- Angiographic features.
Angiographic features of the six patients are summarized in Table 2.
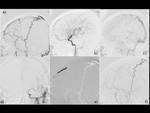
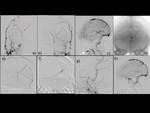
The paramedian branches of the middle meningeal artery and the frontal and parietal branches of the superficial temporal artery supplied the SSS-DAVF bilaterally in all patients.
The anterior falx arteries,
which originate from the ophthalmic artery,
supplied the SSS-DAVF in 4 patients,
and the transosseous branches of the occipital artery supplied the SSS-DAVF in 2 patients.
Shunted pouches were found in all 6 patients,
which were located superolaterally or superomedially to the main lumen of the SSS.
In all cases,
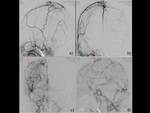
the SSSs were occluded and the shunted blood drained retrogradely via the cortical venous anastomosis into the cavernous sinus and/or the transverse sinus,
the posterior part of the SSS,
and the inferior sagittal sinus.
Cerebral venous blood from the affected areas of the brain drained via cortical venous anastomoses with significant congestion was seen in 4 patients.
In the remaining 2 patients,
cerebral venous blood from the affected areas of the brain partially drained via the isolated SSS into the epidural veins and/or emissary vein.
All cases showed occlusion of the SSS,
and 3 cases showed bilateral TSS occlusion.
3 patients showed coexistence of DAVFs in other locations,
namely the cavernous sinus (CS) in 1 patient,
the TSS in 1 patient,
and both CS and TSS in 1 patient.
Table 2: Angiographic features
| |
Feeder |
Normal cerebral venous drainage via affected SSS |
Patency of the other sinus |
Coexistence of dAVF in other locations |
| 1 |
MMA,
anterior falx artery |
no |
yes |
no |
| 2 |
MMA,
STA,
anterior falx artery |
no |
yes |
no |
| 3 |
MMA,
STA,
anterior falx artery |
yes |
no |
no |
| 4 |
MMA,
STA,
anterior falxartery |
no |
yes |
lt.CS |
| 5 |
MMA,
STA |
no |
no |
lt.CS,lt.TS |
| 6 |
MMA,
STA |
yes |
no |
rt.SS,
bil.TS |
MMA,
middle meningeal artery; STA,
superior temporal artery;
CS,
caverous sinus; TS,
transverse-sigmoid sinus;
SS,
sigmoid sinus;
2. Endovascular treatment.
The techniques and treatment results of the six patients are summarized in Table 3.
Coil embolization of the affected sinus or fistulous pouch was performed in 4 cases wherein the isolated sinus was not a normal cerebral venous drainage route.
Sinus packing was performed in three patients via a transvenous approach through the occluded sinus (n=2),
or via a transarterial approach (n=1).
One patient underwent selective transvenous embolization of the shunted pouch combined with transarterial embolization.
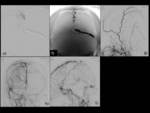
The SSS-DAVF disappeared immediately after treatment in 4 patients.
In 2 cases wherein the affected sinus received normal cerebral venous drainage,
selective transvenous embolization of the shunted pouches was initially attempted but failed due to poor maneuverability of the microcatheter/microguidewire caused by the occlusion of the transverse/sigmoid sinuses in addition to the SSS occlusion.
These 2 patients were then treated by transarterial embolization of the shunted pouches using a mixture of diluted (17%-20%) n-butyl-2-cyanoacrylate (NBCA) and lipiodol.
Angiography immediately after treatment showed that the SSS-DAVF had disappeared in 1 patient,
and was minimally residual in the other patient.
No complications were observed during and after the treatment in all patients.
Follow-up angiography and/or MRA showed no findings suggesting recurrence or reaggravation for 4~42 months (mean 13.2 months).
Table3: Treatments results
| |
Treatment |
Angiographic results |
Complications |
Recurrence/aggravation (follow-up months) |
| 1 |
Selective TVE + TAE (NBCA) |
disappeared |
no |
no (12months) |
| 2 |
Sinus packing (transvenous) |
disappeared |
no |
no (44months) |
| 3 |
TAE(NBCA) |
markedly regressed |
no |
no (4months) |
| 4 |
Sinus packing (transarterial) |
disappeared |
no |
no (6months) |
| 5 |
Sinus packing (transvenous) |
disappeared |
no |
no (30months) |
| 6 |
TAE(NBCA) |
disappeared |
no |
no (8months) |
TAE,
transarterial embolization; TVE,
transvenous embolization;
NBCA,
n-butyl-2-cyanoacrylate