Our data review of 1627 patients yielded a total of 73 that matched all the inclusion criteria.
Of those,
44(60%) were women and 29(40%) were men.
The average age at presentation was 64,
with extreme ages of 25 and 98 respectively.
Our data showed a peak incidence of ischemic stroke in the 8th decade.
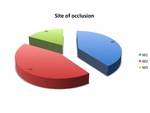
According to the site of occlusion of the MCA (M1,
M2 or M3) the study population was divided in three groups:
M1 occlusion was identified in 29(40%) patients,
M2 occlusion in 31(43%) patients and M3 occlusions in 13(17%) patients.
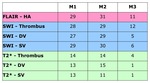
In our study we found that for M1 occlusion,
SWI and FLAIR provided excellent sensitivity for a confident diagnosis of acute ischemic stroke even in the absence of positive DWI findings.
HA in FLAIR and HSV in SWI were identified in 29 patients (100%),
while hypointense thrombus in SWI was found in 28 patients (96,5%).
Hypointense deep veins (HDV) in SWI were also identified in 27 patients (93%).
In M2 occlusion we noted slightly diminished but still excellent sensitivity for all signs in SWI (Thrombus visualization - 29 (94%),
HDV - 29 (94%),
HSV - 30 (97%),
while HA in FLAIR were identified in all of the 31 patients (100%)
In the 13 cases of distal M3 occlusion we found hypointense thrombus visualization in SWI to be the most reliable sign - 12 out of 13 patients (92%) followed by HA in FLAIR for 11 of the 13 patients (85%).
In all three categories of patients the T2* sequence was used to identify the same signs found in SWI (Hypointense thrombus,
HSV and HDV).
We found that on average,
T2* was not nearly as sensitive as SWI for these signs.
In T2* sequences we only identified signs in 14 patients (48%) for M1 occlusions,
in 15 patients (48%) for M2 occlusion and for only 4 patients (31%) in M3 occlusion.
We selected one representative patient for each of the three groups to better depict situations encountered in routine practice where the signs we studied played a definitive or supporting role in the diagnosis of acute ischemic stroke.
Patient 1 - M1 occlusion
(fig.
10,
11)
46 years old female patient admitted for persistent right upper extremity paresis,
aphasia and disarthria.
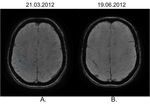
Patient underwent MRI exam one hour and thirty minutes after symptom onset.
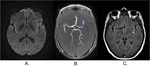
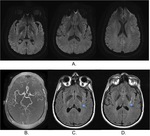
Diffusion weighted imaging showed no abnormality while TOF demonstrated clear occlusion of distal portion of M1 segment with flow absence in the left MCA territory (fig 10 A.
and B.).
NIHSS at admission: 15
FLAIR imaging shows linear hyperintensity in the subarachnoid space of the left sylvian fissure corresponding to retrograde arterial slow flow in the ischemic territory,
via leptomeningeal collaterals,
distal to occlusion(3),(4).
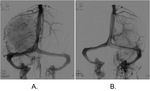
The hemodynamics are easily appreciated on digital subtraction angiography (fig.
17)
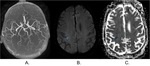
In this case SWI and T2* imaging has a supportive role to TOF and FLAIR.
While we can identify thrombus and hypointense superficial and deep veins on T2* imaging,
SWI better depicts thrombus size,
morphology,
while providing better visualization of superficial and deep veins(fig.
11) due to the fact that it has higher spatial resolution compared to T2*.
It has been shown that superficial and deep veins hypointensity in T2* and SWI is caused by the elevated oxygen extraction fraction due to slow flow in the ischemic region(5) but venous dilatation is also associated (fig.
18).
Final diagnosis for this patient was acute ischemic stroke consecutive to left M1 MCA occlusion.
Patient underwent combined thrombolysis and was discharged with a NIHSS of 4.
Patient 2 - M2 occlusion
(fig.
12,
13)
53 years old male patient admitted for sudden onset of right facial hemiparesis and right upper extremity paresis reversible in 30 minutes.
Patient had undergone combined thrombolysis for a right M1 occlusion a month before.
The stroke MRI was performed 1 hour after symptom onset.
NIHSS at admission: 2
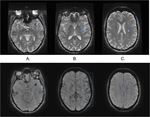
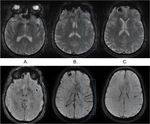
DWI identified no particular abnormality but TOF shows absence of flow in the posterior region of the superficial left MCA territory.
FLAIR shows hyperintense arteries in the region of TOF flow absence (fig.
12)
T2* and SWI shows hypointense thrombus in the M2 segment of the left MCA and hypointense superficial and deep medullary veins,
better depicted by the higher spatial resolution and sensitivity of SWI (fig.
13)
In this case,
information provided by FLAIR,
T2* and SWI was an important factor in deciding the diagnosis of acute ischemic stroke and consequent treatment.
Patient was administered i.v.
thrombolysis and discharged from hospital three weeks later with a NIHSS of 0.
Patient 3
(fig.
14,
15,
16)
67 years old patient admitted for sudden onset of left hand paresis reversible in 15 minutes. Patient had a NIHSS of 0 at admission and MRI was performed 3 hours after symptom onset.
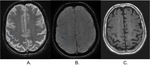
T2* shows discrete linear hypointensity in the right precentral sulcus confirmed by SWI (fig.
14).
The marked hypointensity in SWI suggests thrombus in the distal M3 segment of the right MCA.
FLAIR and TOF shows no evident abnormality but DWI and ADC confirms focal acute ischemic lesion in the precentral region,
adjacent to thrombus location (fig.
15)
The patient was discharged 6 days later with an NIHSS of 0.
Three months later a control MRI study was performed which showed absence of thrombus previously visualized and cortical microhemorrhage due to opening of the blood-brain barrier.