The role of imaging is to establish the diagnosis and assist with the management of the disease,
namely in surgical planning.
Imaging can identify the primary tumors and can assess the location of the metastatic process (e.g.
identify if there is supramesocolic and/or inframesocolic involvement,
if there are signs of mesentery and omentum metastasis,
etc).
There are various patterns of peritoneal involvement and their knowledge allows the correct diagnosis.
Location:
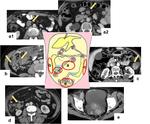
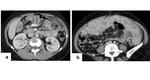
The main sites of growth of seeded metastasis follow the pathways of ascitic flow and are: the pouch of Douglas,
the small bowel mesentery,
the ileo-cecal junction,
the right and left paracolic gutters,
the hepatorenal fossa,
and the right subphrenic space (Figures 4 and 5).
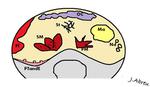
Two unusual sites of peritoneal carcinomatosis are the umbilicus and the ovaries; such metastases are respectively called Sister Mary Joseph’s Nodule and Krukenberg Tumors (Figure 6).
CT patterns of peritoneal involvement:
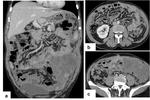
Carcinomatosis present with numerous CT tumors patterns (Figure 7),
which usually represent a continuum of disease spread and tumor burden.
These patterns include:
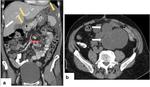
- Thickening and enhancement of peritoneal reflections (especially if nodular) (Figure 8);
- Peritoneal nodules,
plaques/sheets of soft-tissue that can progress to large masses (Figure 9 an 10);
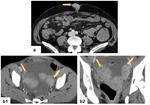
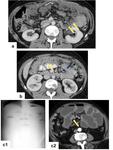
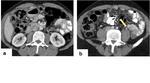
- Thickening,
stranding and distortion of the mesentery (Figure 11) ;
- Stranding and thickening of the omentum (omental cake) (Figure 12);
- Thickening and nodularity of bowell wall (Figure 13);
- Various amounts of ascites and degrees of lymphadenopathy may be present.
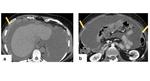
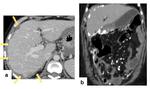
- On the liver surface subcapsular deposits indent the parenchyma,
described as “scalloping” (Figure 14) .
- The presence of calcification,
before treatment is instituted,
suggests mucin-producing primary tumor (Figure 14).
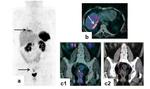
PET-CT findings of peritoneal carcinomatosis:
The glucose analog 18-F fluoro-2-deoxy-d-glucose (FDG) is used in FDG PET to show increased glycolysis in cancer cells and in activated WBCs in inflammatory and infectious processes.
- PET provides qualitative and quantitative metabolic information,
allowing assessment of disease extent and early detection of disease that may appear morphologically normal on CT.
- CT provides anatomic and morphologic information,
allowing accurate localization and clarification of physiologic uptake.
FDG PET/CT has been shown to have higher sensitivity in detecting peritoneal carcinomatosis than FDG PET and CT alone,
higher specificity than FDG PET alone,
and equal specificity to CT alone.
However,
FDG is a nonspecific tracer as it can be taken up by a variety of peritoneal processes.
Several FDG PET/CT patterns of peritoneal carcinomatosis have been reported.
PET-CT findings of peritoneal carcinomatosis include (Figures 15 to 18):
- single or multiple enhancing hypermetabolic peritoneal nodules;
- nodular thickening of the peritoneum with contrast enhancement and increased metabolic activity;
- ascites that may or may not be FDG avid.
CT mimics of peritoneal carcinomatosis:
There are several neoplastic and non-neoplastic conditions that may mimic peritoneal carcinomatosis on CT scan.
These include lymphomas,
granulomatous infections like tuberculosis,
and primary peritoneal malignancies such as mesotheliomas.
Lymphoma (Figure 19)
Peritoneal lymphomatosis may be seen on CT as omental caking or masses,
with diffuse peritoneal thickening or ascites.
Associated findings that may help in distinguishing lymphoma from peritoneal carcinomatosis include:
- splenic enlargement;
- aneurysmal dilatation of a bowel segment with a thickened wall;
- diffuse retroperitoneal and mesenteric lymphadenopathy - the enlarged lymph nodes appear as homogeneous attenuation or central low attenuation with peripheral rim enhancement,
sometimes forming masses causing encasement of the superior mesenteric artery and vein,
producing a ‘sandwich sign;’
- ascites without any loculation or septations.
Primary peritoneal mesothelioma (Figure 20)
Malignant primary peritoneal mesothelioma is rare and may have a variable appearance at CT:
- it is indistinguishable from carcinomatosis when the predominant imaging findings are multifocal peritoneal nodules and omental involvement ranging from finely infiltrated fat to omental caking;
- it is usually associated with ascites;
- it can be also seen as a irregular or nodular peritoneal thickening, a “stellate” pattern of the mesentery or bowel wall thickening;
- calcification is uncommon.
Ancillary findings to support the diagnosis of peritoneal malignant mesothelioma include the lack of evidence of a primary malignancy or metastasis elsewhere,
the lack of lymphadenopathy within the abdomen and when there is imaging or clinical evidence of asbestos exposure.
Peritoneal tuberculosis (Figure 21)
A high index of suspicion for peritoneal tuberculosis is important as it can be a difficult and elusive diagnosis to make.
The CT scan findings favoring the diagnosis include:
- omental cake-like masses;
- mesenteric macronodules;
- smooth peritoneum with minimal thickening and pronounced enhancement as compared to the nodularity seen in peritoneal carcinomatosis;
- presence of mesenteric and retroperitoneal adenopathy with low-attenuation centers (caseous necrosis) and calcifications.
- The fibrotic type of tuberculous peritonitis,
although not common,
is characterized by loculated ascites,
large omental masses,
and separation or fixation of bowel loops.