Primary appendiceal neoplasms are rare.
With exception of carcinoid tumors,
most of them are seen in middle-aged or older patients.
Although other clinical manifestations are known,
approximately 30-50% of all appendiceal neoplasms will manifest as an acute appendicitis.
Other signs and symptoms include a painful palpable mass,
gastrointestinal bleeding,
ureteral obstruction or hematuria,
intussusception and increasing abdominal girth from rupture of a malignant mucocele,
resulting in pseudomyxoma peritonei.
Some of them are detected incidentally on imaging. Mucoceles that result from cystic mucinous neoplasms account for the majority of appendiceal tumors detected at imaging.
However,
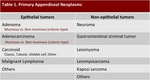
other types of tumors may occur an the radiologist must be aware of their existence (Table 1).
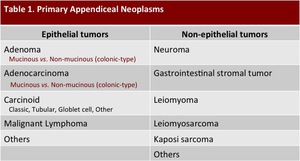

Table 1: Classification of primary appendiceal neoplasms.
In addotion,
detection of these neoplasms at preoperative imaging is also important because it may change the surgical treatment and obviate additional surgery.
APPENDICEAL EPITHELIAL NEOPLASMS
Epithelial neoplasms of the appendix may be benign or malignant (adenoma vs. adenocarcinoma).
Although these epithelial neoplasms are less common than appendiceal carcinoid tumors,
they are more likely to be detected at imaging due to their larger size and higher rate of complications.
It is useful to categorize these tumors as mucinous or nonmucinous epithelial neoplasms.
Mucinous Epithelial Neoplasms
Unlike the typical polypoid lesions that predominate throughout the colon and rectum,
the majority of epithelial tumors of the appendix are mucin rich,
showing a circumferential mucosal involvement and strong propensity to form mucoceles.
This term is used to describe an appendix distended by mucus,
it can represents either a benign or a malignant condition. However,
mucoceles resulting from nonneoplastic occlusion rarely exceed 2cm in diameter.
Mucoceles larger than 2cm are more likely to represent benign neoplasms,
if initially diagnosed as simple mucoceles (Fig. 1).
Mucinous neoplasms are also less likely to manifest with appendicitis than most other appendiceal neoplasms.
This fact may be related to the formation process of mucoceles that results from chronic luminal obstruction. Most benign mucoceles due to mucinous adenomas are relatively asymptomatic and are found incidentally at physical examination as a palpable mass or at abdominal imaging.
In opposition,
the majority of mucinous adenocarcinomas produce symptoms that lead to their diagnosis (Fig. 2, Fig. 3,
Fig. 4,
Fig. 5).
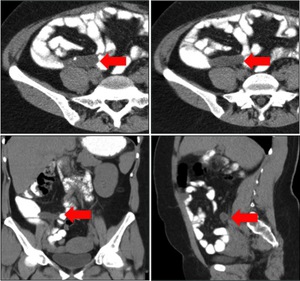
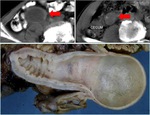
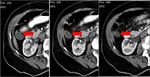
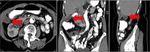
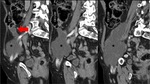
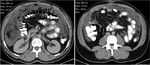
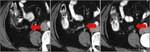
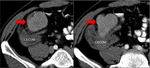
Fig. 2: Mucocele from mucinous adenocarcinoma of the appendix. Axial CT scan shows an elongated cystic mass (red arrow) in the expected region of the appendix, which measures 46x18x14mm. An eccentric calcification is seen. Coronal and sagital CT images show the same radiological findings (red arrow).
Clinical manifestations may have malignant causes such as direct invasion of the adjacent organs or increasing abdominal girth from tumor extension into the peritoneal cavity,
known as pseudomyxoma peritonei.
The term pseudomyxoma peritonei describes intraperitoneal diffuse accumulation of gelatinous material,
but is also used to describe localized collections from rupture of a benign mucocele. The diffuse form involves proliferation of viable neoplastic cells throughout the peritoneum and implies a malignant cause.
Although pseudomyxomas usually arise in the peritoneal cavity,
they may occur in the retroperitoneum. Both are typically insidious,
with a 5-year survival rate of 65%.
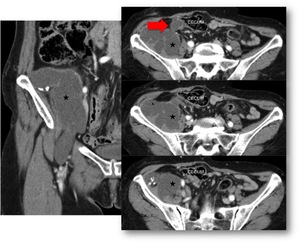
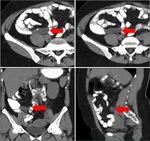
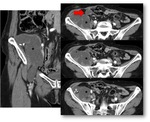
Fig. 7: Pseudomyxoma retroperitonei from mucinous adenocarcinoma of the appendix. Axial and coronal contrast-enhanced CT scan show an enlarged appendix with diffuse wall thickening (red arrow) and a lobulated hypoattenuating mass with tiny wall calcifications. The mass is observed in the right retroperitoneal space and displaces the adjacent structures, infiltrating the right iliac muscle (black star). Note the mass extension into the right crural canal. A CT guided biopsy confirmed the diagnosis.
Cross-sectional imaging is useful for evaluating the full extent of the tumor.
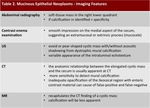
Typical imaging features of mucinous epithelial neoplasms are described below (Table 2).

Table 2: Imaging features of mucinous epithelial neoplasms of the appendix.
On the other hand,
atypical imaging features may reflect malignancy,
secondary complication or a pathologic variant.
Soft-tissue thickening and irregularity of the mucocele wall surrounding fat are findings that suggest malignancy or inflammation.
Intraluminal gas or an air-fluid level within a mucocele are diagnostic for infection.
Intussusception into the colon is an uncommon but known manifestation of appendiceal mucoceles.
Myxoglobulosis is a rare mucocele variant consisting of multiple intraluminal spherules,
specially identified on radiograms or TC when they calcify.
Pseudomyxoma retroperitonei is caused by the rupture of a mucinous lesion in the retrocecal appendix and fixation of the lesion to the posterior abdominal wall (Fig. 6, Fig. 7, Fig. 8).
A more significant group of patients with mucinous adenocarcinoma will present with slowly increasing abdominal girth from pseudomyxoma peritonei caused by mucocele rupture or transmural extension (Fig. 9).
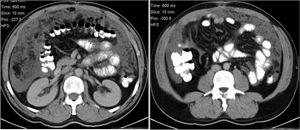
Fig. 9: Pseudomyxoma peritonei from mucinous adenocarcinoma of the appendix manifesting as increasing abdominal girth. Axial CT scan shows intraperitoneal mucin.
Typical imaging features include widespread heterogeneous peritoneal locules that displace and distort the hollow viscera or produce a scalloping effect on the solid organs.
Benign mucinous tumors are cured with appendectomy. If resectable, malignant lesions require right hemicolectomy.
Treatment of pseudomyxoma peritonei usually consists of surgical debulking with appendectomy,
omentectomy,
and oophorectomy (in women).
Intraperitoneal chemotherapy may be applied.
Nonmucinous Epitelial Neoplasms
The nonmucinous adenomas and adenocarcinomas that are characteristic of colorectal neoplasia rarely occur in the appendix. They tend to manifest clinically with appendicitis,
related to malignant luminal obstruction or because of the direct invasion of adjacent organs.
The majority of cases detected at imaging will be malignant,
usually in the setting of suspected appendicitis in an older individual.
At CT a focal soft-tissue mass involves the appendix but demonstrates no mucocele formation (Fig. 10,
Fig. 11). A subtle infiltrative appendiceal mass withsurrounding periappendiceal inflammation may be mistaken for nontumoral appendicitis.
APPENDICEAL CARCINOID NEOPLASMS
Classic Carcinoid Tumors
Classic carcinoid tumors of the appendix derive from subepithelial neuroendocrine cells and may represent up to 80% of all appendiceal neoplasms. They are often seen in young adults.
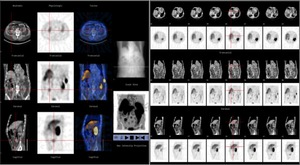
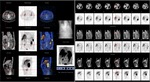
Fig. 13: Neuroendocrine tumor (classic carcinoid) of the appendix. SPECT detected pathological emitted radiation in in the expected region of the appendix.
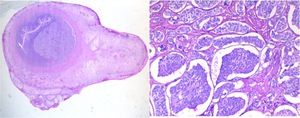
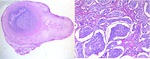
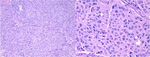
Fig. 14: Neuroendocrine tumor (classic carcinoid) of the appendix. Hematoxylin and eosin stain. Low power magnification view and 200x magnification view.
Unlike with most other primary appendiceal neoplasms,
find these neoplasms at surgery or pathologic examination is more challenging. Most of them ar discovered in the distal third of the appendix and are less than 1cm in size.
Therefore,
even in the setting of acute appendicitis,
a coexisting carcinoid tumor is the obstructing cause in only 25% of cases.
It remains unclear why the appendix is the most common site for gastrointestinal carcinoid tumors and why these tumors demonstrate a uniquely indolent clinical course in this location compared with other gastrointestinal carcinoid tumors.
Although all carcinoid tumors are considered potentially malignant,
metastatic disease and carcinoid syndrome rarelly occur when the primary site is the appendix. Studies have shown that tumor size correlates well with prognosis.
The relative paucity of imaging findings in the majority of appendiceal carcinoid tumors reflects the typical small size,
confinement to the distal appendix and low complication rate of these tumors (Fig. 12,
Fig. 13,
Fig. 14).
A symptomatic obstructing carcinoid tumor near the base of the appendix will usually manifest at CT or US as appendicitis.
The tumor may not always be appreciated,
unless if it has sufficient size or demonstrates calcification. Mucocele formation can occur but is a rare finding.
Appendiceal carcinoid tumors sometimes demonstrate a diffuse infiltrative pattern that manifests as diffuse mural thickening.
Although rare,
metastatic disease has CT features similar to those of small bowel carcinoid tumors.
An irregular soft-tissue mass near the root of the mesentery is characteristic.
Simple appendectomy is sufficient for treatment of most carcinoid tumors less than 2cm in size.
Greater tumors should be considered malignant and generally require right hemicolectomy.
Tubular Carcinoid & Goblet Cell Carcinoid Tumors
Tubular carcinoid tumors are rare histologic variants of classic carcinoid tumors.
They are seen in younger patients,
tend to be small,
localized to the appendiceal tip and have a good prognosis.
Goblet cell carcinoid tumors are uncommon and are nearly exclusive to the appendix.
They represent an entity intermediate between adenocarcinoma and classic carcinoid tumor.
Cross-sectional imaging findings will typically reflect the infiltrative nature of the tumor,
with often mild but diffuse mural thickening.
The propensity of advanced tumors to metastasize to the ovaries and peritoneum has been demonstrated.
Tubular carcinoids can generally be treated as classic carcinoid tumors.
Globlet cell carcinoid tumors are considered a low-grade malignancy and therefore most patients will undergo right hemicolectomy.
APPENDICEAL LYMPHOMA
Although the gastrointestinal tract is the most common site for extranodal non-Hodgkin lymphoma,
appendiceal lymphoma is rare.
The most common clinical manifestation is acute appendicitis,
which may be the only indication of disease.
According to the literature,
all reported cases of appendiceal lymphoma have proved to be non-Hodgkin lymphoma.
On imaging,
appendiceal lymphoma demonstrates as a prominent enlargement of the appendix with relative maintenance of its vermiform appearance.
If its blind ending nature is not noted,
the abnormal appendix can be mistaken for an abnormal small bowel loop or an extraintestinal process such as lymphadenopathy.
Diffuse mural thickening is typically hypoechoic at US and has soft-tissue attenuation at CT.
On US,
they can mimics the appearence of appendicial mucoceles.
Significant dilatation of the appendiceal lumen may be an important associated finding.
OTHERS APPENDICEAL NEOPLASMS
Rarely ganglioneuromas and paragangliomas of the appendix may occur.
Appendiceal mesenchymal tumors are also rare and typically benign.
Smooth muscle tumors involving the appendix have been reported.
Leiomyomas affect the appendix more often than leiomyosarcomas,
in opposition to the remainder colon.
Neurofibromas and schwannomas also rarely arise in the appendix.
Recently,
however,
it has been suggested that gastrointestinal stromal tumors may represent the most common mesenchymal tumor of the appendix.
It is likely that many of the appendiceal smooth muscle tumors reported in the older literature would be reclassified as gastrointestinal stromal tumors at modern immunohistochemical analysis.
Kaposi sarcoma of the appendix has been reported in patients with acquired immunodeficiency syndrome.
Other subtypes of sarcoma may rarely occur in otherwise healthy individuals (Fig. 15, Fig. 16,
Fig. 17).
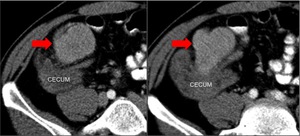
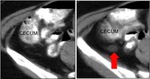
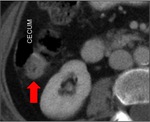
Fig. 15: Follicular Dendritic Cell Sarcoma. Axial contrast-enhanced TC scan, performed in a patient with a palpable mass and with right lower quadrant pain, shows a solid mass near to the cecum, which infiltrates its lumen. The patient undergone to laparotomy and the pathological analysis revealed a follicular dendritic cell sarcoma of the appendix.
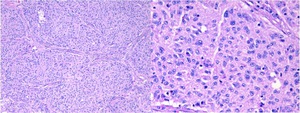
Fig. 16: Follicular Dendritic Cell Sarcoma infiltrating the appendix parenchyma. Hematoxylin and eosin stain. Magnification view of 100x and 400x.
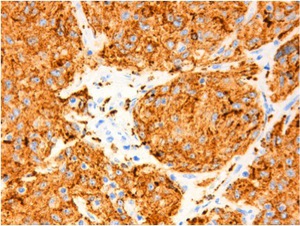
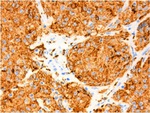
Fig. 17: Follicular Dendritic Cell Sarcoma. The neoplastic cells are immunoreactive with staining for CD68 (PGM1).