ULTRASOUND TECHNIQUES
- Transabdominal US (TAUS) requires moderate bladder distention to create an acoustic window for the visualization of the vagina.
However,
transabdominal transducers,
which offer a wide field of view,
allow an extensive overview of the pelvic region but with a lower resolution than with transvaginal US.
- Transvaginal US (TVUS) is performed with the patient in lithotomy position and the patient’s bladder completely empty,
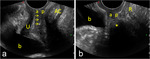
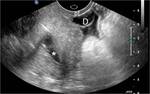
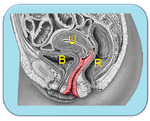
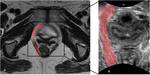
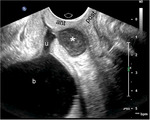
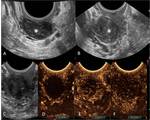
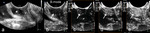
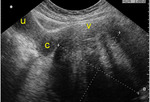
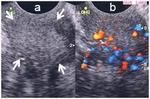
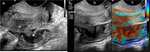
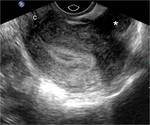
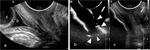
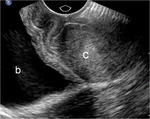
which brings the organs of interest closer to the higher-frequency transducer and improves image resolution Fig. 1 Fig. 2.
The major limitation in the assessment of the vagina with this technique is that the transducer is typically inserted into the anterior or posterior fornix prior to begin the examination,
which bypasses the perineum and the vagina.
For this reason,
it is essential monitoring the probe during its penetration in the vagina from the introitus to fornices in order to demonstrate any parietal lesions that otherwise could be missed.
- Translabial (TLUS) imaging has been firstly described in 1986 by Kohorn.
With the patient in litothomy position,
a high-frequency probe is applied directly on the perineum,
between the labia majora,
directly on the urethral meatus and the vulva Fig. 1 .
Ultrasound beam is directed upwards to visualize the hiatus of the pelvic floor and the pubo-rectal muscles,
and posteriorly to visualize both internal and external sphincters.
This approach allows for an accurate study of both the anterior (urethra and bladder),
median (vagina and uterus),
and posterior compartments (rectum and anus) of the pelvic floor; also,
connective tissues can be assessed.
In functional studies of the pelvic floor,
the exam must be performed with bladder replenished of urine,
both at rest and during Valsalva manoeuvre.
A video-loop registration can be useful to assess the urethral-vescical dynamic in relationship with others pelvic organs.
- Endoanal approach (EAUS) can be performed using endoanal linear probes.
However,
nowadays the use of this approach is extremely limited in vaginal studies,
because this kind of probes is no longer in commerce.
It is mostly used in gastroenterologic field by using endoanal rotating probes with 360 degrees vision for a high-resolution assessment of anal sphyncters.
- Three-dimensional Imaging (3DUS).
Volumetric evaluation allows for an acquisition of the entire volume of the middle compartment of the pelvic floor,
which can be later reformatted on different planes,
according to the relevant structure to assess.
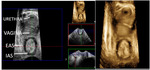
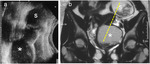
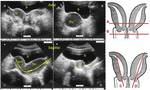
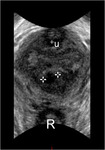
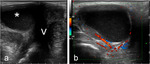
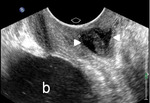
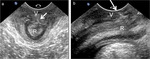
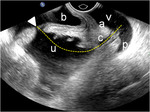
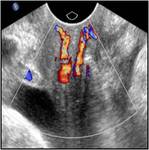
This allows for a precise evaluation of the parietal musculotendinous structures that are oriented along the plane of the pelvic floor Fig. 3 Fig. 4 .
- Contrast-enhanced ultrasound (CEUS) represents a valuable tool to assess tissutal vascularization.
The advent of microbubble contrast agents has provided the additional ability to obtain essential quantitative information relating to tissue vascularity with real-time acquisition,
tissue perfusion and even endothelial wall function.
The use of endocavitary contrast medium can also help to assess the presence of hidden fistulas.
- Real-time sonoelastography (RTE) is a recent US technique that enables assessment of tissue elasticity and has shown a clear potential for studying tissutal stiffness,
increasing diagnostic capabilities of B-mode US.
In general,
most productive lesions show increased stiffness because they have higher cell and vessel density compared with the surrounding normal tissue.
However,
the use of RTE software developed for the use with endovaginal probes is relatively recent.
NORMAL ANATOMY OF FEMALE PERINEUM
Female perineum is a diamond-shaped structure,
located inferiorly to the uro-genital diaphragm,
between the pubic symphysis anteriorly,
the inferior pubic rami laterally,
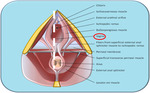
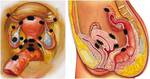
the coccyx and sacrotuberous ligaments posteriorly Fig. 5 Fig. 6 Fig. 7 :
- it is anatomically divided into two triangles,
one anterior (urogenital) and one posterior (anal),
by an imaginary line that joins the inferior pubic rami;
- the anatomic support to female perineum is warranted by the pelvic floor,
a complex structure that supports pelvic organs by muscular and fascial components.
NORMAL ANATOMY OF THE VAGINA
The vagina is commonly described as a fibromuscular sheath or tube extending from the vulvar vestibule to the uterus:
- located in the middle compartment of the pelvis;
- intimately related to the urethra and neck-trigone area of the bladder anteriorly and the anal canal and lower rectum posteriorly;
- its length,
configuration,
and position vary widely,
and its shape is determined by the surrounding structures;
- average length of 7–9 cm but can range from 4 to over 12 cm in length;
- the posterior wall is longer and ends in the posterior fornix; the shorter anterior wall ends in the anterior fornix.
ULTRASOUND ANATOMY OF THE VAGINA
At US,
the vagina is best demonstrated in the midline sagittal plane with a translabial approach.
An endovaginal 3DUS scan allows an high definition assessment of vaginal walls and related muscular structures with the possibility to obtain a multiplanar reconstruction of such findings,
thus allowing a systematic tomographic survey of any finding of interest. In females of reproductive age,
the normal vagina is seen as a collapsed,
hypoechoic,
tubular structure with a central high-amplitude linear echo representing the apposed surfaces of the vaginal mucosa.
A 3D acquisition allows for reconstructing of the pelvic floor US images on a pure axial plane,
thus demonstrating the vagina as a crescent-shaped hyperechoic linear structure (with anterior concavity) occupying the median compartment of the pelvic floor,
between the urethra anteriorly and the ano-rectal structures posteriorly.
In the axial plane,
urethra appears as a round anechoic structure between the posterior aspect of the pubis and the anterior vaginal wall; on a sagittal plane,
it originates from the lowest portion of the bladder and directs to vulvar vestibule.
Posteriorly,
the internal anal sphincter appears as a hypoechoic ring while the external sphincter appears as a ring of mixed echogenicity.
The mucosal folds are visible as structures of mixed echogenicity with a characteristic radiation from the central area (“star sign”).
CONGENITAL ABNORMALITIES OF THE VAGINA
Imperforate Hymen
- Hymen is a normally occurring membranous fold that fully or partially obstructs the external orifice of the vagina,
and its location indicates the junction between the urogenital sinus and sinovaginal bulb;
- imperforate hymen is the most common congenital obstructive abnormality of the female genital tract,
with a frequency that can vary from 1 case per 1000 population to 1 case per 10,000 population;
- most commonly occurs in isolation;
- occurs due to a failure of recanalization of this membranous vestige;
- variations in hymenal anatomy commonly are not detected until menarche,
when the patient presents with cyclic abdominal pain and primary amenorrhea Fig. 8 Fig. 9 ;
- when a complete imperforate hymen is present,
this condition is associated with the presence of hematocolpos, which is menstrual blood collection into the distended vagina and can be well depicted with trans-labial US;
- can be diagnosed at physical examination upon identification of a bulging,
bluish membrane that allows transillumination at the introitus.
Vaginal agenesis
- Vaginal agenesis occurs when the sinovaginal bulb does not form and is reported to occur in 1 in 5000 females;
- in the isolated form of vaginal agenesis with a normal development of secondary sexual characteristics and normally functioning uterus and ovaries,
patients develop hematometra and present with primary amenorrhea and severe cyclic pelvic pain;
- although it can be diagnosed at physical examination,
adjunct cross-sectional imaging is often performed,
especially in patients who present with a palpable abdominal mass;
- can be also associated with the presence of other abnormalities (40% urinary tract,
10-15% spinal tract,
25% acoustic deficits).
VAGINAL AND PARAVAGINAL CYSTS
Müllerian cysts
- Müllerian cysts are the most common benign cyst of the vagina,
accounting for up to 44% of cystic masses Fig. 10 Fig. 11;
- the most common location is along the anteriolateral aspect of the vagina; however,
these cysts can be located at almost any location within the vaginal walls;
- average 3 cm in size,
but can range from 1.4 to 7.0 cm in greatest dimension;
- smaller cysts are commonly present,
remain asymptomatic and never come to clinical attention.
Gartner Duct Cysts
- Gartner duct cysts are embryologic secretory retention cysts that arise from the residual wolffian (mesonephric) duct remnant Fig. 10 Fig. 11 Fig. 12 ;
- usually solitary and less than 2 cm,
most commonly develop in the anterolateral wall of the proximal one-third of the vagina;
- when located at the level of the urethra,
they can cause mass effect on the urethra,
giving rise to urinary tract symptoms;
- often associated with other wolffian abnormalities (unilateral renal agenesis,
renal hypoplasia,
and ectopic ureteral insertion);
- although usually asymptomatic,
cyst aspiration,
tetracycline sclerotherapy,
or surgical excision may be used to treat larger lesions.
Skene Gland Cysts
- Skene glands are paired structures located laterally the external urethral meatus (at 3 and 9 o’ clock positions),
with ducts draining directly into the urethral lumen Fig. 10 Fig. 11 ;
- retention cysts are caused by inflammatory obstruction of the paraurethral ducts;
- located inferiorly to the pubic symphysis;
- may be differentiated from urethral diverticula,
which tend to be midurethral in location Fig. 13 ;
- both Skene gland cysts and urethral diverticula are periurethral in location and,
due to their position,
may cause recurrent urinary tract infections or urethral obstruction;
- anechoic at US and CEUS with thin,
non-enhancing wall unless superimposed infection is present;
- usually asymptomatic but may require drainage or excision due to superimposed infection.
Epidermal inclusion cysts
- Epidermal inclusion cysts (also temed “sebaceous cysts”) are the most common type of non-embryological cyst Fig. 14 ;
- vary in size from a few millimeters to several centimeters;
- their location almost always correlates with a site of previous surgery and represents a traumatic inclusion of normal vaginal mucosa following vaginal laceration or episiotomy.
Bartholin Gland Cysts
- Bartholin’s glands secretions provide to lubricate vulvar vestibule with ducts that drain at the 4 and 8 o’ clock positions of the vaginal vestibule Fig. 10 Fig. 11 ;
- Bartholin gland cysts are the most common vulvar cysts,
developing in 2% of women during their lifetime;
- located at the posterolateral vaginal introitus,
medial to the labia minora;
- their location at or below the level of the pubic symphysis helps differentiate them from Gartner duct cysts;
- range in size from 1 to 4 cm (but can increase with repeated sexual stimulation develop as a result of an obstruction of the gland’s duct by a stone or a stenosis related to prior infection or trauma);
- patients are often asymptomatic but can present with mild dyspareunia,
typically in the 2nd to 3rd decade of life;
- superimposed infection or abscess formation may require drainage;
- a rare complication is development of squamous carcinoma or adenocarcinoma in a Bartholin gland duct or cyst,
respectively;
- at US,
simple cysts are anechoic,
thin-walled and unilocular,
but septations can be seen Fig. 15 ;
- the cyst wall may be thickened and,
if infected,
enhancement can be observed at CEUS examination;
- visualization of any solid component within the cyst should raise concern for malignancy.
SOLID MASSES
US and MR imaging allows the best differentiation between normal and abnormal vaginal structures.
US imaging can provide detailed depiction of solid masses that are not assessed at clinical examination.
However,
US imaging is not a fully adequate technique in the staging of pelvic malignancies,
not providing a comprehensive evaluation of the entire pelvis; for this reason,
MR is usually necessary to provide a topographic study of such pathology and can be used for vaginal tumor staging and surgical and radiation therapy planning.
Leiomyomas
- Leiomyomas are an uncommon entity in the vagina with only about 300 reported cases in literature;
- commonly seen in the age group ranging from 35 to 50 years;
- may originate in the smooth muscle of the vagina,
local arterial musculature,
or smooth muscle of the bladder or urethra; however,
midline of the anterior vaginal wall is the most common location;
- at US,
their characteristics are similar to uterine leiomyomas,
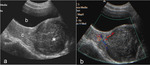
showing a heterogeneous but predominately hypoechoic and well circumscribed appearance Fig. 16 Fig. 17 Fig. 18 Fig. 19 ;
- at CEUS examination,
the enhancement of leiomyomas is uniform,
as opposed to the heterogeneous enhancement of leiomyosarcomas.
Primary Vaginal Malignancies
- Primary vaginal malignancies are relatively rare,
representing about 1%–2% of all gynaecologic malignancies and less than 20% of vaginal malignancies Fig. 20 ;
- primary cancers are defined as having no involvement of the external os of the cervix or the vulva inferiorly Fig. 21 ;
- The neoplastic patologies originated from rectovaginal septum,
the anterior wall of the rectum and from the muscles of the pelvic floor can simulate both the clinical and the imaging findings of a primitive vaginal malignancy Fig. 22 Fig. 23 ;
- the most common cancer of the vagina is squamous cell carcinoma,
representing about 80% of all primary vaginal malignancies:
- vaginal bleeding is the most common presentation;
- human papilloma virus infection,
age≥60 years and smoking
are considered risk factors;
- tends to spread early,
by direct invasion into the bladder and
urethra anteriorly and the rectum posteriorly;
- in more than half of the cases,
this type of cancer involves the
proximal vagina,
in one-third the lower vaginal tract and in
11% of cases the whole vagina.
- Non–squamous cell carcinomas account for 15% of all primary vaginal carcinomas,
including:
- adenocarcinoma (9%),
more commonly found in ≤30 year
women,
typically arises from the anterior aspect of the upper
vagina or rectovaginal septum,
superior to the perineum and
can be diffusely infiltrative,
lobulated,
or circumferential and
annular;
- melanoma (3%);
- sarcoma (1%).
Secondary vaginal pathology
- Secondary lesions of the vagina are more common than primary tumors and account for over 80% of all vaginal tumors;
- mostly occur by means of contiguous spread from adjacent cancers (vulva,
cervix,
endometrium and urinary bladder,
or anorectum);
- distant vaginal metastases may occur by means of lymphatic or haematogenous spread;
- the malignancies that most commonly metastasize to the vagina are ovarian,
cervical,
endometrial,
and rectal cancer;
- between the vaginal malignancies that are adenocarcinomas,
92.5% of lesions in the anterior wall of the upper third of the vagina arise from the upper genital tract,
whereas 90% of lesions in the posterior wall of the lower third arise from the gastrointestinal tract.
Vaginal cuff disease
- Vaginal cuff represents the apex of the vagina where the apposed upper walls are sutured together;
- is a site of recurrent gynaecologic malignancy after hysterectomy (seen most often with cervical carcinoma,
but it also occurs with endometrial cancer and rarely with ovarian cancer) Fig. 24 ;
- postoperative anteroposterior vaginal cuff size quoted in the literature is up to 2.1 cm;
- at pelvic US,
normal vaginal cuff is generally small,
symmetric,
and homogeneously hypoechoic;
- MR imaging is generally superior to US and CT in terms of diagnostic performance.
Vaginal endometriosis
- Vaginal endometriosis consists in the presence of ectopic endometrial glandular and stromal tissue within the vaginal walls Fig. 25 ;
- may occur during surgical procedures or from the spread of a recto-vaginal pouch endometriosis;
- often associated with dysmenorrheal,
postcoital spotting,
dyspareunia and infertility;
- the condition is almost always associated with endometriosis in other pelvic locations (especially retrocervical and rectal lesions) and may appear as nodular or polypoid masses involving the posterior vaginal fornix;
- the accurate diagnosis of vaginal endometriosis is especially important because a specific surgical procedure is required for treatment and because the condition is associated with a risk for rectovaginal fistulation;
- another site of endometriotic pathology can be found in the rectovaginal space (the region situated between the posterior vaginal wall and the anterior rectal wall below the peritoneal reflection);
- rectovaginal lesions are frequently extensions from retrocervical or posterior vaginal lesions and occur as firm nodules that can be palpated at vaginal examination;
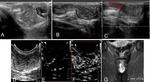
- US demonstrates uni- or multi-locular hemorrhagic cysts or with homogeneous low-level internal echoes Fig. 26 Fig. 27 Fig. 28 ;
- the use of US coupling gel into the upper third of the vagina provides distention of the posterior fornix and facilitates the identification of endometriotic hypoechoic nodules and thickening of the posterior vaginal wall;
- a small amount of fluid in the posterior cul-de-sac facilitates the identification of the peritoneal reflection (Douglas pouch).
VAGINAL FISTULAS
- Fistulas can form between the vagina and neighbouring urethra,
bladder,
or bowel Fig. 30 ;
- most often result from obstetric and surgical trauma,
radiation therapy for pelvic malignancy and inflammatory bowel disease;
- air,
fluid,
mucus or feces in the vagina may be present;
- almost half of small fistulas from obstetric trauma will heal spontaneously,
while the remainder require surgical repair;
- color-Doppler US with a microbubble contrast agent can help in the detection of the fistulous tracts Fig. 31 and,
in case of previous neoplastic lesion of the pelvis,
in determination of whether the surrounding tissue represents fibrosis or active tumor together with MR findings.
VAGINAL PROLAPSE
- Vaginal prolapse is the inward and downward bulging of the vaginal walls that occurs when the supporting tissues of the lower pelvis weaken;
- the risk increases with age,
as pelvic muscles weaken and natural reduction in estrogens at menopause also causes muscle to become less elastic;
- can also occur in case of a pedunculated uterine mass passing the cervical canal,
thus provoking a “glove finger” introflection of the uterus into the upper part of the vagina;
- uterovaginal prolapse affects about 50% of parous women (being 20% of them symptomatic),
and develops as a consequence of uterosacral ligaments lesions Fig. 32: in this condition,
the uterus descends into the vagina and can fall outside the vaginal vestibule (complete uterine prolapse) ;
- vaginal vault prolapse usually refers to an apical vaginal relaxation in a patient who underwent hysterectomy;
- continued descent of the vaginal apex results in complete eversion of the vagina.
VAGINAL VARICIES
- Vagina is an unlikely location to develop varices,
because of the presence of a bilateral draining system (similar to uterus),
which largely communicates with the uterine,
vescical and hemorroidal plexuses;
- vaginal varices are usually found in cirrhotic patients or after hysterectomy;
- color-Doppler US reveals venous flow inside these hypoechoic,
serpiginous lesions Fig. 33 .