Overview of TIPS:
By relieving portal hypertension,
TIPS creation is now an established procedure for prevention of variceal bleeding and treatment of refractory variceal bleeding and refractory ascites,
among other complications of portal hypertension [1].
Conventionally,
the general steps of the procedure include:
1) Cannulation of the hepatic venous system via percutaneous right internal jugular vein access
2) Measurement of pre-shunt hepatic pressures
3) Visualization of the hepatic/portal venous system,
to target shunt placement
4) Transhepatic puncture into the portal venous system from the hepatic venous system
5) Portosystemic shunt creation with insertion of stents along the punctured tract
6) Measurement of post-shunt portal pressure,
with dilatation of shunt as needed
Complications related to portal vein puncture in TIPS:
However,
TIPS procedure-related complications can occur [2].
One particularly fraught and unpredictable step in TIPS is the transhepatic portal vein puncture,
which involves an essentially blind puncture of the central aspect of the portal venous system (typically the right portal vein near its confluence into the main portal vein),
via a needle throw from the central aspect of the hepatic venous system (typically in the anteroinferior direction from the more posterosuperiorly-located right hepatic vein).
Due to the blind nature of the puncture,
multiple passes may be required until the portal venous system is successfully punctured,
and with each pass comes risk of unintentional puncture/injury of nontarget structures,
such as hepatic structures (hepatic artery,
biliary system,
liver capsule) or nearby extrahepatic organs (eg,
right kidney puncture <2% [3]).
Although unintentional punctures are usually well-tolerated,
consequences can include biliary fistula formation (<5% [3]),
symptomatic hepatic arterial injury (<2% [3-4]),
or organ-specific damage,
and may require follow-up intervention.
Portal vein targeting in TIPS:
Improvement of portal vein targeting is crucial to decreasing the number of passes and the inherent risks.
Preprocedure imaging allows for consideration of anatomic variants and vessel patency but is not real-time.
Bony anatomic landmarks are helpful [5] but can vary relative to the portal vein position through different phases of respiration.
Thus,
other methods of portal vein targeting have been developed.
Wedged hepatic venography (WHV) is commonly used,
with placement of either a directly-wedged catheter/sheath or balloon occlusion catheter into a selected hepatic vein,
followed by injection of either iodinated or carbon dioxide contrast into the wedged hepatic vein for retrograde outflow into the portal venous system,
which can then be used as a roadmap for targeting.
An additional benefit of this method is that the order of portal vein branch opacification can help deduce which hepatic vein branch has been selected and wedged.
However,
this roadmap is not real-time and cannot account for changes in view or respiratory motion.
The injection of contrast in WHV has also been associated with liver laceration (up to 7.5% with iodinated contrast [6],
1.8% with the less viscous carbon dioxide [7]),
and even capsular injury requiring intervention [8].
Since the risk of bleeding in capsular injury may be worse in the presence of ascites,
preprocedure paracentesis has been advocated.
An additional disadvantage of carbon dioxide WHV (cWHV) is requirement of a high imaging frame rate,
increasing operator radiation exposure.
Another less commonly utilized option is intraprocedure ultrasound,
which allows for real-time visualization of hepatic vessels and structures without the use of contrast [9]; however,
its use is highly operator-dependent and sonographic visualization of the needle and other objects can be difficult.
Other more invasive techniques of portal vein targeting include cannulation of an enlarged umbilical vein [10],
transhepatic placement of a portal vein guidewire [11] or periportal coil,
or the transhepatic "gunsight" approach with placement of endovascular snares/wires for direct portocaval shunt [12].
However,
transhepatic and transvariceal approaches can be technically difficult and are risky in patients with coagulopathy,
particularly those with ascites,
both common issues in the patient population undergoing TIPS [3].
A lesser-known but relatively straightforward portal vein targeting technique,
using a hepatic artery microguidewire as a target,
has been advocated by Matsui et al [13] and Yamagami et al [14],
taking advantage of the hepatic artery’s companion course with the portal vein.
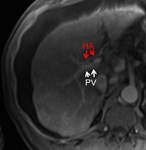
The hepatic arterial system typically courses anterior to the portal venous system in the portal triad (Fig.
1),
therefore a particularly convenient target for a portal vein-directed needle throw that typically begins in the more posteriorly-located right hepatic vein.
Placement of a periportal hepatic artery guidewire allows for real-time targeting,
and the arterial access additionally allows for mesenteric and celiac portography,
which can demonstrate both the portal venous anatomy and any associated varices in real-time.
It can be performed safely and efficaciously by even less experienced operators and without the need for additional apparatus unlike in carbon dioxide wedged hepatic venography.
Yamagami et al [14] had a 100% success rate of TIPS creation without any symptomatic puncture-related complication,
even when this technique was utilized by operators who did not frequently perform TIPS procedures,
for 11 cases over a 5-year span.
Although guidewire-related thrombus formation may be a theoretical concern [15],
the liver is an organ rich in collateral supply,
so hepatic artery microguidewire-related thrombus formation is of lesser concern,
particularly in the cirrhotic population,
which has high rates of coagulopathy and thrombocytopenia.
Microguidewires have a relatively low profile and have been used quite successfully in cardiac and neurological interventions.
Here,
we consider the outcomes in a 6-year series of TIPS creation cases,
with hepatic artery guidewire versus with carbon dioxide wedged hepatic venography,
supervised by a single operator at our institution.