Many different extrapulmonary localizations of TB were observed: 59% at lymph nodes; about 13% involved the central nervous system (CNS); 10% at different vertebral levels (Pott’s disease) associated with paraspinal muscle abscess; 13% at abdomen (four cases characterized by bowel wall thickening and a case of renal TB); 26% of pericarditis (all but one accompanied by coexistent pleuropulmonary disease).
About 51% was Caucasian people (mean age of 67 years old),
49% non-Caucasian with lower mean age (32 years old).
About 49% of all our patients showed also pleuro-pulmonary TB.
We observed a different age incidence of extrapulmonary disease.
Young patients affected by extrapulmonary TB were represented mainly by immigrants.
Differently,
the older patients with extrapulmonary localizations were italian people.
Tuberculous lymphadenitis
Lymphadenitis is the most common extrapulmonary TB manifestation and it mainly involves cervical and supraclavicular lymph nodes; moreover inguinal,
axillary,
mesenteric or mediastinal involvement are possible too.
Typical lymph nodes imaging appearance is a central necrosis visible as a central low attenuation on CT scan.
This pattern,
however,
is not pathognomonic of TB since similar features may be seen also in metastasis,
lymphoma and inflammatory diseases.
Excisional biopsy with histology,
microbiological culture and biomolecular methods remain the goal procedure for definitive diagnosis.
Pott’s disease
Spinal TB accounts for about 50% of skeletal TB.
Typically more than one vertebral body is involved.
The lower thoracic and upper lumbar levels are most commonly affected.
The infection usually begins in the anterior part of vertebral body,
with the involvement of the intersomatic space.
Often vertebral erosion can result in anterior vertebral wedge deformation with consequent spinal sagittal deformities as kyphosis.
The infectious disease process can have an extension along the anterior or posterior longitudinal ligament.
Paraspinal involvement may include the psoas muscle,
with a psoas abscess (Fig.
1).
Calcification within the abscess is pathognomonic of tuberculosis.
CT and MRI are important to demonstrate small bone focus and extended disease.
CNS TB
Usually CNS damage is originated from an hematogenous spread,
but it may result also from rupture or an extension of a subependymal focus.
Infection may be located in brain,
meninges or spinal cord (meningitis,
meningo-encephalitis,
tuberculomas,
and abscesses).
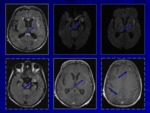
TB meningitis
TB meningitis (Figg.
2-4) is the most frequent manifestation among CNS TB manifestations.
The most typical radiologic appearance is a meningeal enhancement interesting basal cisterns,
the Sylvian fissure and cerebral sulci.
These findings can be detected on CT imaging but they are better seen on MRI examination with gadolinium.
Unfortunately this is a nonspecific appearance and it characterizes other infective meningitis or inflammatory diseases.
Complications of TB meningitis include:
- hydrocephalus,
caused by blockage of basal cisterns due to inflammatory exudates
- ischemic infarct,
particularly in the basal ganglia or internal capsule,
resulting from occlusion or compression of small perforating vessels.
Encephalitis
The encephalitis due to TB infection is a rare extrapulmonary localization associated with high morbidity and mortality.
Principal symptoms are fever and clinical signs of neurological deficits.
On MRI T2-weighted sequences often reveal a meningeal thickening caused from diffuse leptomeningeal inflammation.
Laboratory findings can show the presence of Mycobacterium tuberculosis in cerebrospinal fluid.
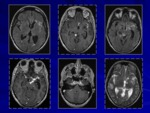
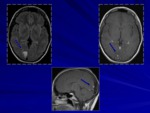
Cerebral tuberculoma
TB granuloma,
also known as tuberculoma,
is the most frequent intraparenchymal lesion among central nervous system forms of tuberculosis.
The most registered localization of tuberculomas is on frontal and parietal lobes.
Pathologically aspect of tuberculoma is a central caseation necrosis surrounded by a capsule of collagenous tissue.
Patients with cerebral tuberculoma (Figg.
2,
4,
5) can present sings and symptoms of raised intracranial pressure,
and focal neurological deficits.
On imaging we can observe single or multiple granulomas.
On MRI scan,
tuberculoma is hypointense on T1-weighted image with central variable signal intensity T2-weighted image according to the different types of granuloma (noncaseating granuloma,
caseating granuloma with a solid center,
caseating granuloma with a liquid centre).
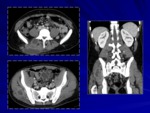
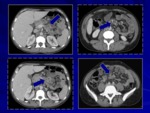
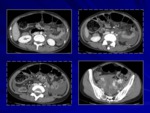
Abdominal TB
The abdominal localization of TB is case specific.
Patients can present various symptoms depending from localization.
The more common localizations are: lymphatic system,
genito-urinary system and digestive system.
Often symptoms are nonspecific and laboratory and instrumental features can suggest a neoplastic disease.
CT and MRI can detect lesions with a high grade of accuracy,
but often the final diagnosis request a pathological confirmation.
Abdominal TB (Figg.
6,
7) may involve the gastrointestinal tract,
peritoneum,
mesenteric lymph nodes,
and genitourinary tract.
The most common manifestation of abdominal disease caused by TB is represented by lymphadenopathy.
- gastrointestinal TB: thickening of cecum and terminal part of the ileum,
ileocecal valve enlarged,
and mesenteric lymphadenopathy;
- genital TB involves frequently the fallopian tubes in women,
with a bilateral salpingitis.
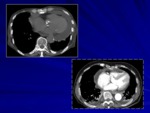
TB pericarditis
A first sign of pericardial involvement (Fig.
8) is represented by pericardial thickening (more than 3 mm).
CT can demonstrate thickened and irregular pericardium commonly associated with mediastinal lymphadenopathy.
We can also observe sometimes a distension of the inferior cava vein with more than 3 cm diameter.
Sometimes pericardial calcification can be seen.