Type:
Educational Exhibit
Keywords:
Arteriovenous malformations, Contrast agent-intravenous, Ultrasound-Colour Doppler, CT-Angiography, CT, Liver, Anatomy, Abdomen, Congenital
Authors:
F. Tavanti1, D. Sergi2, C. Bernardi1, C. De Vincentiis1, M. Di Pietropaolo3, A. Pallavicino1, L. Stefanetti3, V. David1; 1Roma/IT, 2reggio calabria/IT, 3Rome/IT
DOI:
10.1594/ecr2013/C-1934
Imaging findings OR Procedure details
The diagnosis of CEPS is made with US,
CT,
MR imaging,
or sometimes angiography.
US is the initial examination for patients with nonspecific liver disease,
because it is non-invasive and may demonstrate the absent PV in most cases.
Doppler US is also useful to determine the flow direction of the identified vessels.
Both CT angiography and MR angiography depict the course of the porto-systemic shunt and allow identification of the absent portal branches.
Despite MR Angiography not exposing patients to ionizing radiation must be considered the first-choice exam,
also in the evaluation of associated focal hepatic lesions,
Multidetector CT demonstrated better spatial resolution in the detection of abnormal vasculature.
Thus post-processing techniques,
such as maximum intensity projection,
multiplanar reformation and volume rendering,
provide additional information [5,8].
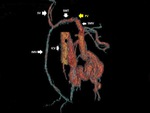
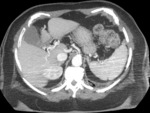
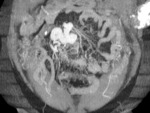
We suspected Abernethy syndrome type 1 (Fig.1) in a 86-year-old female with hepatic encephalopathy in which an abdominal contrasted-enhanced CT scan highlighted a normal appearance of the liver (Fig.2) in presence of multiple collateral circles draining blood directly in vena cava (Fig.
3),
in the absence of portal vein.
The patient had remained,
although she had a congenital malformation,
asymptomatic for years,
before presenting signs of porto-systemic encephalopathy.
This is the first case of Abernethy malformation described in an old patient.