there is no evidence of active / chronic disease [ellipse].](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504514?maxheight=150&maxwidth=150)
![Fig. 20: “Infectious colitis”. (A) Abdominal ultrasound shows moderate ascending colon parietal thickening in a 8-year-old with fever and diarrhea. The whole colon had this aspect. (B) Cytomegalovirus pancolitis with significant wall thickening, hyperenhancing mucosa and luminal distension. (C, D) Axial contrast-enhanced CT abdominopelvic CT studies of the same patient separated by five days. The patient had previously been treated with amoxicillin, and presented with profuse diarrhea and painful abdominal cramps. "Clostridium difficile" was isolated in the stool. In (C) there is extremely marked colonic wall thickening due to edema and the colon lumen is almost virtual [arrows]. There is also significant amount of ascites [*], indicating disease severity. The patient did not show improvement and a new CT was acquired five days later (D): the colon is significantly distended and the mucosa is thin [arrows], suggesting toxic megacolon. Ascites is still present [*].](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504524?maxheight=150&maxwidth=150)
![Fig. 21: “Ischemic colitis”. Axial contrast-enhanced CT study reveals significant edematous thickening and stratification of the splenic flexure of the colon [arrow], with pericolic haziness implying edematous infiltration of the involving fat [Δ]. The other colonic segments were completely normal. Colonoscopy confirmed the diagnosis of ischemic colitis in this watershed area.](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504533?maxheight=150&maxwidth=150)
![Fig. 22: “Foreign body perforation”. Coronal (A) and axial (B) contrast-enhanced CT study reveals significant densification and phlegmonous alterations of the mesenteric fat [Δ], involving a spontaneously hyperdense linear structure compatible with a foreign body [circle], also imaged in ultrasound (C) [arrow]. This image was in intimate contact with a jejunal loop, suggesting bowel perforation. At this time there were no organized collections or extraluminal air.](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504541?maxheight=150&maxwidth=150)
![Fig. 23: “Tubo-ovarian abscess”. Pelvic transabdominal ultrasound (A, B) reveals an expansive hypoechogenic formation with hyperechogenicity of the adjacent mesenteric fat, in a young female with fever, pelvic pain and dyspareunia. Axial (C, D) and coronal (E) contrast-enhanced CT study was obtained to clarify the nature of the lesion. The possibilities included complicated DIP or complicated diverticulitis. CT revealed a heterogeneous lesion originating in the left adnexal region [arrow], with haziness and stranding of the involving fat [Δ], reinforcing the diagnosis of complicated DIP with tubo-ovarian abscess. An intrauterine dispositive is also seen [circle].](https://epos.myesr.org/posterimage/esr/ecr2013/116902/media/504551?maxheight=150&maxwidth=150)
