Fields in 1991 proposed a classification of NP,
into four groups.
- Mononeuropathy: post-traumatic neuromas,
nerve root compression and idiopathic neuropathies as trigeminal neuralgia.
- Polyneuropathies: ischemic,
metabolic (diabetic neuropathy),
etc.
- Deafferentation pain: postherpetic neuralgia,
amputation neuromas phantom limb pain syndrome and central pain syndrome.
- Complex Regional Pain Syndrome type1 (Reflex Sympathetic Dystrophy –RSD-) and type 2 (Causalgia).
Another classification of NP is based on the location of the lesion:
- Central Nervous System:
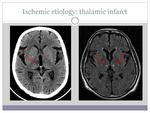
- Ischemic etiology : Central poststroke pain due to thalamic infarct (image 1)
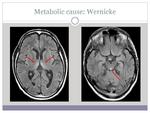
- Metabolic cause: Wernicke (image 2)
- Immunological diseases: Multiple Sclerosis (image 3),
AIDS.
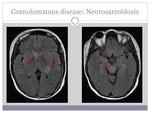
- Granulomatous diseases: sarcoidosis,
tuberculosis.
- Intrinsic and extrinsic compression: tumors,
meningiomas.
- Craneal nerves:
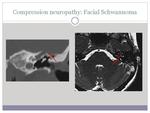
- Neoplastic disease: bening and malignant (image 5)
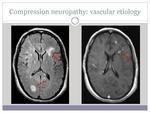
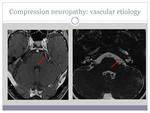
- Compression neuropathy (image 6)
- Peripheral nervous system:
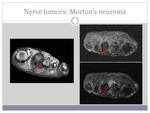
- Nerve tumors: Morton's neuromas (image 7),
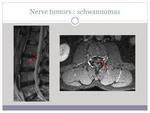
schwannomas (image 8),
traumatic neuromas,
etc
- Nerve root compression: herniated disc.
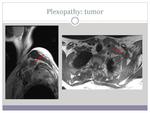
- Plexopathies (image 9).
- Systemic disease.
FUNCTIONAL IMAGING STUDIES
Application of new MRI techniques will play a very important role in the study of patients with neuropathic pain.
These imaging procedures include functional magnetic resonance (fMRI) performed with a blood oxygenation level-dependent (BOLD) sensitive T2*-weighted multislice gradient echo EPI sequence,
to establish the extent of cortical reorganization from face to hand area in motor and somatosensory representational maps.
Generally,
fMRI studies are based on the acquisition of images,
while the patient is at rest and while performing a specific cognitive,
emotional or sensitivo-motora task.
In this procedure the resonance signal changes depend on the concentrations of oxygen in blood,
fMRI is able to detect this change is due to a fundamental difference in the paramagnetic properties of oxyHb and deoxyHb.
When a specific region of the cortex increases its activity in response to a task,
the extraction fraction of oxygen from the local capillaries leads to an initial drop in oxygenated haemoglobin (oxyHb) and an increase in local carbon dioxide (CO2) and deoxygenated haemoglobin (deoxyHb).
Following a lag of 2 - 6 seconds,
regional cerebral blood flow (RCBF) increased,
delivering an surplus of oxygenated haemoglobin,
washing away deoxyharmoglobin.
Apparently,
the RCBF increase could be up to 50% in response to the increase in neural activity however,
the increase in oxygen consumption is much lower than the increase of the contribution through the blood.
So in venous phase (venous capillaries,
venules and veins) there is an elevated concentration of oxyhemoglobin (diamagnetic compound) with regard to deoxyhemoglobin (paramagnetic substance).
In addition this technique supposes an advantage because it do not require contrast administration for the study of brain activity.
With this technique Moseley (2006) demonstrated significant pain relief in patients with complex regional pain syndrome (CRPS).
Other autors have evaluated the relationship between cortical reorganization,
the various forms of pain in patients with phantom limb pain syndrome and the analgesic effect of mental imagery by fMRI; they demonstrated measured activation,
in the phantom limb area and explained it by a change in the excitability of cortical neurons previously responsive to functions involving the hand or arm only.
Tractography is performed using DTI and computer post-processing to track the fiber bundles which exist in the brain and spinal cord and visualize them as two and three dimensional images.
This technique is being studied to determine if neuropathic pain is associated with changes in regional brain anatomy and connectivity